Cheryl has issued a plea for increased awareness of Charcot-Marie-Tooth (CMT) disease, a debilitating condition that affects the child of one of her close friends.
Symptoms of CMT, including muscle weakness, uncontrollable pain, balance problems and difficulty walking, usually begin when a person is aged between five to 15 years old.
Cheryl urged her 3.6 million Instagram followers to learn more about the condition and the impact it has on kids, and Karen Butcher, chief operating officer at the charity Charcot-Marie-Tooth UK concurred that simply making the condition common knowledge can make a positive impact on children’s lives.
“It’s important that children with CMT feel supported by everyone around them,” she told HuffPost UK.
“As some children with CMT can’t walk very well - and trip and fall a lot – they get bullied at school, so it’s really important to tell their peers all about the condition.”

“In addition, it’s important teachers also understand the challenges children with CMT face,” Butcher added.
“So that if a pupil with CMT is fatigued or in pain, they are aware that they aren’t being lazy or defiant and they can help them in the right way.”
What is CMT?
CMT is not a single disorder, but a group of neurological conditions that damage peripheral nerves.
These nerves are responsible for transmitting commands from the brain to the muscles, and for sending information to the brain about sensations, such as pain, heat, cold, touch and, importantly for balance, where your joints are in space.
It is rarely life-threatening but it is a progressive disease, meaning it may get worse over time, with sufferers’ hands, feet and legs growing weaker, leading to problems including hammer toes, restricted mobility, uncontrollable pain and some people end up wheelchair bound.
Tasks needing fine motor skills - such as fastening shoe laces - may also become very difficult.
Currently there is no cure and leading neurological expert, Professor Mary Reilly, estimates around 23,000 people in the UK have CMT, which is named after the three scientists who discovered it.
What are the symptoms of CMT?
The disease can affect people very differently, even in the same family.
But some symptoms are common to most types of CMT. These include: wasting, weakness and reduced sensation starting in the feet/legs and eventually involving the hands/arms.
Early symptoms to watch out for in your child include:
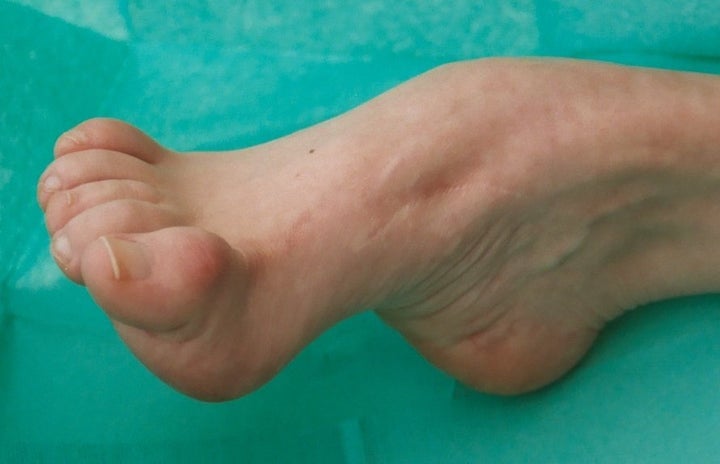
* Difficulty walking because of problems picking up the feet and high arches (or abnormally flat feet).
* Weakness in the feet, hands and forearms.
* Difficulty with running and general agility – including being ‘clumsy’.
* Trouble balancing, regularly tripping up or falling over.
None of these symptoms necessarily mean your child has CMT disease, so if you notice them it’s a good idea to speak to your GP about the condition.
“Early, accurate diagnosis can improve the lives of those with the condition as it can be managed more effectively,” explained Butcher.
“In addition, because CMT is genetic and there’s a 50% chance it can be passed on from a parent to a child, then professional genetic counselling can also be received so the risks to the next generation can be learned.”
What treatment is available?
At present there are no therapies that can halt the progression of CMT, but there are ways to manage many of the complications .
The right referrals to the right clinicians are crucial, according to Butcher.
“For example, physiotherapy can help people with CMT by strengthening their muscles, but some people still haven’t been referred and they can’t afford to go privately,” she explained.
“We know we aren’t the only group of people affected by NHS cuts, but they are impacting our members, as cost-conscious GPs fail to refer them to experts who could make real improvements to their quality of life.
“Thankfully, there are things that can be done for those with CMT, but they do need specialist care and advice.”
The charity advises specifically asking your GP about your child being referred to a specialist for current treatments to manage symptoms and complications, including: physiotherapy, orthotics, occupational therapy, pain and fatigue management and – when needed – orthopaedic surgery, speech therapy and respiratory support.
In July, The Lancet reported that ‘progressive resistance exercise’ proved beneficial in not only slowing the progression of muscle weakness but also increasing muscle strength.
Visit the CMT charity website for more info on accessing treatment.
What support is available?
“We have a youth group called CMT Kids that works with schools to raise awareness of CMT, particularly if there’s a child in the school with the condition,” explained Butcher.

“Likewise, we support families of young children with CMT and often put them in touch with other families who’ve been through the same thing or with medical professionals who can help them,” Butcher continued.
“In the office we’ve just designed a new publication called ‘If your child has CMT’ and parents can contact us for that.
“Our advice for parents of children with CMT is to remember that this is a life changing but not life threatening condition, so please try and let your child enjoy their childhood as much as they are able.
“There are varying extremes of CMT and obviously this condition can be really stressful for some families whose children are going through surgery or physical and emotional pain, but for many children with CMT it really is possible to live a normal life and they should be encouraged to join in as much as they can.”
Find out more at www.cmt.org.uk or contact 0800 6526316 or donate by visiting www.justgiving.com/CMT
