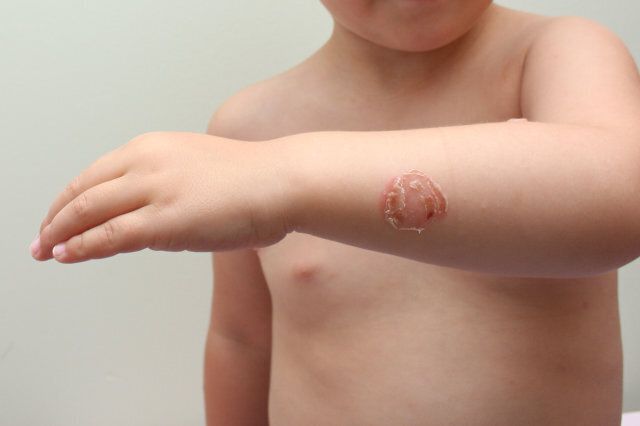
Has your child suddenly developed red, itchy blisters around their nose and mouth? Then they might have picked up impetigo.
What is it?
Impetigo is a highly contagious bacterial infection, which is fairly common in children. Adults can catch impetigo as well, but as children have less developed immune systems, and because they tend to be in close physical contact with one another in nurseries and schools, they are more prone.
Impetigo enters the body through broken skin – for example, via a cut or graze, or a patch of nasty eczema. Children carry the bug around with them for between four and 10 days before showing any symptoms of impetigo – and this is why it's so hard to avoid if there is a spate. There are two types of the infection: bullous impetigo and non-bullous impetigo.
Bullous impetigo results in large, fluid-filled blisters, usually on the body, which will take several days to burst and scab over.
Non-bullous impetigo results in small, red, itchy blisters which usually occur around the nose and mouth. They burst quickly, and evolve into brownish coloured scabs. Non-bullous impetigo can spread to other parts of the body.
Left untreated, impetigo would clear up by itself within a few weeks, but because it's so contagious (not to mention uncomfortable for your little one), treatment is recommended.
What can I do?
If you notice red bumps or blisters around your child's nose and/or mouth, go to your GP. The doctor should be able to diagnose impetigo on sight, and will probably prescribe you with an antibiotic cream to fight off the infection.
Follow the instructions that come with the cream. Within 48 hours of beginning treatment, the impetigo should no longer be infectious, but finish the course your child was prescribed.
Meanwhile, you need to do what you can to avoid spreading impetigo around the household and neighbourhood, as well as around your child's body.
Scratching the blisters can not only make them worse, but it can also lead to patches of impetigo cropping up elsewhere, so keep your child's nails trimmed right down, and clean.
Young babies might benefit from wearing mitts, particularly at night time (older children might not tolerate mitts, but you could try!). If your child has any cuts or grazes, clean them, and cover them with a bandage or plaster. You could also tape a loose gauze over the blisters on your child's face.
Keep the impetigo scabs clean – gently wash them once or twice a day with mild baby soap and water. Pat them dry with some paper towel – and then chuck the paper straight in the bin.
Don't let anyone share a towel, flannel or pillow with your child. Also, wash their bedding and clean their toys.
Do keep your child away from playgroups, nursery or school until the infection is no longer contagious. Once 48 hours of treatment has passed, they can return as long as they do not have any pus-filled blisters. If the pus is still present, then so is the infection.
If, after a week of treatment, the impetigo is still there, go back to your GP, who might need to investigate further. The doctor might offer your child oral antibiotics at that point – if so, it is absolutely essential that your child finishes the prescribed course, even if they seem to be better.
Occasionally, impetigo can lead to other infections and illnesses – so if your child develops a fever, or any other symptoms after being treated for impetigo, go straight back to your GP.
Although it can be extremely hard to avoid impetigo, because of its sneaky incubation period, you might reduce the risk of your child contracting it again if you ensure cuts and grazes are wrapped up or have a plaster applied.
What else could it be?
If your child has a red bumpy rash on their face, but it's also elsewhere on their body, such as between their fingers or on the hands and wrists, then they might have scabies.
More on Parentdish