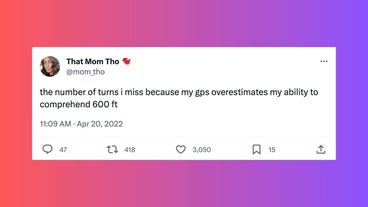
gps
"I love hearing someone blasting music out of their car and then the GPS directions pop off at full volume. YOU ARE ON THE FASTEST ROUTE!!!!!"
Mind is calling for better mental health training for GPs to help them cope with demand.
Do you know if you need to re-register with another practice?
69% said they experience a high level of demand for medical assessment letters
Scientists aren't sure how to deal with it. 🤔
If it ain't broke, don't fix it.
'Hopefully it's a big, but 'nice' bear.'