Much like smear tests, when women reach a certain age, mammograms become a regular part of their life.
But for someone who has never been for a breast screening before, the lead up to the examination can be a fraught time - and the fear of not knowing what happens might even be enough to put some women off.
To help put your mind at ease, Sue Oliver, Nuffield Health's head of mammography and laser safety, has explained the entire process and answered all of your burning questions including whether it hurts and how long the screening lasts.
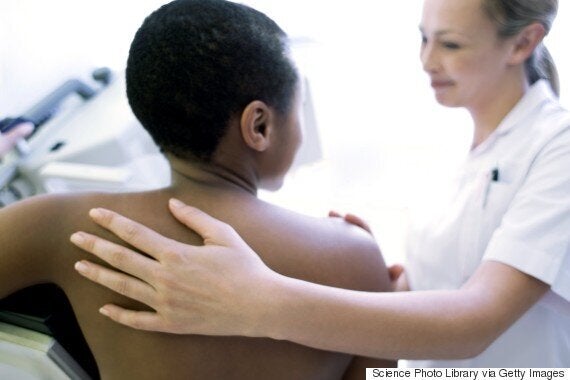
The NHS breast screening programme uses breast X-rays (mammograms) to screen all women in the UK aged 50 to 70 who are registered with a GP. They are sent an invitation to go for screening every 3 years.
Mammograms are often associated with breast cancer diagnosis, but they can also be used to detect and diagnose breast disease, a benign condition in which a woman has painful lumps in her breasts.
Oliver told HuffPost UK Lifestyle that most women, and even some men, will have many mammograms during their lifetime.
"Over time, people get more comfortable with breast screening, but your first one may invoke embarrassment, anxiety or even fear," she explained.
"Like so many medical investigations, mammography pushes the boundaries of what many people are comfortable with. But the reality is likely to be far less confronting than you might imagine."
Will I have to take my bra off?
"You will have to allow your breasts to be seen and even handled by a relative stranger. Take comfort from the fact that your mammographer is a professional, here to help and always female," explained Oliver.
Undressing to the waist is an essential step to getting a clear scan.
Any material other than breast tissue in the scan would obscure details and render the image useless.
"The mammographer will help position your breast correctly on the plate. This is essential to get the best quality image to help diagnose any issues," she added.
Will I be exposed to dangerous radiation?
Mammograms use X-rays to take detailed images of the breast tissue, which exposes the patient to a very low dose of radiation.
"Every exposure to radiation comes with a small risk, but it is much lower than the risk of not having the exam," explained Oliver.
"In a mammogram, the dose is roughly equal to the amount you'd be exposed to on a return flight from the UK to Australia - a journey many happily take with little concern about radiation."
SEE ALSO:
Graphic Images: Brutal Reality Of Breast Cancer Shown In Woman's Post-Radiation Therapy Photos
Will it hurt?
To get a clear scan, each breast needs to be held in place between two plates.
"The grip needs to be firm so there is no blurring of the image through movement," explained Oliver. "It may be uncomfortable and very rarely it may be painful."
She advised that if you do experience discomfort or pain, you should tell your mammographer right away and they'll do what they can to make you more comfortable.
What does the scan entail?
During a mammogram, each breast needs to be scanned twice, once from top to bottom and again from side to side.
"Each scan takes about one minute," said Oliver. "Once the scan is taken, the compression will automatically release and you'll be free to move away from the machine."
What happens next?
"Most women who come for a screening don't have cancer. Around 96 in every 100 women tested will get a normal result," explained Oliver.
"About four women will require extra tests but three of them will be given the all-clear. So chances are, even if something is discovered in the exam, it's not breast cancer after all."
She added: "Being aware of your own breasts and self-checking regularly is still the best defence against breast cancer.
"It can be a shock to discover a lump and it's natural for your mind to turn immediately to cancer.
"Any discovery should prompt a visit to your GP, but jumping to conclusions will only cause unnecessary concern."