
Americans are more concerned about sepsis than ever before in the Internet age.
Some of that heightened awareness came recently, after Patty Duke's family went public about the fact that she died from the condition. The day the news broke, Google searches for the word “sepsis” spiked 827 percent. Recent spikes in search terms like “sepsis symptoms” and “what is sepsis” clearly indicate an interest in the condition and how people can protect themselves.
This dovetails with the ongoing efforts of medical professionals and policy makers to reduce cases of sepsis in hospitals. For instance, the Centers for Medicaid and Medicare Services issued new criteria for how to diagnose and treat sepsis last year in an effort to save lives and money, as severe sepsis is an extremely expensive condition to treat. The Centers for Disease Control and Prevention is also being more proactive about sepsis awareness messaging, especially after the highly publicized death of 12-year-old Rory Staunton in 2012. The boy had cut his arm playing sports, and the infection led to sepsis that went unnoticed at the hospital.
New public interest in the condition is a boon to the sepsis awareness movement and will certainly save lives. But the U.S. has no reliable way to track if awareness or prevention programs are actually making a significant dent in sepsis deaths. That’s because we don’t have an accurate way of tracking sepsis deaths, period, according to a new report from the CDC. Unlike cancer, diabetes or other diseases with national surveillance programs, health officials and researchers are currently unable to track national sepsis trends or tell whether or not new efforts to combat the syndrome are making a difference.
Because the U.S. has no way of accurately tracking sepsis deaths, there's no way to tell what needs to change in order to better fight against the condition. Establishing a national surveillance system could play a huge role in reducing sepsis cases, either by alerting doctors to clinical signs they may miss during diagnosis or counting sepsis deaths to track the progress of awareness campaigns.
“Unlike cancer, diabetes or other diseases with national surveillance programs, health officials and researchers can’t track national sepsis trends.”
What is sepsis?
Sepsis happens when your body has an overwhelming response to an infection. This overreaction can cause life-threatening organ dysfunction, and can kill in a matter of days or even hours. The sooner a health care provider can spot sepsis, the higher a patient’s chances for survival.
There is no diagnostic test for sepsis. Healthcare providers make what’s called a “clinical diagnosis” based on a constellation of symptoms that may include fever, elevated heart rate, abnormal white blood cell count and other factors. The problem is that sepsis symptoms like fever, difficulty breathing and pain are easily confused with other diseases or infections that could clear up on their own. Physicians and health authorities also disagree on when sepsis actually starts, making it even more difficult to diagnose and list as a cause of death on a certificate.
We don't know how much sepsis there really is
In the new report, the CDC analyzed sepsis deaths in the U.S. and found that yearly estimates vary wildly depending on how the data is collected. For instance, if the CDC uses administrative hospital codes to make an estimate, the mortality rate ranges from 168,000 to 381,000 deaths per year. But if they use death certificate data, the numbers range from 146,000 to 159,000 deaths per year. That means the hospital code estimate for sepsis-related deaths is 15 to 140 percent higher than the data drawn from death certificates, and there’s no way to tell if this data is an over- or underestimate of true sepsis deaths.
"This study highlights the need for a more reliable definition of sepsis, based on objective clinical data that can provide an accurate estimate of sepsis cases and deaths and whether there are changes in these estimates over time," the report's lead author, Dr. Lauren Epstein, told HuffPost.
We don't treat sepsis like a 'real' disease
Currently, the main ways to treat sepsis include antibiotics to address the infection the body is trying to fight, vasopressors to increase blood pressure, and other supportive care to help maintain blood sugar levels, modify the immune system, and keep the body hydrated and oxygenated.
A nationwide surveillance system could have the added bonus of elevating sepsis to a disease level that has its own targeted therapies, much like the way doctors and scientists approach cancer and heart disease, notes Dr. Paul Walker, president and CEO of the Canadian company Spectral Medical. Spectral is developing an experimental sepsis therapy, and the company plans to publish the results of their six-year U.S. clinical trial later in the year.
A national sepsis surveillance system could change everything
The best way to get an accurate count of sepsis deaths would be to create a national sepsis surveillance system that draws data directly from medical records, so that it isn’t up to individual healthcare providers to interpret patient records and come to a conclusion on their own, Epstein explained. Then researchers could use this data in an algorithm that predicts or diagnoses sepsis, and the outcomes could feed into national trend reports.
For a surveillance system to work, physicians, hospitals and healthcare authorities first have to agree on a definition of sepsis, its symptoms and when the syndrome starts. Is it the 2001 definition put forth by an international coalition of sepsis groups, which has been characterized by critics not sensitive enough? Is it their most recent 2016 definition, published in a February issue of the journal JAMA, which discards an emphasis on inflammation and focuses more on organ dysregulation? Is it something in between?
That's been the challenge for Dr. Stephen Claypool, the Minnesota-based medical director of the health division of the global IT and software firm Wolters Kluwer.
For the past four years, Claypool and his team have been experimenting with a surveillance system based on a computer algorithm that takes into account things like heart rate, body temperature, white blood cell count and other lab results in a patient’s electronic health records to spit out real-time sepsis diagnoses before doctors can even identify it.
The system is in place in two hospitals in Alabama and Florida, and sepsis mortality rates at both locations have gone down. But deploying the system on a national scale presents several hurdles, Claypool explained.
“A surveillance system is a great idea, but there are challenges,” he said. “Everybody agrees [sepsis] exists, but some people don’t want to call it sepsis until it gets really severe, and some want to call it sepsis earlier."
If an agreement was reached on when sepsis starts, the American healthcare system could then create an infrastructure for a sepsis surveillance system. But the groundwork could only be laid once the following two questions are taken care of, Claypool said: Do hospitals have the ability to let agreed-upon sepsis algorithms access electronic health records to compute underlying data? And will everyone agree to adopt the program, so that the nation’s hospitals can all be on the same page and begin counting cases of sepsis and sepsis-related death in the same way?
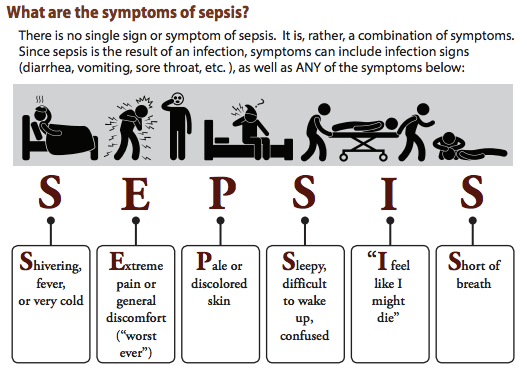
How to spot sepsis
Sepsis is difficult to spot, but the CDC uses a "SEPSIS" acronym to outline the basic symptoms of the condition for patients.
For now, the CDC has to keep aggregating big data on sepsis in piecemeal ways, which prevents health authorities and researchers from tackling the problem head on. And until a surveillance system is in place, it’s up to awareness campaigns among healthcare providers and the general public to not only prevent deaths by sepsis, but to spur more research in the field.
"More awareness of sepsis in the public could lead to earlier detection and more prompt treatment of sepsis,” said Epstein. "More public interest could also lead to more research into understanding the biological complexity of sepsis and identify biomarkers that can reliably identify sepsis and track clinical improvement."
CORRECTION: A previous version of this story referred to Wolters Kluwer as Minnesota-based. While the firm's medical director, Dr. Stephen Claypool, works in Minnesota, the company is headquartered in the Netherlands.