There's an unacceptable public health crisis in Sierra Leone; and it's not Ebola.
The WHO's most recent review of global maternal mortality not only maintains Sierra Leone as having the highest rates in the world, but that those rates are getting worse.
November 7 was the day that the whole of Sierra Leone had been waiting for: 42 days without a single recorded case of Ebola and the outbreak declared over. The collective relief that this brought was accompanied by collective reflection of everything that has passed during this unprecedented outbreak: the cultural shock, national trauma and the international paranoia that resulted in a lethally slow and late response.
The international response eventually kicked into action, with international and humanitarian organisations arriving with big claims; not only were they coming to stop Ebola, they were going to see the whole crisis through to the end. That was the promise of Justine Greening, Britain's international development secretary, recognising the need for a continued commitment to Sierra Leone's health care system after Ebola.
As the international community now adjusts its mindset from Ebola emergency to post-Ebola rebuild, there is talk of the transition from a crisis to a development context. The line between humanitarian and development has always been blurred and debatable. The discourse of development should not overlook that for women's health, Sierra Leone is still very much in the throes of an emergency, however. The humanitarian crisis in that respect is not yet over.
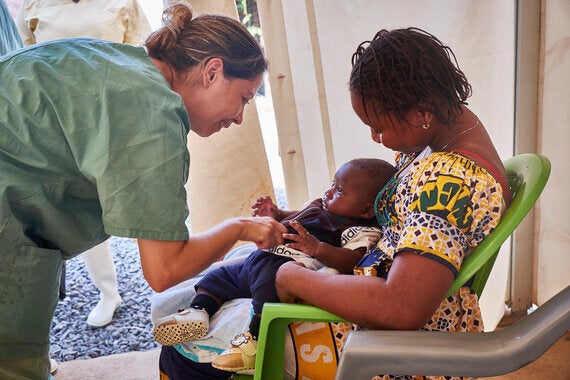
This time last year, I was sitting in a large Médecins Sans Frontières/Doctors Without Borders (MSF) Ebola centre near Sierra Leone's border with Guinea. The epidemic was raging, with more ambulances bringing patients every day, and more expectant faces looking to us for answers. I had come to see a specific patient. She had been making a good recovery, but was in late pregnancy, and there were concerns over her obstetric management. Even after a pregnant woman recovers from Ebola, the pregnancy itself remains infected and potentially contagious.
In that region a pregnant woman is referred to as a Belly Woman, making me the Belly Woman Doctor. Together we made a plan for a safe delivery for her and those who would look after her. She had a risk of haemorrhaging at delivery, so all the necessary drugs were prepared. Clear instructions and training took place before labour began so that everyone, patient and healthcare worker, knew what to expect and how to manage.
She survived Ebola, and she survived childbirth. That makes her one of the lucky ones. Sierra Leone was already the most dangerous country in the world to give birth even before the scourge of Ebola came to pass.
In May 2014, just as Ebola crossed the border into Sierra Leone, the World Health Organization (WHO) ranked the country as having the highest maternal mortality ratio globally. As the epidemic swept down the country, a combination of maternity unit closures and fear of attending health facilities (as places associated with Ebola) left women more vulnerable and with few choices but to hope for the best.
During the epidemic, ActionAid made a prediction that the risk of dying in childbirth could reach up to one in every seven women of reproductive age. Similarly, the UN Population Fund warned in October last year that more than 120,000 women could die across the three worst affected countries in the following 12 months if there was not urgent action to strengthen systems and provide access to family planning and emergency obstetric care.
As we now look forward to the "post-Ebola" era, it comes as little surprise that the situation for women remains tragically hazardous. Just as we now recall our collective failures for a timely response to the epidemic, we are simultaneously dragging our heels in responding to this persisting public health crisis.
The World Bank has calculated that the toll from those who died in the line of duty - the healthcare workers - will leave a deep and lasting legacy on maternal outcomes especially, wiping out hard-earned gains made over the past 20 years, with all three countries being severely impacted. Sierra Leone's maternal mortality is predicted to rise by a further 74 percent from its pre-Ebola levels, essentially making pregnancy a life-threatening event.
The faith of those who need access to maternity services the most has been stretched past breaking point. The Liverpool School of Tropical Medicine recently carried out a series of interviews showing that the little hope that women had in their health services has been crushed by the epidemic. Attending antenatal care and giving birth in a health centre have both reduced, not only due to the lack of access, but out of fear and suspicion.
So it was with open arms that 7 November was received, with those who stepped up to the challenge taking a moment of pride in what has finally been achieved. Though before we polish our medals, hand out awards and pat ourselves on the back, let's take a moment to look at what is left behind. For the Belly Women, the job is far from done and the promise has yet to be delivered.