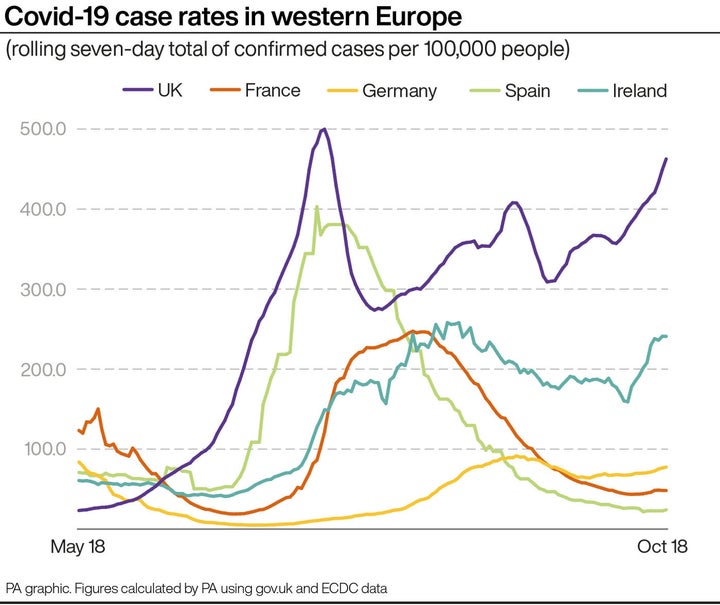
Britain’s Covid infection rate is starting to climb again, but the UK’s closest neighbours are seeing a much lower level of confirmed cases.
Cases among older people are seven times higher in Britain compared neighbouring European nations. Hospital admissions are six times higher while the death rate is three times higher.
This has left people seriously concerned.
In fact, the UK’s rate of confirmed cases is now one of the highest in the world.
But what’s causing this large disparity – and is there anything the UK can do to turn it around?
1. Fewer people are wearing masks in England
Masks are not obligatory in indoor spaces in England, although they are still mandatory in some circumstances in Scotland, Wales and Northern Ireland.
Face coverings do reduce Covid transmissions significantly but Downing Street stopped them from being mandatory from July 19 – on Freedom Day – aside from in healthcare settings and care homes.
It’s a very different picture across the rest of Europe as masks remain in place in most indoor places.
Public health expert in Spain Alex Arenas told i newspaper: “Without a doubt, the combination of wearing masks and the fast vaccination programme has brought the coronavirus contagion rate down in Spain.”
2. Increased rate of indoor mixing
Mask-wearing is not solely responsible for impacting the Covid infection rate, though.
In Scotland the Covid infection rate is still quite high. ONS estimates 1 in 80 people there have Covid compared to 1 in 60 in England, despite having much stricter instructions around wearing the face coverings.
Both countries have seen a similar level of indoor mixing between large groups, which has in turn led to increasing infection rates.
3. Britain started vaccinating earlier
The UK stunned the world with its speedy vaccine rollout at the beginning of December 2020, beating many of its European neighbours who struggled to negotiate with vaccine companies as part of the EU.
However, this speediness could come back to hurt the British population as it means people will need booster jabs sooner rather than later – just as winter is approaching and people are more vulnerable.
After five months, Covid vaccine protection starts to drop off.
According to the Financial Times’ journalist John Burn-Murdoch around 75% of older people are five months’ after their second dose, making them more vulnerable to infection.
Pfizer is also known to provide more long-lasting protection for its recipients. The UK used Astra-Zeneca more widely than other European nations towards the start of the vaccine rollout, as many in the EU were concerned about potential blood clots.
4. The vaccine rollout has become sluggish
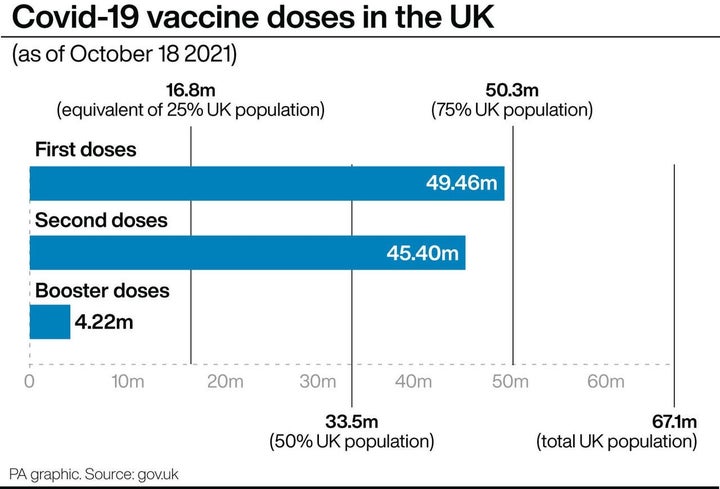
More than 49 million people in the UK – meaning almost nine in 10 people aged 12 and above – have had at least one dose of the vaccine.
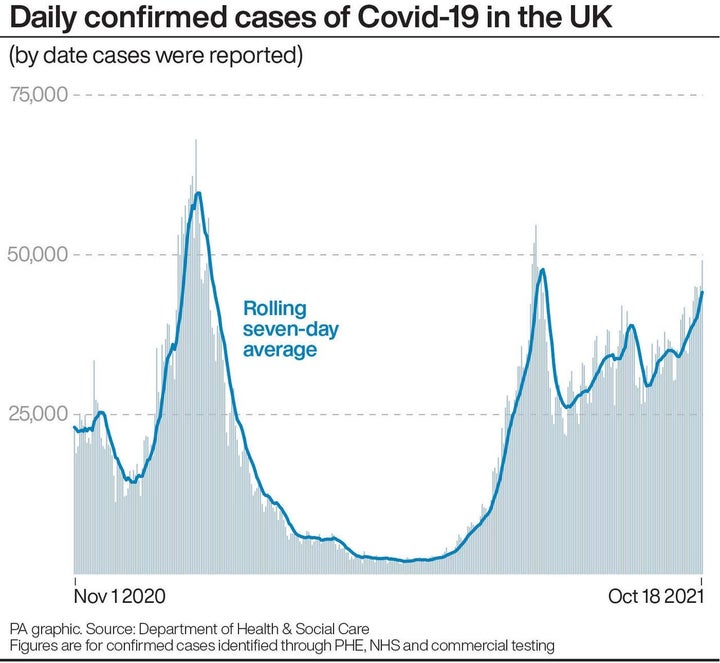
But the vaccine dose rate has dropped far below the 500,000 daily doses administered each day back in mid-March. Vaccinations have levelled off in every age group aside from 16 and 17 year olds.
Children were vaccinated relatively late in the UK compared to the those in many European nations. While healthy children are not necessarily at high risk from Covid, they can pass it to more vulnerable groups.
What’s the solution?
1. Booster jabs
Professor Neil Ferguson, a member of the government’s scientific advisory group for emergencies (Sage) has recommended that the government need to speed up boosters and vaccinations of teenagers.
At the moment, those aged 12 to 17 are only able to get one dose at a time – Ferguson wants these age groups to now receive two doses.
NHS England chief executive Amanda Pritchard said that the UK will now “make the most of half-term” by allowing those aged 12-15 to book their jabs online.
2. Wearing more masks
Health secretary Sajid Javid did warn that as part of the UK’s contingency planning, face coverings could become a legal requirement in England if the NHS buckled under another surge of cases.
However, many are calling for masks to be made mandatory sooner rather than later as cases continue to rise.
3. Better sick pay
According to Burn-Murdoch, the very make-up of the country’s economy plays a part in Covid levels too.
He tweeted: “UK has far worse sick pay than other Western European countries, making it much harder for people who do get sick to stay home and protect others.”
Back in October 2020, the UK was at the bottom of all OECD nations – Organisation of economic co-operation and development – when it came to the amount of mandatory sick pay it grants to workers.
Burn-Murdoch continued: “Older people are far more likely to be in poverty in the UK than elsewhere, which can increase their risk of both catching and dying from the disease.”
4. Updating the Covid symptoms
As the ‘super-cold’ takes hold this autumn, there are concerns many are dismissing real Covid symptoms because they think they have caught a more minor infection instead.
Epidemiologist Tim Spector of King’s College London – and the Zoe Covid Study – has been calling for the government to change its list of Covid symptoms on the official government website ever since the Delta variant became the UK’s most dominant strain.
While previous strains were recognisable for causing a shortness of breath, a dry cough and a fever, the Delta variant causes a sore throat, running nose and sneezing.
Spector claimed: “The UK still has more cases than most of Europe and I believe this is for two main reasons; the first is a lack of masks and social distancing and the second is because we’re ignorant of the symptoms.”
He added: “By not updating advice, we’re letting people into care homes, schools, workplaces and large gatherings displaying known signs of Covid.
“One in 95 people in the UK have Covid.”
