
The pill remains the most popular method of prescribed contraceptive among women in England, new figures have revealed. Almost nine in 10 women in England who received contraception from the GP or pharmacies took either the combined pill or “mini pill” in 2017-18, figures obtained by the Guardian under the Freedom of Information Act showed, which equates to more than 3.1 million women.
This figure has remained steady in the past three years, despite a growing backlash against the pill. One study claimed that the combined contraceptive pill reduced the general wellbeing of healthy women, while another from 2016 said women who take the contraceptive pill are more likely to be treated for depression. Women have previously told HuffPost UK that the contraceptive pill left them with side effects such as poor mental health, skin flare-ups and mood swings, which left them turning to fertility apps instead.
For women, the pill isn’t the only option - and we certainly shouldn’t treat it like one. While condoms (and the female condom) remain the only way to protect against STIs, there are many more options of effective contraception to consider to prevent unwanted pregnancy.
It’s clear we need more research and resources invested into the issue, but in the meantime we reached out to FPA and the British Pregnancy Advisory Service (BPAS) to outline the pros and cons of 13 temporary methods of contraception, in order of effectiveness.
Contraceptive Implant (99.9% Effective)
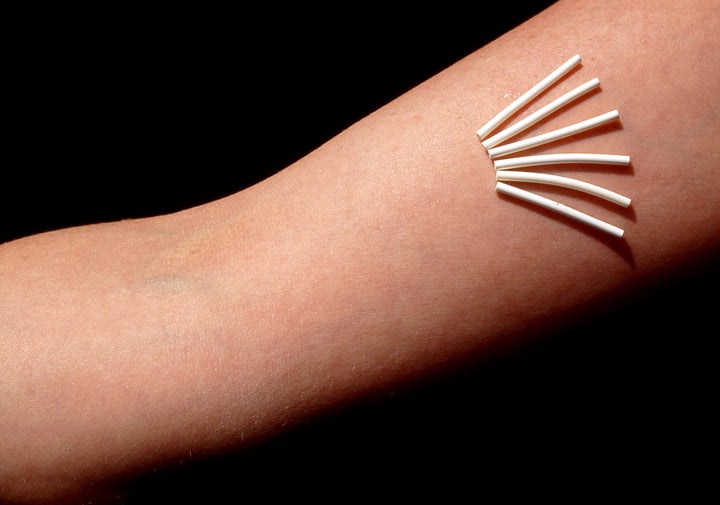
The implant is about the size of a thin matchstick and is inserted under the skin of the upper arm using local anaesthetic. It contains the hormone progestogen, which prevents the ovary from releasing an egg and thickens the cervical mucus (also known as discharge) to act as a barrier to sperm.
Pros
:: Once fitted you don’t have to think about contraception and it does not interfere with sex.
:: It lasts for three years but can be removed at any time by a doctor or nurse and normal fertility will return.
:: It offers highly effective protection against pregnancy. If implanted correctly, it’s more than 99% effective.
:: It’s useful for women who know they don’t want to get pregnant for a while.
:: It’s useful for women who can’t use contraception that contains oestrogen and for those who find it hard to remember to take a pill daily.
Cons
:: At first, you may feel some bruising, tenderness or swelling around the implant.
:: In the first year after the implant is fitted, your periods may become irregular, lighter, heavier or longer - although this usually settles down after the first year.
:: A common side effect of the implant is that your periods stop completely.
:: Some medications can make the implant less effective. Therefore additional contraceptive precautions need to be followed when you are taking these medications.
IUS (99.8% Effective)
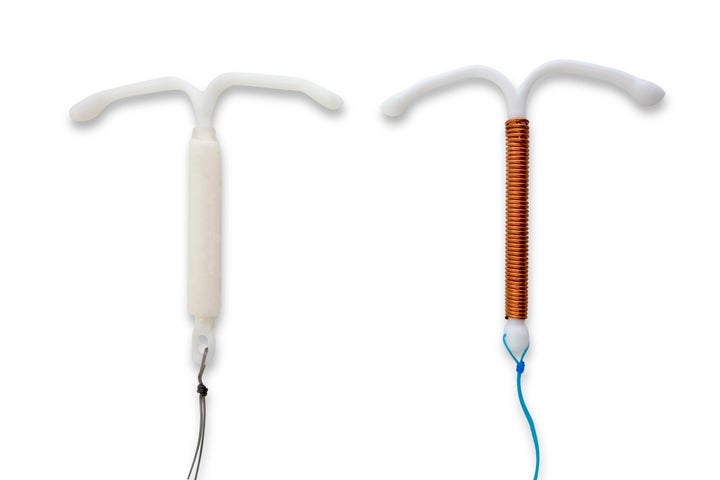
An IUS is a small plastic T-shaped device that continuously releases a small amount of the hormone progestogen, which interferes with implantation and thickens cervical mucus to act as a barrier to sperm.
It requires a simple procedure, carried out by a doctor or nurse, to insert it into the uterus. Two brands of IUS used in the UK are Mirena and Jaydess.
Pros
:: Once it has been fitted you don’t have to think about contraception and it does not interfere with sex.
:: Periods may become lighter or stop altogether.
:: It lasts for up to five years but can be removed at any time by a doctor or nurse and normal fertility will return.
:: It isn’t affected by any other medicines.
Cons
:: You may experience unpredictable bleeding in the first few months of use.
:: There is a low risk of an ectopic pregnancy, but only if you happen to become pregnant while using an IUS - which is very unlikely. “Although the risk is low, if you are using an IUD or IUS and you think you might be pregnant and/or have a sudden or unusual pain in your lower abdomen, you should seek medical advice as soon as possible,” the CEO of FPA, Nikita Halil, tells HuffPost UK.
Intrauterine Device / IUD / Coil (99.2% Effective)
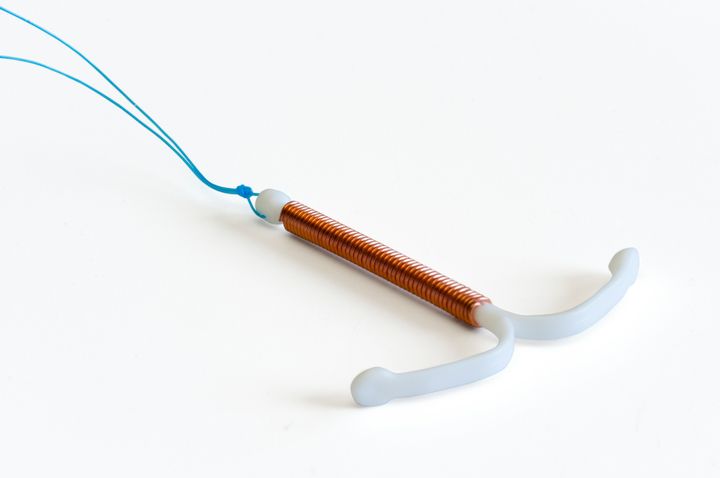
An IUD is a small, T-shaped piece of flexible plastic and copper that is fitted inside the uterus by a doctor or nurse. The copper is toxic to sperm.
Pros
:: Once fitted you don’t have to think about contraception and it does not interfere with sex.
:: It can be left in place for up to 10 years but can be removed at any time by a doctor or nurse and normal fertility will return.
:: It’s suitable for people who are unable to use hormonal methods.
:: It isn’t affected by any other medicines.
:: An IUD can also be used as emergency contraception and is more effective at preventing pregnancy than taking an emergency pill.
Cons
:: In contrast to the IUS, periods may become heavier, longer or more painful. However, according to FPA, this can improve after a few months.
:: There is a low risk of an ectopic pregnancy, but only if you happen to become pregnant while using an IUD.
Contraceptive Injection (94% Effective)

An injectable form of the hormone progestogen, which prevents the ovary from releasing an egg.
The injection is another long-acting method which lasts for 13 weeks. It’s highly effective if you use it according to instructions and always have your next injection at the right time.
If you don’t always do this then it’s less effective – the way it’s typically used means around six in 100 injection-users become pregnant in a year.
Pros
:: It does not interfere with sex and you don’t have to think about contraception for three months after injection.
:: It may reduce heavy painful periods and help with premenstrual symptoms for some women.
:: It isn’t affected by any other medicines.
Cons
:: It can cause unpredictable bleeding, however periods usually become lighter or stop altogether.
:: You may experience weight gain with this method, but not all women do.
:: The injection takes 12 weeks to leave the body if side effects do occur.
:: It can take up to a year for fertility to return to normal after using it, which means it’s not suitable if you want to get pregnant in the near future.
Combined Pill / The Pill (91% Effective)
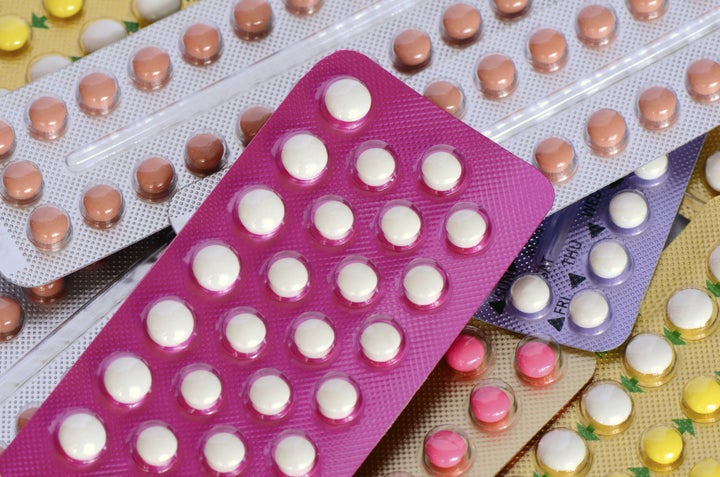
The pill is made of synthetic hormones similar to those found naturally in a woman’s body. It works by preventing the ovary from releasing an egg.
“The combined pill is still one of the most commonly used methods of contraception and is often one of the few methods on offer from GP surgeries,” says Nakita Halil.
It must be taken daily to prevent pregnancy, at the same time of day.
Pros
:: It usually makes bleeds regular, lighter and less painful.
:: Studies have found that it reduces the risk of cancer of the ovary, uterus and colon.
:: Normal fertility returns as soon as you stop using it.
Cons
:: According to Halil, there can be a range of side-effects such as headaches, nausea, mood changes and breast tenderness.
:: It can have some serious side-effects in a small number of women, such as a blood clot, heart attack or stroke, but these aren’t common.
:: Missing a pill, vomiting or severe diarrhoea can make it less effective.
:: May not be suitable if you smoke and are over 35 years old.
:: Some types of medicine might make it less effective, including ones used to treat epilepsy, HIV and TB, and the complementary medicine St John’s Wort.
Mini Pill / Progestogen-Only Pill (91% Effective)

The progestogen-only pill (also known as the mini pill) is also taken at the same time, every day. Unlike with the combined pill, there is no seven-day break.
According to BPAS, there are two types of progestogen-only pills: both thicken the cervical mucus to prevent the sperm from reaching the egg, some also prevent the ovary from releasing an egg each month.
Pros
:: Unlike the combined pill, the mini pill doesn’t contain oestrogen so it’s useful for women who can’t use the hormone.
:: It can be used if you smoke and are over 35 years old.
:: It can help with premenstrual symptoms and painful periods.
:: It does not interfere with sex.
:: Normal fertility returns as soon as you stop using it.
Cons
:: It can cause irregular bleeding.
:: Missing a pill, vomiting or severe diarrhoea can make it less effective.
:: It must be taken at the same time every day to work properly.
:: Some types of medicine might make it less effective, including ones used to treat epilepsy, HIV and TB, and the complementary medicine St John’s Wort.
Contraceptive Patch (91% Effective)
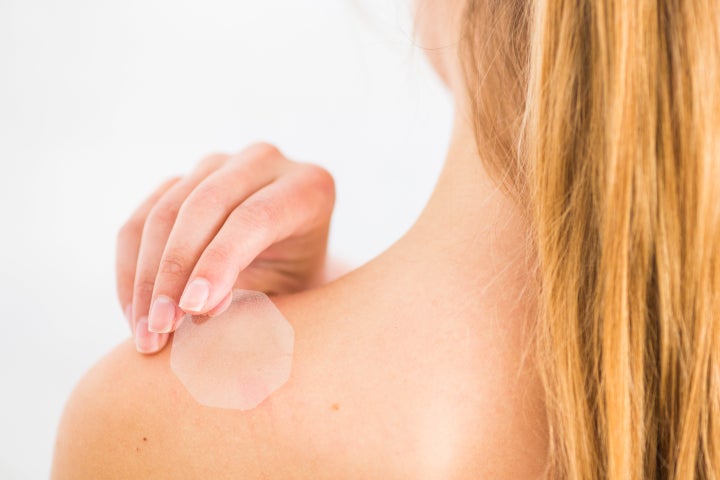
A lesser-known contraceptive, the 4cm square plastic patch sticks to the skin and releases hormones into the bloodstream.
Unlike the pill, which is taken daily, new patches are usually applied weekly.
Pros
:: It does not interfere with sex.
:: It is not affected by vomiting and diarrhoea.
:: Periods may become regular, lighter and less painful.
:: Normal fertility returns when you stop using it.
Cons
:: It may be seen on the skin or cause skin reactions.
:: It can fall off without you noticing.
:: May not be suitable if you smoke and are over 35 years old.
:: Some types of medicine might make it less effective, including ones used to treat epilepsy, HIV and TB, and the complementary medicine St John’s Wort.
Vaginal Ring (91% Effective)
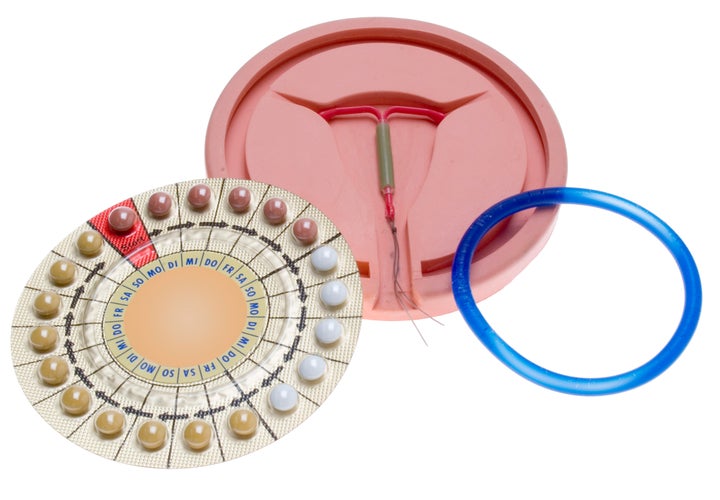
A flexible, transparent, plastic ring which a woman places inside the vagina herself (like a tampon). It is left in place for three weeks and then removed, at which point a woman will usually then have her period. One week later, users add a new ring and start the cycle again.
This method of contraception releases the same hormones used in the combined pill, which prevent the ovary from releasing an egg.
Pros
:: It does not interfere with sex.
:: You don’t have to have to think about it everyday.
:: It is not affected by vomiting and diarrhoea.
:: Periods may become regular, lighter and less painful.
:: Normal fertility returns when you stop using it.
Cons
:: It may not be suitable if you smoke and are over 35 years old.
:: In rare instances it may fall out during sexual intercourse or while straining during a bowel movement.
:: It has been associated with an increased risk of blood clots, stroke or heart attack. Anyone with a history of these conditions or any condition that makes your blood more likely to clot should avoid using it.
:: According to vaginal ring manufacturer NuvaRing, the most common side effects are: irritation inside the vagina or on the cervix, headache (including migraine), mood changes, the ring slipping out or causing discomfort, nausea and vomiting, vaginal discharge, weight gain, vaginal discomfort, breast pain or discomfort, painful menstrual periods, abdominal pain, acne and less sexual desire.
:: Some types of medicine might make it less effective, including ones used to treat epilepsy, HIV and TB, and the complementary medicine St John’s Wort.
Diaphragm And Cervical Caps (88% Effective)

Diaphragms are circular domes made of thin, soft latex or silicone with a flexible rim, while cervical caps are smaller and are made of latex or silicone. They are barrier methods of contraception, which means they prevent sperm and egg from meeting.
They fit inside the vagina and cover the cervix (the entrance to the womb).
Pros
:: You only need to use them when you have sex.
:: They have no serious health risks or side effects.
Cons
:: To be effective, diaphragms and caps need to be used with a spermicide. This can be messy to use and some people can be sensitive to it.
:: They come in different shapes and sizes, so you will need to see a doctor or nurse first to ensure it fits correctly.
:: You need to learn how to use it to cover the cervix properly.
Male Condoms (82% Effective)

”Male condoms (also known as external condoms) are still one of the most popular methods not least because they also help protect you from sexually transmitted infections and they are so widely available,” says Nikita Halil.
“People often don’t know that they come in a range of shapes and sizes and it’s worth experimenting to find one that feels good to you.”
Pros
:: They protect against sexually transmitted infections as well as pregnancy.
:: They are good for people who don’t want to use hormonal methods.
:: They aren’t expensive, are easy to access and you can often get them for free.
:: They come in different shapes, sizes and flavours, which can make sex more fun.
Cons
:: You have to interrupt sex to put one on.
:: It can split or slip off.
:: Oil-based products (like body oils, hand creams and vaseline) can damage the latex and make the condom more likely to split. So always use water-based lubricants.
Female Condoms (79% Effective)

”Female condoms are the only other method that help protect you from sexually transmitted infections,” says Halil.
“They’re not as popular or widely available as male condoms but are another choice if you can’t use hormonal methods.”
Pros
:: Unlike male condoms, they can be put in any time before sex.
:: They protect against STIs as well as pregnancy.
:: They’re a good choice for women who can’t use hormonal methods.
Cons
:: They can slip or get pushed out of place if they aren’t used properly.
:: They can be quite expensive to buy.
Withdrawal (78% Effective)

This method is where the man withdraws his penis from a woman when he feels he is going to ejaculate. He then ejaculates outside of her body.
Generally, experts advise against this method.
Pros:
:: You don’t need to visit a clinic or use any products.
Cons:
:: Some sperm can leak out of the penis before ejaculation.
:: It has a relatively high failure rate - around 22 out of 100 women relying on it will get pregnant in a year.
:: It requires lots of control and practice.
Fertility Awareness Methods (76% Effective)

This is when a woman identifies the most fertile phase of their monthly cycle using natural signs such as body temperature, cervical secretions and the length of their menstrual cycle.
During the fertile period, a couple will avoid sex or use another contraceptive method such as condoms.
Experts say you should only use natural family planning if you have been taught by a specialist. Every woman is different and natural family planning needs to be understood really well if it is going to be effective.
Pros:
:: There are no physical side effects.
Cons:
:: Some fertility awareness methods may be hard to use during fever or vaginal infection, after childbirth or while breastfeeding.
:: Some areas have limited availability of suitably trained healthcare professionals to teach this method.