Now that the holiday excesses are over, are you thinking about your liver? Worried about your alcohol consumption or maybe feeling bad about all those mince pies (you know, the rich fruit pies that the Brits are so keen on)? Your liver is an incredibly complex organ made up of many different cell types working together - and it plays an important role in your well-being.
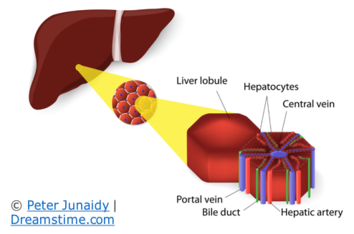
The liver removes toxins (like alcohol and aspirin) and toxic metabolites produced in normal metabolism. It also helps to digest food, it stores vitamins and minerals, regulates your blood sugar and controls your cholesterol levels. Pretty impressive, but this complexity creates a headache for scientists trying to study the human liver so that they can better understand its functions and help develop therapies to cure liver disease.
We know that excessive alcohol consumption seriously damages the liver, leading to liver fibrosis, cirrhosis and even liver cancer. But although alcohol consumption in excess is a behaviour normally only found in humans, research into alcohol-related liver diseases often involves animals. We have heard the stories of animals eating fermented fruits and becoming 'confused', but animals, by nature, don't drink alcohol and do not get drunk.

So, to generate an 'animal model' of alcohol abuse, animals are forcibly dosed with vast amounts of alcohol. The so-called Tsukamoto-French model involves surgical insertion of a tube into the animal's stomach via the neck.

The tube is attached to a syringe system above the cage that then drip-feeds alcohol (or any other toxin or drug) into the animal. Concerns about the lack of natural behaviour aside (animals attached to this sort of mediaeval device cannot move around normally), this approach does not work. Even when animals are continually 'fed' alcohol like this, their rapid metabolism means that they do not generate the high blood alcohol levels typical of people who binge drink nor develop the liver damage and scarring that is associated with alcoholic liver disease in people.
Another common liver disease is non-alcoholic fatty liver disease (NAFLD for short), or hepatic steatosis. This is a build-up of fatty deposits in the liver and affects up to 27 per cent of the industrialised world. NAFLD can progress to the more serious hepatic fibrosis and cirrhosis, but it is readily preventable with reduced fat intake (sorry, you need to cut back on those mince pies). Given that NAFLD is easily preventable, why on earth should animal models of NAFLD exist? In fact, animal models of NAFLD form the subject of 3,153 scientific articles published since 2009. As a fairly conservative estimate, around 67 animals are used for each study--a total of 211,251 mice in less than a decade. That is almost a quarter of a million animals killed for a condition that is reversible simply by moderating fat intake.
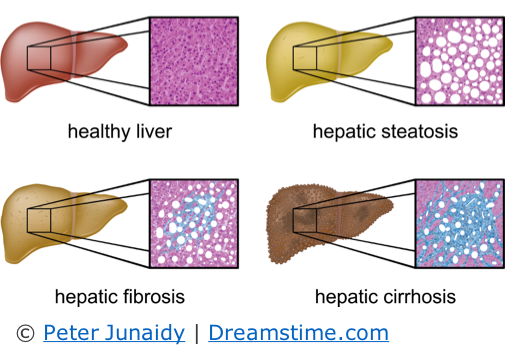
Hepatic fibrosis (or scarring of the liver) is a response to tissue damage. In people, fibrosis is often a result of infection or disease. However, animal models of liver fibrosis are made by deliberately causing damage. There are several ways to do this, each of which involves a crude, unnatural intervention aimed at destroying some or all liver function, rather than recreating how human beings develop liver disease. For example, the chemical carbon tetrachloride is often used to produce liver fibrosis in animals. Does this 'model' human disease? The short answer is no. How can it, when the chances of a person encountering enough carbon tetrachloride to damage their liver is deliberately minimised - the use and production of carbon tetrachloride is strictly regulated around the world. This chemical is classed as an anticipated human carcinogen (likely to cause cancer) and a contributor to global warming! However, mice are injected with this dangerous toxin, and in amounts over ten million times more than people are likely to encounter.
The only way we can get (better) treatments for liver disease is if we appreciate how a healthy human liver operates--and we really do need a better understanding of how the liver works. There are more than 100 different forms of liver disease, and although these have diverse underlying causes (genetics, infections, drug-related damage, etc.), their major common features are that they are chronic, progressing over time, and that we currently have limited treatment options.
However, there is good news. Researchers are having considerable success in developing models of the human liver and in using human cells to create systems in which human liver function and human liver disease (even chronic disease) can be studied. Recently, scientists have made a dynamic model system that assembles several of the different cell types found in normal human liver, and adds a perfusion element to make an 'organoid' that looks and behaves like a human liver. Other researchers are making the most of advances in organ transplantation and using tiny pieces of human liver tissue to examine drug-induced liver injury. The human tissue is ethically harvested from healthy areas of the liver, which has to be removed in the transplant to make way for a new organ, and that would normally be discarded. These approaches allow us to measure human responses to human toxins (alcohol, aspirin, fatty diet, etc). We should follow this lead and leave the rodents to their fat-free, alcohol-free, and altogether healthier lifestyle.