A mum is urging women to learn the symptoms of Bacterial Vaginosis (BV) after the condition caused her to go into premature labour.
Amanda Butler, 42, from Milton Keynes, went into labour when she was just 25 weeks pregnant.
Her son Callum was born weighing 1lb 9oz and had to undergo a heart operation, a lumbar puncture, laser eye surgery and 10 blood transfusions.
"Callum’s experience was awful, and it was incredibly difficult for my husband and I to have to watch him suffer," says Butler.
"As a new mum, it was heartbreaking not to be able to cuddle my son for weeks after he was born."
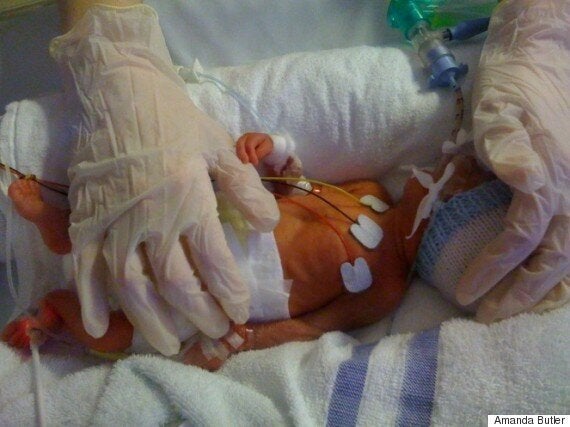
Callum Butler
Doctors later informed Butler her labour had been brought on prematurely because she had BV.
"I was angry because it was the first I had heard of it," Butler said. "I feel like it could have been totally avoided had I been given the right information.
“Today, Callum is a happy, healthy little boy, but I am definitely one of the lucky ones.
"I don’t want anyone else to have to go through what Callum endured, so I would urge anyone in the early stages of pregnancy who thinks they may have the symptoms of BV to speak to their midwives as soon as possible."

Amanda Butler and Callum
BV is a common condition in which the natural balance of bacteria inside the vagina becomes disrupted.
One in three women will get BV at some point in their lifetime according to the sexual health charity FPA.
For the majority of women it won't pose any threat to their health and around half of the women who develop it won't experience any symptoms.
"If you do get symptoms you might notice a change in your usual vaginal discharge," explains Paul Casey, FPA’s Training Manager.
"This may increase, become thin and watery, change to a white/grey colour and develop a strong, unpleasant, fishy smell, especially after sexual intercourse.
"Bacterial vaginosis is not usually associated with soreness, itching or irritation."
Butler had experienced symptoms during her pregnancy.
“I noticed a discharge around about a week before I eventually went into labour, but I didn’t pay it any attention because pregnancy itself can cause that to happen, and it certainly didn’t concern my midwife," she said.
It is not known what causes the condition, but being sexually active, using scented soaps or bubble baths, having an intrauterine device fitted or using a vaginal deodorant can increase your risk.
If you are experiencing symptoms and you are pregnant, you should contact your GP or GUM clinic as a precaution - although it is important to bear in mind discharge can be a normal part of pregnancy and BV causes no problems in the great majority of pregnancies.
"The infection has been found in some women who have had a miscarriage, a premature birth or a low birth weight baby," Casey tells HuffPost UK Lifestyle.
"Bacterial vaginosis can safely be treated when you are pregnant and when you are breastfeeding – this won’t harm the baby, but do tell the doctor or nurse if you are pregnant. This will influence the type of treatment that you are given."
Your GP will ask you about your symptoms and may examine your vagina.
In some cases, a small sample of the vaginal discharge will be taken using a plastic loop or swab. It only takes a few seconds and is not usually painful.
If you are diagnosed with BV, Casey says there's no need to be alarmed as the treatment is "simple".
"Treatment involves taking antibiotic tablets, either as a single dose or for up to a week, or a cream or gel for use in the vagina for around one week," he explains.
"These treatments are very effective though it is quite common for bacterial vaginosis to return, and some women get repeated episodes.
"In these cases, women may be given a course of antibiotic gel to use over a number of months and others may be given antibiotic tablets to use at the start and end of their period.
"Some women may also find it helpful to use a lactic acid gel, which can help to restore the pH balance in the vagina."
Amanda is sharing her story as part of a National BV Day campaign from Balance Activ, which aims to raise awareness of the condition.