Since COVID-19 turned our lives upside down six months ago, scientists have been scrambling to learn as much as they can about this deadly disease.
There is still a lot of research to be done. But back in April, a team at Duke University set out to answer a question that was on everyone’s minds (and still is): How effective are face masks at reducing the transmission of respiratory droplets that carry the coronavirus?
The researchers, who released their results in early August, found that a fitted N-95 mask (without a valve) and a three-layer surgical mask are the most effective at preventing the spread of aerosol droplets that might carry COVID-19.
This study is one of the first to focus on the effect of a mask at stopping its wearer from spreading potential coronavirus aerosols (rather than protecting the wearer from those nearby).
“All the testing in the past had to do with protecting the individual wearing the masks, not considering protecting other people,” Eric Westman, one of the study’s authors, told HuffPost. “So, for example, the N-95 mask with a valve is the best [at protecting you], but the valve allows you to exhale unfiltered air, so it’s not the best mask when looking at whether it protects other people from you if you’re sick.”
The team avoided assigning a definitive ranking to the masks in the study — which has significant limitations and faced criticism when the results were published — but agreed that a fitted N-95 mask (one without a valve) is one of the most effective face coverings currently available.
Because research on the efficacy of certain types of masks is still scarce, these results are useful in that they provide us with more information on the importance of wearing masks.
How was the study conducted?
To analyze 14 different masks — which Westman said were chosen because they were “conveniently available” — the researchers came up with a relatively simple method that involved a black box, a lens, a laser and a cell phone camera.
“The idea of testing real people with a laser is novel,” Westman said. “Before this pandemic nobody really considered doing that.”
The team cut a hole in the front of the box and two thin slits across its left and right sides. A laser beam shined a light across the slits while a cell phone camera was positioned on the back of the box. Study participants were then asked to speak through the hole while the cell phone recorded the way the light moved in different directions by the speaker’s respiratory droplets. A computer algorithm did the rest.
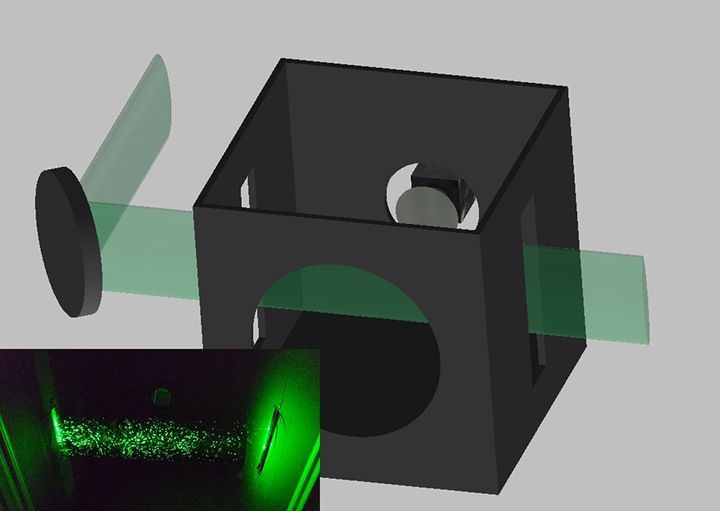
Participants first spoke through the hole without a mask on, and then again while wearing the masks.
Each of the 14 masks was tested 10 different times.
Are there masks we should avoid?
The gaiter — a type of face covering often used by outdoor exercisers — that the study tested was the least effective of the 14 masks. In certain circumstances and depending on the fabric it’s made of, a gaiter might be more dangerous than helpful.
“The more porous the fabric, the more you can see through it or blow through it, the less it works,” Westman said.

And you might want to think twice about covering your face with a bandana, bandit-style: They didn’t perform particularly well within the constraints of this study.
Though the study is far from perfect, Jack O’Horo, an infectious disease specialist at the Mayo Clinic, noted that the research has gotten experts closer to understanding that a mask’s material — rather than the type of mask — should be examined to determine its efficacy.
“We may ultimately find out what materials should be acceptable and not acceptable,” he said. “I have been giving the advice that if you can hold up the material through the light and see the points of light throughout it, then it’s probably not going to work as a mask.”
Which masks are best?
The fitted N95 masks without valves performed best, but the three-layer surgical mask (#1 in the image above), a cotton/polypropylene mask (#5) and a two-layer polypropylene apron version (#4) also all registered relatively low droplet counts.
See a thorough performance chart here:
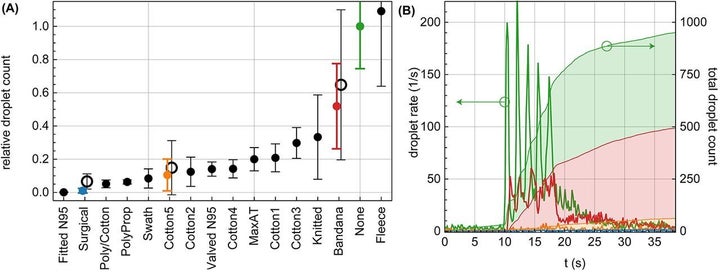
Medical-grade N95 masks are “critical supplies that should be reserved for healthcare workers and other first responders,” Jasmine Reed, the public affairs specialist at the Centers for Disease Control and Prevention, told HuffPost.
But the shortage of N95s that mask wearers were warned about at the beginning of the pandemic is not as big of a problem now. The supply chain is getting better, O’Horo said. However, he added that he believes that the general public won’t necessarily benefit from this particular mask style.
“When N95s are used in health care settings, we do a thorough fit testing to make sure the fit of the mask is tight enough to work as a respirator,” he said. “If it’s not the appropriate fit, it’s not better than a surgical mask.”
What are the study’s limitations?
After releasing the study, researchers at Duke faced a lot of backlash from scientists, journalists and the general public. Criticisms ranged from complaints about the study’s limited sample size to the lack of an epidemiologist on the research team. Another drawback: The test subjects didn’t necessarily mimic real-world behavior. Although the recorder measured the extent of the aerosol spread when normally speaking, people tend to talk louder (and more softly), sneeze and cough throughout a regular day — behaviors that might totally shift the results of the research. (Yes, speaking loudly does, indeed, increase the amount of aerosols you release through your mouth.)
Study co-author Martin Fischer, a chemist at Duke, held a press conference about a week after its publication, saying that the study, entitled “Low-cost measurement of facemask efficacy for filtering expelled droplets during speech,” was meant to demonstrate a particular way to test mask effectiveness, not test all possible types of masks.
“We did have one person already — a volunteer who makes their own masks — asking, ‘How can we test our masks?’” Westman told HuffPost. The study at least “raised awareness that not all masks are the same.
He went on to acknowledge that the team “raised more questions than we have answered but I’d like to see a study done with a systematic look, different fabrics, different styles.”
Although he agreed with most of the criticisms, O’Horo said the study produced some useful guidance: “The idea that a face covering is a face covering is a mask [is not correct]. We can give better advice as to what actually counts as a mask.”
According to O’Horo, a cloth mask with two layers is the preferable face covering for the average non-medical professional to wear every day.
“Masks that aren’t perfect still are helpful,” Westman said. Which is to say: Stay safe, wear a mask and think about the people around you.
Experts are still learning about COVID-19. The information in this story is what was known or available as of publication, but guidance can change as scientists discover more about the virus. Please check the Centers for Disease Control and Prevention for the most updated recommendations.