Warning: This article contains content and images on the subjects of mental health and self-harm that some people may find triggering.
For many people caught in the pain and turmoil of a mental health crisis, difficulties accessing NHS treatment were already acute before a global pandemic stuck.
But a HuffPost UK investigation has found long waiting times for mental health care have been exacerbated by the strain coronavirus has placed on the NHS.
It was already common for patients to be asked to wait between six weeks and a year for basic mental health treatment prior to the pandemic.
They are now given a minimum waiting time of 10 months to start therapy and are being forced to cope with even less access to their local services as staff, funding and resources are burdened by the stress of the pandemic.
Jacob, 22, an anthropology student at Birkbeck University, who has asked for his last name not to be published, is currently on an 11-month waiting list for psychological therapy through the NHS, a service he says he needs now.
“I’m very uncomfortable – I feel scared,” he said. “I am experiencing real fear right now and I think to be told 11 months is ridiculous.”

He is considering paying for private mental health care if he cannot get help soon.
Jacob left his flat in London when lockdown was announced in March and moved in with his grandmother in Wiltshire.
Once there, he spent the first week calling his London GP to get his prescription transferred. He was unsuccessful. They were too busy to respond and told him to find a GP where he was even if it was temporary.
Upon registering with his grandmother’s GP he also requested mental health therapy, but he was told not to expect an appointment until May 2021.
Jacob was diagnosed with bipolar 2 disorder four years ago, a condition that involves depressive and hypomanic episodes. After his initial diagnosis he was left waiting for therapy for five months and then had a breakdown, warranting him being sectioned for 28 days.
“I was in a really dark place and, if I’m going to be honest, I was happy to be in there,” he said. “I was nervous to leave because I felt so safe and looked after.”
Once discharged, Jacob lived with full autonomy. He had a job, lived on his own and started university.
But he has had small episodes of anxiety and depression since the start of the pandemic that he believes require a psychologist’s attention.
“If I were living on my own right now, I don’t want to think about it,” he said. “That would be horrendous. I’m very grateful to have my grandmother. It’s a huge blessing I cannot explain.”
Once Jacob moves back to London as the pandemic eases, he will have to re-register with another GP and jump back to the end of the queue to access cognitive behavioural therapy, a talking therapy to help manage his condition, adding an additional minimum of six months to his current wait time.
He may end up waiting between one and two years for therapy by the time he finally receives it.
“I have friends who have been waiting 18 months plus for DBT therapy and they are just not getting any better”
- Emma-Marie Whittenham
Jacob told HuffPost UK he feels he only has two choices: pay for private mental health care out of his own pocket or keep waiting until his condition spirals enough that he requires emergency help again.
Another student, Hannah Hawkins, 21, who is studying sport science and physiology at the University of Leeds, is also being forced to wait as her condition worsens during lockdown.
Prior to the pandemic, Hawkins had overdosed three times and was sent to hospital multiple times. Her condition is still left undiagnosed and untreated.
Her most recent overdose was in March last year, during the second half of her first year at university.
After being released from the hospital she was told to get on with her life like normal, but due to her continued mental health problems she missed most of her first year of classes and was forced to drop out of university.

Without professional help, the way she was left to cope with the suicidal and self-harm tendencies she was experiencing was through the distraction found in routine.
Now, because of the pandemic, Hawkins is no longer working and her eating and sleeping habits have become chaotic.
She told HuffPost UK she knows she needs help and is trying to finish the registration with her GP in Kent but the anxiety she feels about not being taken seriously is making it very difficult to move forward.
“Taking the next step is like just getting closer and closer to getting invalidated again and reliving things that have already happened in the hospital when the mental health team didn’t listen to me, and they just came to a really horrible conclusion that I wasn’t really struggling with anything,” she said.
“I feel like I’m one of the lucky ones. But it had occurred to me that it’s probably because I was so ill”
- Sarah Graham
Although Hawkins has not been able to get a diagnosis or any long term treatment, others who have managed to break into the system have experienced increased support and help during the lockdown.
Sarah Graham, 42, a painter in Hitchin in Hertfordshire, is feeling stable and on the brink of a full recovery with the support of her mental health team during the pandemic.
“I feel like I’m one of the lucky ones. But it had occurred to me that it’s probably because I was so ill,” she said.
Graham was sectioned by the NHS three years ago following a manic episode involving the police picking her up from a hotel room where she was having delusions of meeting the Queen and rescuing the country from a terrorist attack.
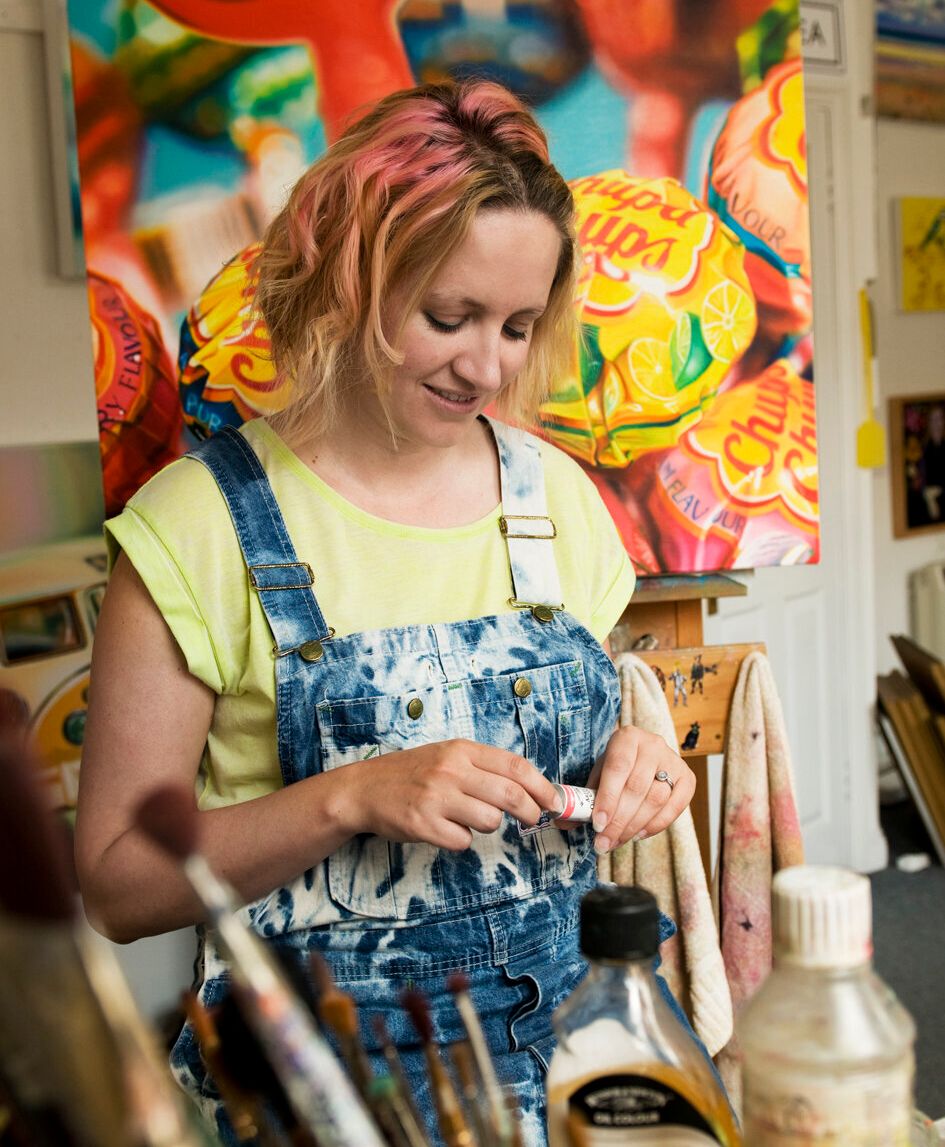
She was placed with a crisis team and eventually graduated to a care team. Post-lockdown, she still regularly meets her psychiatrist and care coordinator but now the appointments are all carried out over the phone.
Graham told HuffPost UK the two most difficult aspects of the pandemic are not having those important face-to-face meetings with her psychiatrist, and the possibility of losing her care coordinator due to NHS cuts.
She was recently informed the care coordinator, who is a psychiatric nurse, might be replaced by a nurse who is neither trained in mental health care nor her medical history.
“I would be gutted if I lost my care coordinator through this,” said Graham. “Even though I’m doing well, she needs to know the whole picture, the good times and bad times. So I just have my fingers crossed that I can maintain that with her. It’s important to me that I do have that support and, if I do have a dip, then I can ring her straight away.”
She says she is aware of the risks for those who have not been so lucky in accessing care.
“I know that I am one of the lucky ones with my bipolar,” she said. “I know that it is so destructive and can shatter people’s lives and they can lose their confidence and be battling very constantly. I am so lucky that I have periods of wellness where I can lead a very normal life. Even through lockdown and even through this pandemic.”
Because getting into the system is sometimes so difficult, some patients have chosen to pay for private care because it ensures treatment and wait times are minimal, if any at all.
Emma-Marie Wittenham, 28, who works in digital advertising in central London, opted for private mental health care last year after being told it would take at least six months to see a specialist, despite being given a diagnosis and told she needed treatment.
And now, during the pandemic, she has been able to utilise and access anything she has needed without additional wait times or resource restrictions.
“I know so many people that don’t have private healthcare and the pandemic hasn’t helped,” she said. “It’s isolated so many people. I’ve got friends that are just tearing their hair out pretty much not dealing with it. It’s also people who haven’t suffered with mental health before and the pandemic just exaggerates it, even more so than it would have been.”

Wittenham stopped seeking psychological help through the NHS after having a mental breakdown in January 2018 when she was prescribed a specific therapy by her crisis team but was not given a means to access it.
“For me it definitely escalated my internal turmoil probably tenfold because I was just like: ‘No one’s going to help me – I’m just a waste of space,’” she told HuffPost UK.
In June 2019, she finally sought private mental health care after finding out her work would cover the costs. Within 24 hours, she found a therapist nearby and had an appointment and consultation booked.
She has since been diagnosed with bipolar 2 and borderline personality disorder (BPD) and has been able to receive dialectical behaviour therapy (DBT), which has been found to be particularly effective for patients with BPD, every week since.
If Whittenham’s employer had not offered to cover private healthcare costs she would not have been able to afford the therapy, which would have cost her at least £440 a month.
“I have friends who have been waiting 18 months plus for DBT therapy and they are just not getting any better,” she said.
“In fact, because they are worrying so much about getting this therapy they are admitting themselves into the hospital more because life is just building up and they are getting so desperate and they need help.
“You feel like you are just a number waiting on a queue and if you are not on death’s door, they don’t really want to push you further.”
Whittenham says she has received great care from the NHS for physical health problems. It is only in mental health care that she feels she was abandoned.
Dr Andrew Molodynsky, lead mental health consultant at the British Medical Association, told HuffPost UK: “The thought of everyday people paying for private healthcare because of necessity is just deeply saddening.
“My advice would be if people can afford it and their welfare is massively affected by mental health problems then, sadly, it’s probably the right thing to do.”
Experts agree that the chronically underfunded mental health care system in the UK, which was already struggling, is now buckling under the added pressure of the pandemic.
Lucy Schonegevel, head of health influencing at the charity Rethink Mental Illness, said: “Given the overall disruption that many people living with mental illness will have experienced in recent months, it’s vital that mental health is prioritised in response to this crisis so that people can access the support they need, when they need it most.”
According to a recent survey by Rethink Mental Illness, 42% of people said their mental health was worse because they were getting less support from mental health services in the early months of the pandemic. Some 8% of respondents said they hadn’t been able to receive medication.
An NHS England spokesperson said: “Although this survey offers only a snapshot of people’s experiences, the NHS across the country has moved fast to support people who need help with their mental health during Covid including video consultations, online support and the setting up of a new 24/7 mental health crisis hotline.
“Our plans to invest an additional £2.3bn every year by 2023/24 stands firm and we urge everyone who feels they are struggling to cope in these unusual times to seek early advice whether through friends and family [or] self-help websites such as Every Mind Matters, and if your symptoms worsen the NHS is here for you.”
Useful websites and helplines:
- Mind, open Monday to Friday, 9am-6pm on 0300 123 3393
- Samaritans offers a listening service which is open 24 hours a day, on 116 123 (UK and ROI - this number is FREE to call and will not appear on your phone bill.)
- The Mix is a free support service for people under 25. Call 0808 808 4994 or email: help@themix.org.uk
- Rethink Mental Illness offers practical help through its advice line which can be reached on 0300 5000 927 (open Monday to Friday 10am-4pm). More info can be found on www.rethink.org
