Mental Health Awareness week - a chance to share my story.
A chance to describe how at times I can be crippled by anxiety and a chance to highlight post-traumatic stress disorder (PTSD) as a hidden cost of neonatal intensive care.
Nothing can really prepare you for parenthood; but when your baby is born prematurely the time to plan and the excitement and anticipation of a new arrival is dramatically interrupted. Shocked and numb, you suddenly find yourself in the neonatal intensive care unit (NICU).
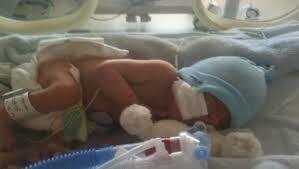
Neonatal intensive care - a scary sounding place and one you are unlikely to chance upon. As it happened I had worked in neonatal care as a children's occupational therapist and yet when my own son was born at 30 weeks I found myself lost in a medical world I did not recognise. For eight weeks I visited my baby every day, trying to become a mother in a unit where rows of incubators housed babies at the very edge of life. All around me monitors beeped and alarmed as they seamlessly chimed with the uncertainty of our journey.
Given the nature of NICU, the pain of leaving your fragile baby each day, the feelings of emptiness and grief, the uncertainty and ups and downs, the lines, wires, monitors and alarms, not to mention the security buzzers at the entrance of the unit or the constant rigorous hand washing, it came as no surprise to me that parents who have experienced premature birth are at greater risk of post natal depression, anxiety and PTSD.

I remember the moment I first felt panicked and sick with PTSD; I was returning to the neonatal unit for a routine 4 week follow up. Walking out of the car park and into the hospital I could hear and feel the sound of my heart pounding in my head. I could hear the beep, beep, beep of monitors and the sound of the ventilator as air filled my son's lungs. If I closed my eyes all I could see were wires and the mechanical rise and fall of my babies tiny chest. I felt sick to the bottom of my stomach and although I felt as if my body was completely shutting down, there was nothing I could do to stop it.
No one warns you about the flash backs, with PTSD often presenting itself once you are home. The support network of the hospital can disappear overnight and you are left to wonder how on earth you made it through. Family and friends with good intention assume that the difficult times are behind you and the idea that discharge would be the end of your neonatal journey suddenly seems farcical. I found the usual routes where I could have sought support closed to me, as well-meaning questions at health visiting clinics or baby groups only intensified negative feelings and bought back painful memories. The reality of becoming a mother in NICU is so far removed from the 'norm' that I quickly became isolated, unable to connect with the experiences of other families.
For a long time I believed I was alone in my thoughts of loss and grief and remained quiet about the flashbacks and crippling anxiety I was experiencing. I still remember the great feeling of relief when I first read another mothers account of life after neonatal care; suddenly I was no longer alone. In fact I was in quite good company, with more than 40% of NICU mums suffer from postnatal depression (compared to 5-10% of mothers who give birth to full term health babies), and more than half reporting symptoms of anxiety and PTSD. Yet, like many aspects of mental health, PTSD following neonatal intensive care is rarely spoken about. Through the openness and honestly of mothers, just like the account I first read, we can begin to normalise PTSD, raise awareness of the hidden cost of NICU and call from more support for mothers following premature birth.
This edited version was originally written for the Smallest Things blog, raising awareness of life after premature birth.