Scientists may have finally proved that the pen is mightier than the scalpel after they developed a prototype for a cancer-detecting ‘pen’ to be used as a tool in surgical procedures.
The ‘MasSpec Pen’ is a tool that reportedly can detect cancer within 10 seconds and is accurate more than 96% of the time, according to the team at the University of Texas who have built the one-of-a-kind object.
Conventional methods of testing for cancerous cells usually take several days for pathologists to anaylse biopsied tissue samples in a laboratory.
But this means that during live surgery, surgeons who are trying to remove cancerous tumours are not able to categorically say that they have removed it in it’s entirety because there is no way of testing on the spot.
Lead author Jialing Zhang said: “Although a surgeon’s goal is to remove cancer in its entirety during excision surgery, achieving negative margins [an absence of cancer cells at the outer edge of the excised tumor specimen] can be challenging.”
This means that they are either prone to removing too little (and the tumour re-growing) or being over cautious and removing too much which can lead to pain, nerve damage and deformation.
Thyroid patients can lose the ability to speak if too much tissue is taken out.
Livia Schiavinato Eberlin, assistant professor working on the study, said: “If you talk to cancer patients after surgery, one of the first things many will say is ‘I hope the surgeon got all the cancer out’. It’s just heartbreaking when that’s not the case.”
However the MasSpec pen can do this same testing with instant feedback - nearly 150 times faster than existing technology - meaning surgeons could know either way.
“Our technology could vastly improve the odds that surgeons really do remove every last trace of cancer during surgery,” said Eberlin.
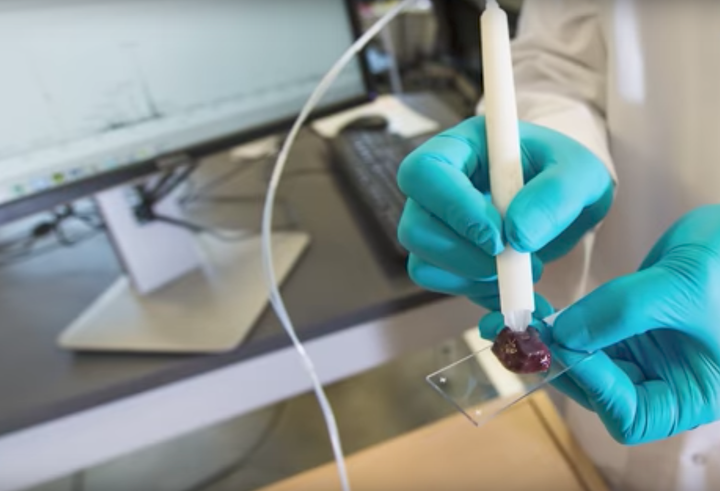
The pen works by releasing a tiny droplet of water onto the tissue, which soaks up chemicals inside the cells. The water is then sucked back up and analysed by an instrument known as a mass spectrometer, which can detect thousands of molecules and identify compounds associated with cancer.
Algorithms then produce a conclusion on whether the tissue is likely to be safe.
The team hope that the technology could be used by oncology teams as soon as 2018.
