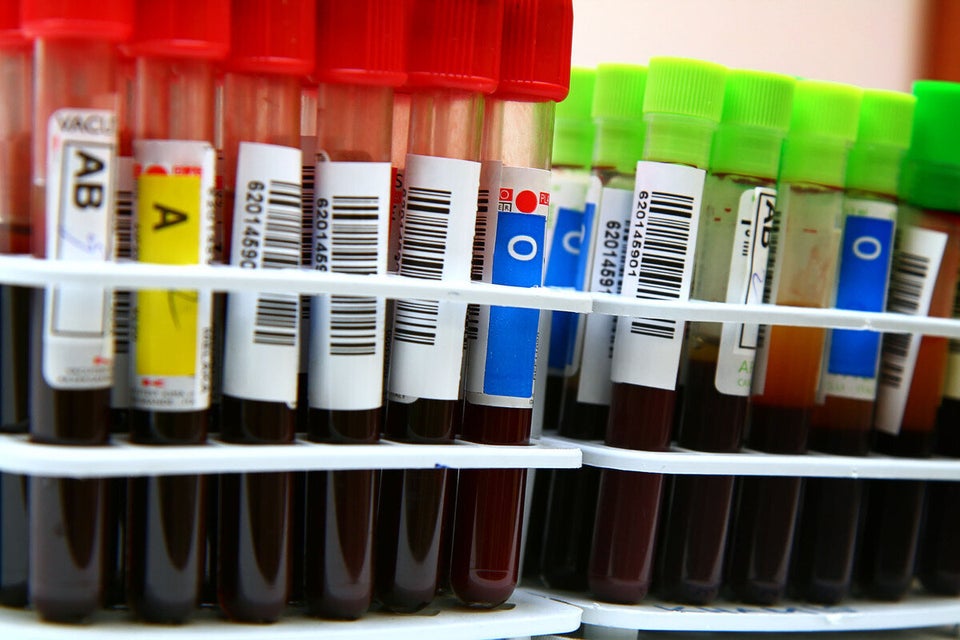
A small percentage of men have complained of a shortened penis after prostate cancer treatment, research reveals.
In a study conducted by researchers from Dana-Farber/Brigham and Women's Cancer Center in Boston, some men have lamented that the change in their penis has interfered with intimate relationships and caused them to regret their choice of treatment.
The study's findings, which are being published in the January issue of the journal Urology, are based on surveys completed by physicians of 948 men treated for prostate cancer and who had suffered a recurrence of the disease.
Complaints were more common in men treated with radical prostatectomy (surgical removal of the prostate) or male hormone-blocking drugs combined with radiation therapy, according to the study.
No men reported a perceived shortening of their penis following radiation therapy alone.
Things HuffPost UK Lifestyle learnt about prostate cancer in 2012
Twenty-five men complained of smaller penises after treatment – 3.73% for surgery, 2.67% for radiotherapy plus androgen deprivation therapy (ADT), and 0% for radiotherapy alone. Radiotherapy included both radiation administered by an external x-ray machine, and brachytherapy – the implantation of radioactive seeds directly into the prostate.
The scientific team, led by radiation oncologist Paul Nguyen, MD, and medical student Arti Parekh, said it is the first study to link men's perceptions of a reduction in penis size to lowered life satisfaction, problems in emotional relationships, and misgivings about the specific form of prostate cancer treatment they chose.
Nguyen said that the potential side effect of a smaller penis is well-known among physicians and surgeons.
"But it's almost never discussed with patients, so it can be very upsetting to some men when it occurs," he added. "Patients can deal with almost any side effect if they have some inkling ahead of time that they may happen."
The report's authors said physicians should discuss the possibility with their patients so that they can make more-informed treatment choices.
There were no direct measurements of penis size either before or after treatment, said the researchers. Nor did the patients' physicians specifically ask about this side effect; the issue was brought up by patients in conversations with their doctors. For this and other reasons, the authors of the new study suggest that the problem is likely more common than reported in the survey.
"Prostate cancer is one of the few cancers where patients have a choice of therapies, and because of the range of possible side effects, it can be a tough choice," said Nguyen. "This study says that when penile shortening does occur, it really does affect patients and their quality of life. It's something we should be discussing up front so that it will help reduce treatment regrets."
The likelihood and magnitude of penis shortening as a consequence of treatment have not been well studied, said the researchers.
However, Jim Hu, MD, a surgeon at the University of California, Los Angeles Medical Center and a co-author of the study, said: "Previous studies have concluded that there is shortened penis length following prostatectomy. This is most common with non-nerve sparing surgery, as this may result in fibrosis and atrophy of erectile tissue due to damage to nerve and vascular structures." The present study did not find much difference on that score.
The study's subjects were men enrolled in a registry called COMPARE that collects data on patients whose prostate cancer shows signs of recurring after initial treatment. Of the 948 men in the study, 22% were younger than 60 and the majority were in their 60s, 70s and 80s. Just over half – 54% – had undergone surgery to remove their cancerous prostate, while 24% received radiation therapy combined with hormone-blocking treatment, and 22% had radiation therapy alone.
In an editorial comment accompanying the report, Luc Cormier, MD, PhD, of Dijon University Hospital in France said the study "is really of interest because of the number of patients and that it included other treatment methods in addition to radical prostatectomy."
The surveys of the men did not report on their sexual functioning. Cormier observed that "sexual activity needs to be thoroughly measured owing to the obvious relationship with the patients' perception of penile length."