"I became terrified of everything, afraid to eat, and convinced the baby would die…”
Dr. Rebecca Lawrence is a psychiatrist who found herself also being a patient. She was admitted for depressive disorder during the early stages of her career.
"I had hoped to train as a psychiatrist myself, and I thought that possibility was now extinguished, that anyone who had been a psychiatric inpatient would never be accepted as a colleague," she explains in an article published by the BMJ.
One in four people in the UK will experience some kind of mental health problem over a year.
It is "the single greatest illness that affects mankind," Professor Stephen Lawrie, Head of Psychiatry at Edinburgh told The Huffington Post UK.

Peak- time commuters crammed into a train, with heads lodged into their neighbours’ armpits can explain some of this biology.
The brain, simplistically put, is similar to an overtly complicated railway system made up of long trains (or neurons) carrying messages.
Unlike the vehicles that roll into King's Cross however, our neurons don’t really move. They simply act as a conduit for signals to jump along.
Between the trains are gaps or junctions called synapses across which the neurons relay their message.
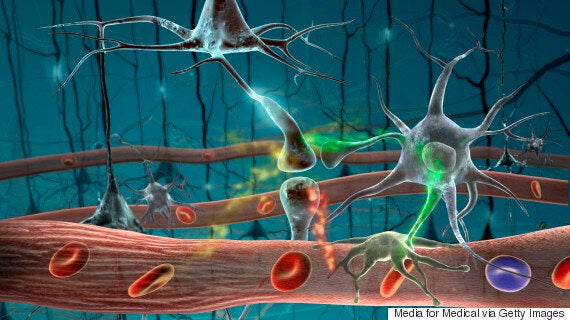
Neurons signalling each other
To ensure the point gets across from neuron to neuron, or train to train, the brain uses chemicals called neurotransmitters.
Similar to most organised networks –biological or otherwise –our neural system is susceptible to failure.
"Due to inclement weather, please ensure you take care while travelling."
Those monotone pre-recorded announcements echoing across a platform are applicable to our brains too.
However, instead of the weather, external factors playing on our neural system are far more unpredictable - they are either genetic or environmental.
Genes have an important role to play in the outworking of mental health illnesses.
"There were, perhaps, a number of warning signs of what was to come—a long period of blackness after a relationship ended, and one of poorly controlled mood before final exams—but hardly different from many others," Dr. Rebecca Lawrence writes.
"I was unaware at that time of family history."
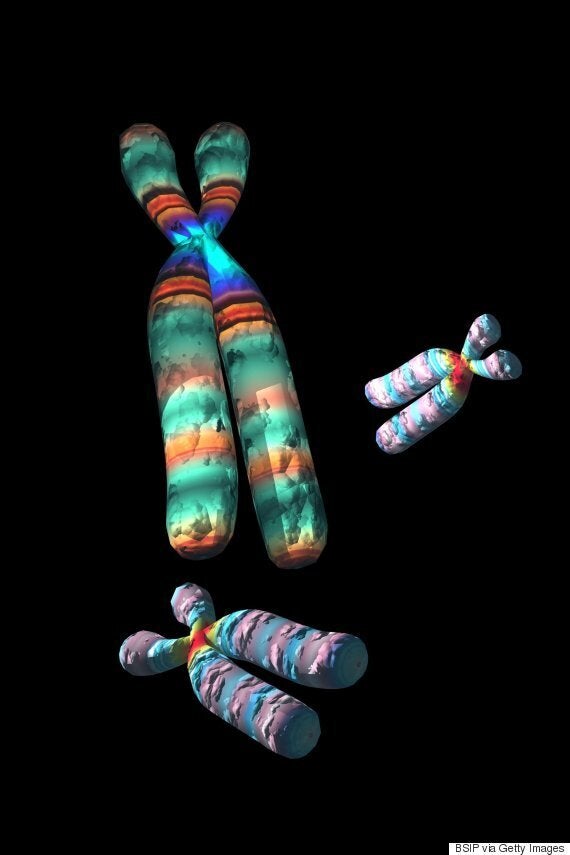
Genes packaged in chromosomes
"67-year-old John Raubenheimer is a poet. He was diagnosed with schizophrenia approximately 30 years ago.
"At the time I wasn't really able to process it. I just laughed it off. I didn’t really see myself as mentally ill. It took a long to come to terms with it."
According to Professor Stephen Lawrie there are 108 genetic regions on our chromosomes, where our DNA is packaged, associated with schizophrenia.
Again, it comes back to neuron to neuron communication. Certain genes can disrupt the communication taking place across the junctions of our brain.
Typically, neurotransmitters need to bind with their matching receptors found in the junctions between neurons. In the case of schizophrenia, Professor Stephen Lawrie explains, there is too much dopamine (a type of neurotransmitter) being produced.
Medication aims to reverse this by stopping dopamine from being registered by the receiving neuron once it crosses the junction.
"Medicine has helped me a lot at the moment. It is just ticking over." John explains in a gentle South African accent.
"Going back in time, schizophrenia meant I was living in a world of my own. It was more to do with having a whole world structure itself around this dream. The dream allowed me to be significant. It was an answer to my helplessness.
"Finding significance and real interaction with people was the answer. I am on a small amount of medication. I take a small dose of antipsychotic medicine and I don't see a psychiatrist or anything."
The last time John saw a psychiatrist was in 2000, the year after his wife died. That was the year he had a breakdown.
Schizophrenia affects approximately 200,000 people in England and Wales and is heavily linked to genetics.
Mortality among people with schizophrenia is approximately fifty per cent above that of the general population, partly as a result of an increased incidence of suicide.
Environmental factors including stress induced from bereavement, increases the risk of psychosis, Professor Stephen Lawrie explains.
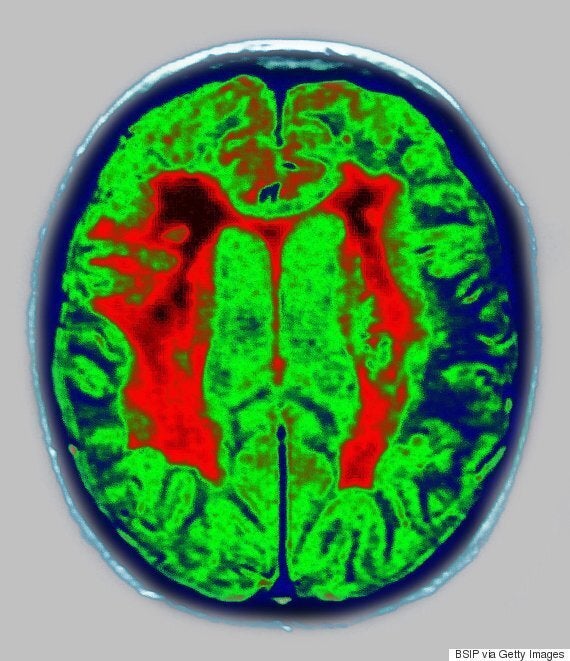
CT scan of the brain
"I don’t really know how I felt—bleak and exhausted, but also sad and angry, especially when I saw other doctors apparently confident and successful," Dr. Rebecca Lawrence writes.
"I had a series of admissions, both before and after my baby was born. What was my diagnosis? How to classify the feelings of fear, terrible fatigue, anxiety, and blackness?
"Depression was what I was told, but I formed an unshakeable conviction that everyone thought I had a personality disorder."
In July, Nature published a study identifying two risk genes associated with depression.
However, experts still say more information is needed.
Joe Herbert, a professor of neuroscience at the University of Cambridge told The Huffington Post UK:
"We don't really know what causes depression at a neural level (in the brain). We do know that depression may follow adversity (for example, loss) particularly if it comes on the back of chronic difficulties.
"But what happens in the brain, and why some people are more resistant than others is unknown."
While we wait to find out, scientists believe the current treatment options are working to reverse the faults in our complex neural network.
Antidepressants
"Looking back, I still think my personality was sorely tested by my experiences. I did improve with electroconvulsive therapy and medication, but hated taking them," Dr. Rebecca Lawrence explains.
In terms of medication, some experts believe it works on junction to neuron communication, with the neurotransmitters being the centre of attention.
"Antidepressants work in a bottom up way, inhibiting the re-uptake the neurotransmitters," Professor Stephen Lawrie says. "The best evidence is that serotonin levels in the brain are low in people with depression, and antidepressants increase levels."
There is also a theory suggesting that medication works by building new neurons – or new trains, a process known as neurogenesis.
Harvard Medical School published a report explaining that neurogenesis is a possible explanation for why there is delayed response to antidepressants.
"…people typically don’t begin to feel better for several weeks or longer…"
Citing studies that prove this, the report continues: "The answer may be that mood only improves as nerves grow and form new connections, a process that takes weeks."
However, Professor Stephen Lawrie is quick to point the flaw in painting such as black and white picture.
"This is highly regarded as over simplistic stories, which are part truth but by no means the whole truth."
Dr. Rebecca Lawrence also doesn't believe there is one solution. She told us: "There simply isn't one best option, with far too many variables."

"When I read a textbook description of psychotic depression, my diagnosis, I can’t marry it with how I feel,"she writes.
"I do feel low, but also agitated and frightened, and simply very ill. I still fear that others think I have a personality disorder."
"Stigma is still very much associated with psychiatric disorders and that is very unfortunate," Professor Stephen Lawrie says.
"Some people say its all in the mind. None of those things are true. It just reflects people’s fear of mental illness. The tragedy is that even in our 21st century Britannia only 25 percent with a diagnosable mental health get treated."
When you look at the burden psychiatric conditions places on life, this statistic becomes concerning.
Disability-Adjusted Life Year (DALY) is a metric the World Health Organisation (WHO) uses to quantify “the Burden of Disease from mortality and morbidity.”
According to WHO, neuropsychiatric disorders are the third leading cause of disability-adjusted life years (DALYs) in Europe
Despite this, Professor Stephen Lawrie believes mental health does not get the monetary attention it deserves.
NHS bosses are supposed to spend 13 percent of their budget on mental health which corresponds to WHO goals. However, most Trusts only spend 10 percent or 11 percent.
Professor Stephen Lawrie is optimistic about the future. "Understanding is improving. Treatments are improving. People are becoming more accepting.
"I remain optimistic that things are getting better slowly but surely."
For those with a diagnosis, the outlook is less clear cut.
Dr. Rebecca Lawrence expands: "My current plan is to be more open and to tell people, but that’s not easy either. Often they’re very embarrassed, and I don’t want my patient status to become the most important thing that people know about me."
For John, a volunteer with the mental health charity SANE, poetry is the way forward. He has just had a poem accepted for publication in The Great British Write Off .
"Shall I read you a poem, he asks enthusiastically?" "Sure," I replied.
"This is a line from ‘The Beauty Of Comedy And Madness,"
"…as sanity slowly claimed me. I trailed it behind me like a lost balloon…"