hospitals
Business secretary Alok Sharma leads the daily coronavirus briefing following the announcement that lockdown will continue for three further weeks. It comes as the number of people who died in UK hospitals nears 15,000 and the NHS could run out of gowns over the weekend.
“The complainers should have been stocked up and ready long before this crisis hit,” tweeted the president, who belittled the coronavirus pandemic for weeks.
For vulnerable mums and dads, phones are a source of friendship, support and lifesaving information.
The government have unveiled plans for 40 'new' hospitals to be built in the next decade.
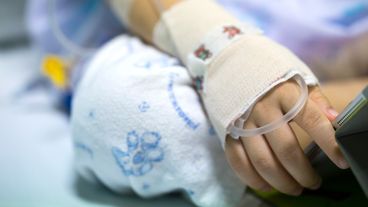
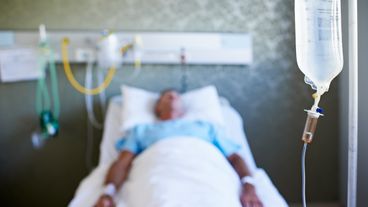
A lack of visitors can have a detrimental effect on patient recovery, nurses said.
"A hospital meal should be a small highlight, a little pleasure and comfort," says the chef.
One in 10 people in hospitals are alcohol dependent – yet researchers argue services and support for these patients are limited.
Three quarters of the best-selling items in hospitals are unhealthy, a study has found.
More than 18,500 surgeries were cancelled in England.
But the reason for the rise isn't so cut and dry.