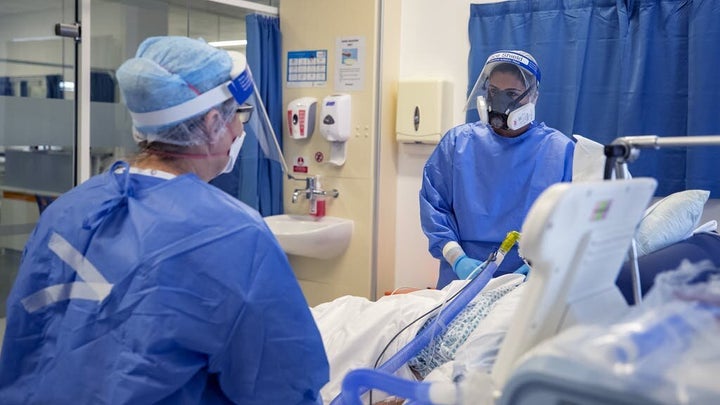
It’s difficult to understate the effect one announcement made last summer about a cheap, safe and readily available drug called dexamethasone, had in the fight against the coronavirus pandemic.
“It sort of changed the world,” says Professor Martin Landray, one of the chief investigators behind the trial that led to its approval and widespread use.
“We announced the results at lunchtime on the 16th of June and by teatime it was NHS policy at the behest of the chief medical officer, and it was saving lives by the weekend.”
At the time, the worst of the first wave was over but with social restrictions still in place, the threat of a second wave on the horizon and vaccines still months away, the entire world was desperate for positive news.
Hailed as the “a major breakthrough”, the news the drug reduced deaths by up to a third among patients on ventilators, and by a fifth for those on oxygen, made headlines around the world.
Since then, dexamethasone has largely kept out of the news but that’s a disservice to its success.
Dr Daniele Bryden, vice dean of the Faculty of Intensive Care Medicine, told HuffPost UK: “You’re probably not hearing about it because it was adopted so rapidly.
“People just took the trial information and said ‘yes, this is what we must do’.”
As the pandemic has continued, this has translated into huge numbers of lives saved.
“It’s quite possible that 12,000 lives [in the UK] have been saved from one cheap, cheerful and relatively well-known drug,” says Prof Landray.
“If we’d known about dexamethasone at the beginning of the epidemic then about 6,500 people would have survived.”
Dexamethasone is a widely-used steroid drug which works to reduce inflammation and is used to treat a number of different conditions, including rheumatoid arthritis and asthma by suppressing the immune system.
The drug was developed way back in 1957 and was first approved for medical use by the Food and Drug Administration in the US in 1958.
It’s also cheap – the cost of a course of treatment for people seriously ill with coronavirus is about £5.
Prof Landray led the Recovery trial – which stands for Randomised Evaluation of COVid-19 thERapY – which recruited 2,104 patients whose outcomes were compared with a control group of 4,321 patients.
The results were startling. “If you treat eight people with it in intensive care, one of the them will walk out alive specifically because of it,” says Prof Landray.
What’s even more remarkable is that in the early days of the pandemic, the general consensus was drugs like dexamethasone wouldn’t work when treating Covid and could even make things worse.
“The general guidance was that steroids shouldn’t be used, that suppressing the immune system when the body is fighting infection is a bad idea,” says Prof Landray.
But when the pandemic began, there wasn’t the time nor sufficient knowledge of the virus to develop new drugs to fight it so scientists had to work with what they already had and trialled a number of treatments.
“We started the year thinking it was a virus illness like flu, and we’re finishing the year very much recognising this is a disease process that affects blood vessels everywhere and it’s an inflammatory process that can be very widespread,” says Dr Bryden.
But despite its numerous plus points, the fact remains dexamethasone alone is not enough in the fight against coronavirus.
“It is still the only drug that’s been demonstrated to save the lives of patients with Covid,” says Prof Landry.
The Recovery study, co-ordinated by the University of Oxford, is also looking at a number of possible treatments including Regeneron Pharmaceuticals’ experimental antibody drug REGN-COV2 which was given to Donald Trump.
It is also testing the antibiotic Azithromycin, anti-inflammatory drug Tocilizumab, and convalescent plasma as well.
“Patents today are benefitting from the participation of patients in the first wave in the UK. And patients today are entering trials for other treatments – but we don’t know if they’re any good or not.
“If you look at the US, 100,000 Americans have been given convalescent plasma but we don’t know if they’re the lucky ones or if it’s made no difference at all.”
The development of vaccines has been the biggest leap forward but coronavirus will not disappear soon and people will still contract it meaning many more dexamethasones will be needed, possibly for years to come.
