Have you noticed that some goals lose their charm with age? (Get a perm. Marry a New Romantic.) Others become increasingly urgent - even when they are decades overdue.
Global surgery is the second type. It's a life-and-death 'to do' more than 35 years in the waiting, but a recent sign suggests this could finally be about to change.
"The vast majority of the world's population has no access whatsoever to skilled surgical care and little is being done to find a solution," said the Director-General of the World Health Organization (WHO).
That's not the recent sign - that's from a speech Dr Halfdan Mahler gave back in 1980. But even then, the scope of the crisis was clear.
Global surgery was never about cosmetic or elective procedures. While the average American sat on track to undergo seven operations over the course of a lifetime, women in low-resource countries were dying for want of an emergency Caesarean section; agonising and grieving, often poisoned by sepsis.
"The era of only the best for the few and nothing for the many," declared Mahler, "is drawing to a close..."

To some extent. Many initiatives in the following decades aimed to redress imbalance and universalise certain essentials. The spread of HIV captured public attention and massive funding; a Who's Who of organisations threw their weight against polio.
But a global effort to ensure safe and essential operations in low-resource settings never really made it past a devoted but inherently short-term network of service-delivery organizations and a passionate but small group of acronyms. They've changed thousands of individual lives and produced compelling reports, but struggled to inspire mass action from the surgical community.
Even as WHO made global priorities of maternal care, road traffic accidents, emergency response - conditions that inherently require surgical intervention - surgery was kept apart.
As a result, local efforts to improve surgical provision like new medical schools and education councils don't get the support they need. They remain impressive outliers rather than scalable templates, and surgery keeps its infamous title: the "neglected stepchild of global public health."
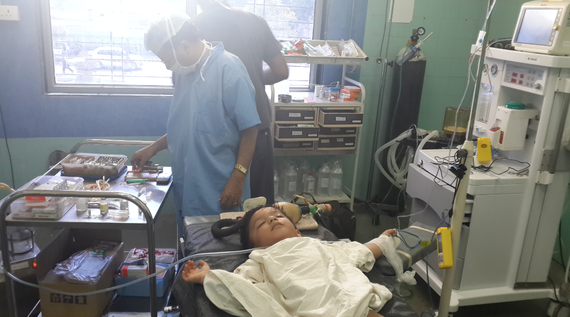
But the stories are there if you look for them, putting statistics - and our fascination with medical dramas - in context.
"Under the shades of a mango tree in Marakwet District, two men restrain a man seated on a locally made stool while the third, armed with a scalpel, slices open his forehead, exposing the skull -"
The poorest third of the world's population receives just 3.5% of the surgical operations undertaken worldwide.
"When it came time for the surgeon to drill holes in the patient's bones, a nurse produced a case containing a Bosch power drill. By way of sterilization, she wrapped it in a green cloth, binding it tight with a strip of muslin."
Surgery is up to 1000 times more dangerous in low-resource settings.
So what's this about a sign, then?
It came in May from the Executive Board at the 67th World Health Assembly in Geneva: "Document EB 135/3."
It asks WHO to propose a resolution "strengthening emergency and essential surgical care and anaesthesia as a component of universal health coverage," and it received universal support from ministries of health across 32 countries. A draft will now be put forward for consideration as an official agenda item at the 68th WHA next year.
This doesn't sound revolutionary - but if global surgery is an unmarked box on the public health 'to do' list, this is the moment power brokers finally decided to pick up a pen.
News travels fast. In politics, academics and the media, conversations about global surgery are rising to the surface.
A recent debate about the valuable contribution of surgery to public health was introduced in the U.K. House of Lords, by surgeon and Lifebox Foundation Patron Lord Bernard Ribeiro. The Lancet published a review proving several surgeries to be cost-effective, rather than a commonly-held extravagance. And an article in the Guardian declared that surgery "should be available to all."
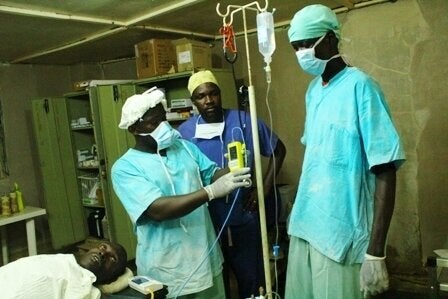
Another recent sign: the week before the Executive Board made their move there was, for the first time ever, a WHA side event dedicated to global surgery. Ministers of health from around the world spoke passionately about the imperative of improving access in their home countries, and congratulated WHO on reaching this milestone.
They also reflected on the time it had taken.
There are healthcare workers in low-resource countries who have waited all their lives for recognition that the people they stitch back together after road traffic accidents, the babies they cut safely from exhausted mothers, wouldn't survive without access to safe surgery.
They recognised the millions more who were not in time.
"Congratulations on this event," said one minister, nodding to the host, "but it has come 30 years too late."
We need to make sure the resolution is signed next year, and in the meantime we need to keep up the conversation - and action - around global surgery.
If it was your life on the line, would you let another decade go by?