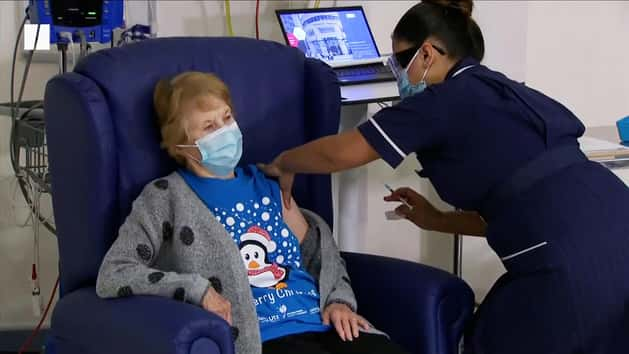
As the coronavirus vaccine rollout takes place across the UK, precautionary advice has been issued that anybody who has a history of “significant” allergic reactions to medicines, foods or vaccines should not receive the jab from Pfizer/BioNTech.
Both staff members had a significant history of allergic reactions – to the extent that they carried adrenaline auto-injectors with them. They are both now recovering well.
From Wednesday, anyone scheduled to receive the vaccination will be asked about their history of allergic reactions.
What is an anaphylactoid reaction?
Anaphylaxis is the result of the immune system, the body’s natural defence system, overreacting to a trigger. Symptoms include feeling lightheaded or faint, breathing difficulties, a fast heartbeat, collapsing or losing consciousness.
Anaphylaxis is a medical emergency and can be very serious if not treated quickly. The NHS advises people to call 999 and ask for an ambulance immediately if someone suffers anaphylaxis, and to use the person’s adrenaline auto-injector if they have one. (One type of auto-injector is an EpiPen, which you’ve probably heard of.)
Does this mean the vaccine isn’t safe?
No. There is always a small chance of experiencing an allergic reaction with any food or medicine.
Professor Stephen Evans, from the London School of Hygiene & Tropical Medicine told the BBC: “If you mean absolutely no adverse effect, then no vaccine is ‘safe’ and no drug is ‘safe’. Every effective medicine has unwanted effects.
“What I mean by safe is the balance of unwanted effects compared with the benefit is very clearly in favour of the benefit.”
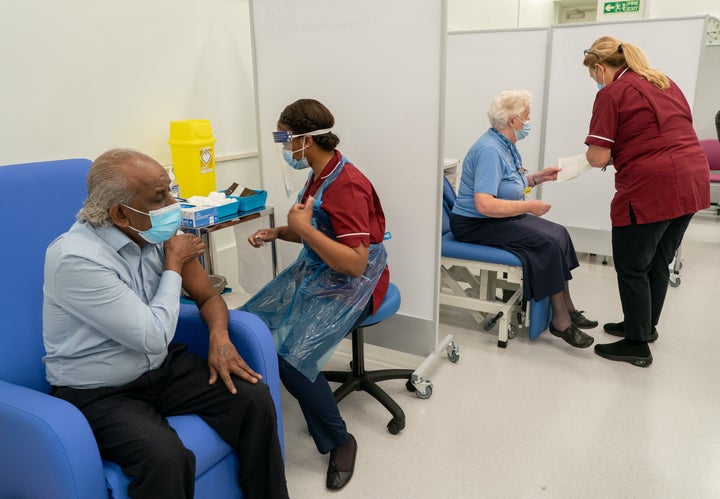
According to research, anaphylaxis to vaccines occurs in about 1 in 760,000 vaccinations. You are more likely to be struck by lightning (1 in 700,000). The UK has one of the highest coronavirus death rates in the world, with some estimates stating one in a thousand people have died after being infected by the virus.
Peter Openshaw, past-president of the British Society for Immunology and professor of experimental medicine at Imperial College London, explained: “As with all food and medications, there is a very small chance of an allergic reaction to any vaccine.
“However, it is important that we put this risk in perspective. The occurrence of any allergic reaction was one of the factors monitored in the phase 3 clinical trial of this Pfizer/BioNTech Covid-19 vaccine, the detailed data from which was released yesterday.
“In this, they reported a very small number of allergic reactions in both the vaccine and placebo groups (0.63% and 0.51%).
“Similar to the rollout of all new vaccines and medications, this new Covid-19 vaccine is being monitored closely by the MHRA.
“They will now investigate these cases in more detail to understand if the allergic reactions were linked to the vaccine or were incidental.
“The fact that we know so soon about these two allergic reactions and that the regulator has acted on this to issue precautionary advice shows that this monitoring system is working well.”
Should I still take the vaccine?
If you do not have a history significant allergic reactions and are not undergoing medical treatment or have a compromised immune system, then yes. The vaccine is safe, as the NHS explains here.
It isn’t just that it will provide protection against Covid-19 (up to 95%, according to its phase 3 trial) – a disease that has already killed more than 62,000 Brits, and more than 1.5m globally.
The fact that some people can’t take it (for instance, because of allergic reactions) makes it even more important that other people do. As explained by the NHS, the more people who are immune, the less chance there is that someone who can’t take the vaccine will be exposed to the virus.
Dr Jennifer Rohn, a medicine cell biologist at UCL, told us last month: “Not everyone can get vaccinated. There are people who are too vulnerable and they’re immunocompromised and they’re relying on everyone else to do the right thing.”
Who shouldn’t take the vaccine?
The MHRA advice states: “Any person with a history of a significant allergic reaction to a vaccine, medicine or food (such as previous history of anaphylactoid reaction or those who have been advised to carry an adrenaline auto-injector) should not receive the Pfizer/BioNTech vaccine.”
The patient safety leaflet for the vaccine cautions that anyone with an allergy to any of the active substances in the vaccine should not receive the jab.
It adds: “Signs of an allergic reaction may include itchy skin rash, shortness of breath and swelling of the face or tongue.”
People undergoing certain medical treatments or those with compromised immune systems may also not be able to safely take a vaccine.
As such, they will be relying on the wider population to take the vaccine, develop herd immunity, and therefore indirectly protect them from Covid-19.
Herd immunity for a disease is typically achieved when between 70 and 90% of a population is vaccinated.