
The UK is experiencing yet another wave of Covid infections, with case numbers rising by half a million in a week.
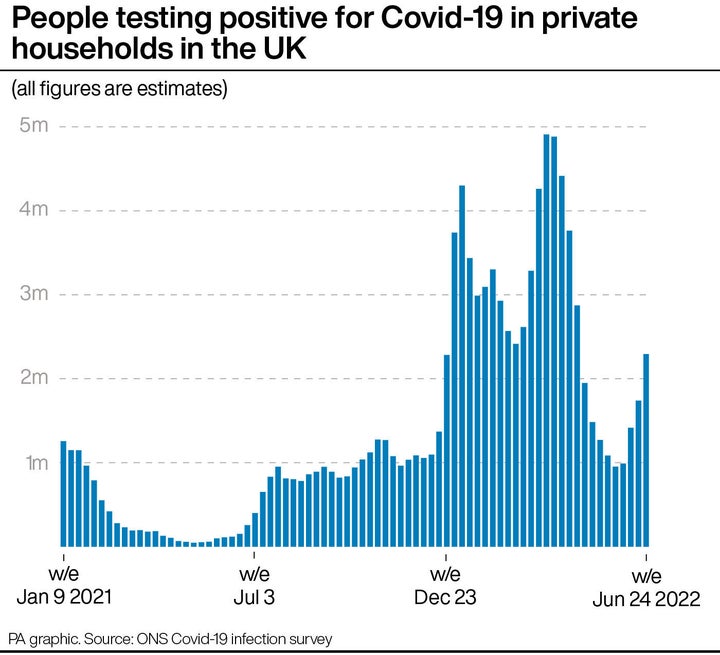
According to the Office for National Statistics (ONS), an estimated 2.3 million people had the virus last week, which is an increase of 32% compared to the week before.
While this is the highest recorded number since late April, it is still lower than the peak seen at the end of March, where Omicron BA.2 (the stealth variant) led to a record 4.9 million cases.
But more than two years into the pandemic and several variants later, how do we tell a mild infection from a more severe one?
Here’s what you need to know.
Why are cases rising?
The incline in case numbers comes down to two new strains, BA.4 and BA.5, which are sub-variants of Omicron. They were labelled as “variants of concern” by the European Centre for Disease Prevention and Control in May.
The UK Health Security Agency (UKHSA) claims BA.5 is growing 35% faster than BA.2, while BA.4 is growing only 1% faster – meaning BA.5 is dominant.
These two strains spread very easily and appear to dodge antibody responses from both those who have natural immunity and have been fully vaccinated.
They supposedly have mutations on their spike proteins, which enable them to retrain their attacks on human lung cells.
Vaccines will still protect against severe disease according to specialists, although rising hospitalisations are still a cause for concern.
It’s been around six months since most people in the UK received their booster jab as part of the winter rollout programme, meaning vaccine efficacy is waning.
Increased socialising at major events such as the Jubilee bank holiday weekend and the return of festivals like Glastonbury will have accelerated case numbers, too.
What are the symptoms of BA.4 and BA.5?
Despite te fresh concerns around the new sub-variants, the UKHSA claims there is “currently no evidence” they cause more serious illness than previous strains, or come with new symptoms.
Breathlessness and a loss of taste or smell were more common with previous strains of the virus, such as Alpha.
Symptoms include:
Cough
Runny nose
Sore throat
Fatigue
Headache
Muscle pain
Sneezing
Pain
So how do you know if you have a severe infection?
There is a key sign which sets mild infections apart from more severe disease.
Dr Dan Goyal, a consultant in internal medicine in NHS Highland, pointed out that it comes down to your breathing.
In a Twitter thread, he wrote: “To be absolutely clear, shortness of breath is NOT a ‘normal’ feature of Covid.
“Shortness of breath indicates severe Covid (or worse) until proven otherwise.”
He suggested that Silent Hypoxia is an additional major concern, and “the most challenging part of Covid management”.
This is when the oxygen in your blood is very low, but the patient is not aware of any related symptoms. Dr Goyal describes it as where the “lungs are inflamed but you don’t feel short of breath”.
To detect this, he recommended buying a pulse oximeter from your local pharmacist. This measures how much oxygen is in your blood.
Dr Goyal said levels of 95% or more is OK, but below 95% needs medical input. When the oximeter shows 93% or 94% oxygen levels, that means you need support from the GP and if it 92% or lower, you need to go to A&E.
Other signs include feeling flu-like symptoms, severe fatigue from small amounts of exertion (like walking up the stairs), any fever lasting more than a few days and any signs of confusion were further warning signs.
What to do if you test Covid positive?
Now there are no official measures in place to reduce transmission among the general public, it’s not clear how people are supposed to respond if they do test positive.
It’s best to self-isolate if you can. If you have a mild case, it should resolve itself within a matter of days. However, this is not the case for everyone and severe disease can develop for some people. Any breathing problems are a danger sign and need medical attention.
Dr Goyal recommended people should ask themselves: “If this wasn’t Covid, would I contact a doctor?”
Pushing yourself to carry on with regular activities can worsen recovery, so wait until you are completely better before returning to your regular day-to-day life.
If you are a high-risk group, you might be eligible for anti-viral therapies which reduce hospitalisation and the overall health risk that comes with catching Covid.
However, you have to take them before the end of day five of symptom onset for them to have an effect.
How can you avoid Covid?
Ventilation and face masks are still key to protecting yourself against infection.
Covid can linger in the air for hours, so open doors and windows where possible.
Vaccines are “a game-changer”, says Dr Goyal, in terms of lessening the severity of the virus, meaning even those hospitalised have a good chance of recovering if fully vaccinated.
Getting fit also reduces your chances of contracting severe disease, as well as wearing the more protective FFP2 masks.
As Dr Goyal noted: “The long and the short of [is] the least number of infections you get the better, and the longer you delay getting infected the better the treatments get. A wee bit of effort is worth it just now.”