More than 5,000 people were forced to wait more than an hour to be seen in emergency departments in England in the first week of the year, official figures show.
The statistics were released on Thursday, as the full extent of the strain on the NHS was laid bare and it was described as reaching a ”watershed moment” by one health boss.
More than 16,600 people had to wait more than half an hour in A&E departments, NHS England said, as staff are faced with rising numbers of flu cases and respiratory illness, with 48 flu-related deaths in England so far this winter.
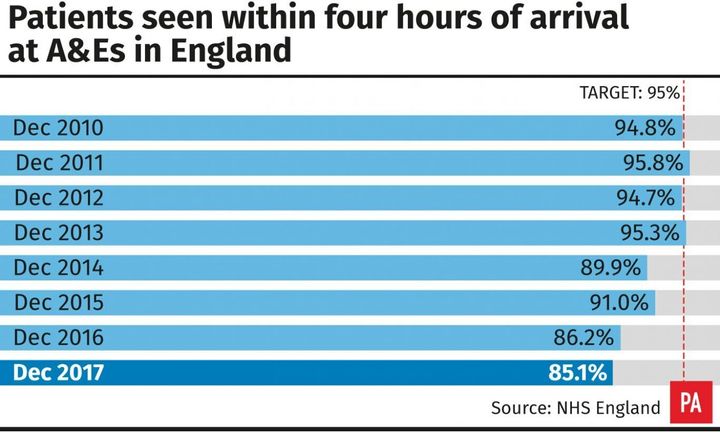
(PA Graphics)
A&E figures show that the NHS ended the year with the same performance level in December – 85.1% – as at the start of the year, equalling January’s record low.
The target of seeing 95% of patients within four hours has not been met since July 2015.
The Royal College of Surgeons said it was “disappointing” that just 77.3% of patients at major A&E departments were treated within four hours, worse than in December 2016 when 79.3% of patients were seen.
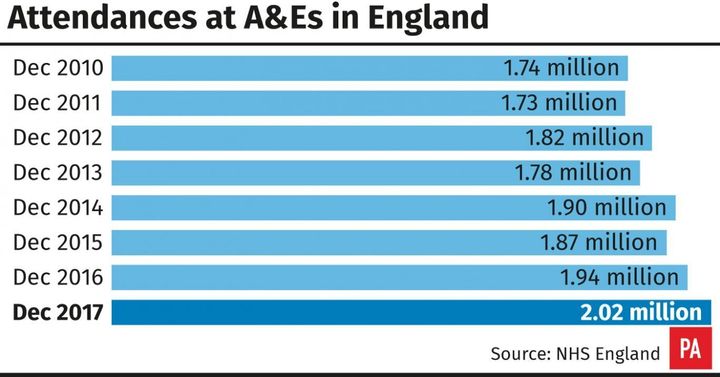
(PA Graphics)
A spokesman added: “It further demonstrates why it has been necessary to cancel patients’ non-urgent procedures until the end of January.
“Despite the best efforts and dedication of NHS staff to treat patients quickly, waiting times for non-urgent care have also deteriorated again in the past year.
“Last week, NHS England advised that hospitals defer non-urgent inpatient planned care until the end of January and that day-case procedures and routine patient appointments should also be deferred where this will release clinical time for emergency care.
“Although this should help relieve some of the pressures on hospitals and avoid last-minute cancellations, it is a short-term solution and will cause huge disruption to those patients whose appointments and operations have been cancelled.”
A letter written by the chief executive of NHS Providers – the trade body which represents NHS services – has called for the Government to commit to increasing the NHS budget to £153 billion by 2022/23.
Chris Hopson said investment on a long-term basis – and help with the immediate financial impact of ”exceptional winter pressures” – was needed to address the ”fragility of the wider NHS”.
Mr Hopson said: ”Despite planning for winter more thoroughly and extensively than before, it hasn’t been sufficient. Rising numbers of flu cases and more respiratory illness have placed intolerable pressures on staff.
”The NHS is no longer able to deliver the constitutional standards to which it is committed. We need to be realistic about what we can provide on the funding available.
”If we continue to run the NHS at close to 100% capacity, day in, day out, permanently in the red zone, it’s not surprising that the service can’t cope when we get a high, but entirely predictable, spike in demand.”
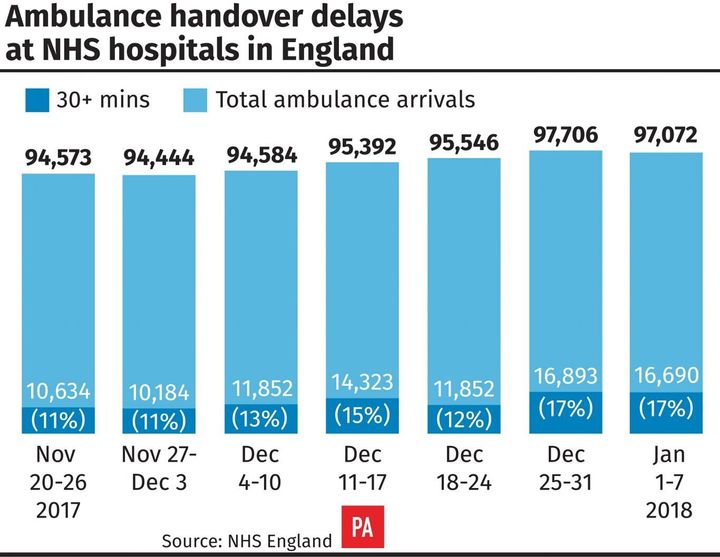
(PA Graphics)
NHS England said figures for delayed transfers of care – when a patient is ready to leave a hospital – were lower than at the same point for any of the past four years.
Glen Garrod, vice president of the Association for the Directors of Adult Social Services (Adass), said this was “evidence that putting extra funding into social care, as the Government has done this year, can bear fruit”.
“This also demonstrates the efforts of our resilient and highly dedicated frontline social care staff, who are doing a stellar job. Carers have been out in all weathers and recently have worked over the Christmas and New Year period, working hard to improve the lives of older people and adults of working age with disabilities,” he added.