In an hour and a half of interviewing Sarah*, I would never have suspected she had taken heroin that morning. Her West London basement flat contains none of the chaos and disorder you might associate with a daily user. The living room is clean. The only item lying on the floor is a food bowl for her cat that comes in and out as we speak. The shelves are full of books with titles such as Prescription Drugs: Alternative Uses, Alternative Cures alongside River Cafe cook books and novels.
Each morning, Sarah, 47, intramuscularly injects a dose of heroin just after she gets up. She injects again in the afternoon - around 5pm if she has been out working or volunteering - and then injects again at bed time. All told, she takes 300mg of the drug a day. All of Sarah’s drug taking paraphernalia is clean and neat.
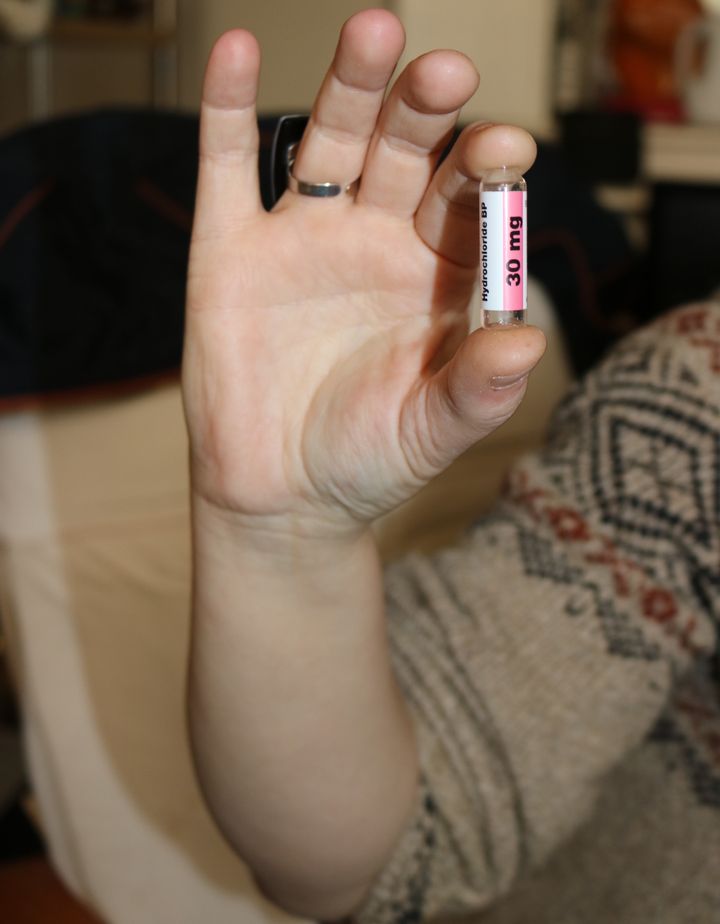
Tomorrow, she will need more heroin. She will hit the streets, not in search of a dealer, but a chemist. She goes to a specialised clinic for addiction, speaks to her key worker about how things are going and receives her prescription. This gives her two weeks’ worth of freeze dried ampoules of diamorphine - the medical term for heroin - clean syringes, sterile water and alcohol swabs, for free, from her local pharmacy.
Heroin prescription has been a part of Britain’s approach to drugs since the 1920s, but the public is largely ignorant of its existence. The policy was so rare internationally it came to be dubbed “The British System”. The Home Office licenses doctors to prescribe diamorphine to those who do not respond to alternatives like methadone or morphine. Possession of diamorphine, a Class A Drug, would ordinarily mean a prison sentence of up to seven years.
Sarah has been on her prescription for 14 years. She became addicted to heroin after leaving home in her native Australia aged 15. This take-home prescription follows repeated failures of what she calls “the methadone merry-go-round”, when she took the substitute given to addicts that failed to suppress her urge. She is determined to come off her prescription but fears, if she relapses, she would not get it back.
Sitting in her living room, I ask where she would be without it. She pauses for 15 seconds, chewing over her thoughts. “God, I don’t know,” she says. “When I asked for this prescription I felt like this was it, this was the last thing that was available.
“I didn’t know what would happen to me if I couldn’t get it. I know that sounds crazy really, because you think ‘just stop, just get it together and fucking stop’. But I think sometimes, when you get to a place when you’re so entrenched or enmired in your situation, drugs are all around you all day...
“I always remember this guy saying ‘when you’re on the bottom rung of the ladder, everything is above you’. You just feel it’s almost insurmountable. Having that prescription really gave me the first tool I really needed to climb out of that mess.”
Sarah speaks slowly and carefully. She is advocating legal, free diamorphine for those who need it in a world where “people just see junkies. They just see heroin. They just see the damage heroin causes”. She wants to get this right.
Sarah may not know where she would be without a diamorphine prescription but the troubles she faced without it paint a bleak picture.
After leaving home as a teenager, Sarah was interested in experimenting and took heroin and speed. It wasn’t until she had a boyfriend who was regularly using heroin and the drug was “around all the time” that she started using regularly too and became addicted. She woke up one day “sick” and “incredibly anxious”. “It’s like this anxiety is in under your bones, you just can’t think straight,” is how she describes the withdrawal symptoms. Sarah, who was by now working as a prostitute, used methadone but found, while it alleviated the symptoms, she still needed her fix.
In 1993, in her early twenties, Sarah came to Britain, something her mother hoped would help her come off drugs. She continued to try and get off heroin using methadone but, still surrounded by contacts and friends she would score with, she kept using. “Heroin doesn’t work as well on methadone. If you’re not ready to stop, you take pills on top to make the heroin when you do score better.” The need for a fix was like “running on a treadmill”, she says. “It’s all that you have time to think about and do every day. It takes all that time to work out how you’re going to get the money. Then try to score. Then, sorting out your gear, having your little chill and then it all starts again.”
Sarah makes a motion with her hands like she is ringing water from an imaginary towel, still deliberating over the words she chooses. “The heroin stops the sickness but also that desire to get heroin. Maybe it’s having a fix... I’m sure that’s got something to do with it... That process... that instant gratification. There’s something incredibly satisfying about when you feel a bit wired or sick or anything and then have a hit, bam, instant, fixed.”

Sarah stopped working as a prostitute when a boyfriend, who did not tell her he was HIV positive, gave her the virus. Her mum, who had moved to Britain, came with her for an appointment for blood tests. This moment brought the stigma around addicts into sharp focus. The doctor, Sarah is adamant, assumed she had contracted it through a dirty needle. The doctor was “condescending, judgmental” while asking blunt questions about her sex life and drug taking, leaving Sarah and her mum fearing she was a low priority on the treatment. She recalls thinking at the time: “I don’t want to be in this situation, but my life’s in your hands now and because of my drug use, I could not get what everyone else gets because you just see ‘junkie’.”
After years on methadone, another doctor asked her what she felt she needed. “Heroin script, actually,” she said, not aware such a thing was actually possible here. But the doctor explained it was. Sarah initially went to a clinic where she had to go every day, take her diamorphine ampoules to inject at home and then return the empty ones the next day, without which she would not receive her next dose.
She calls the environment “terrible”. The doses were too small and patients would top up with other drugs but then lie about it for fear of having the prescription withdrawn as punishment. The constant attendance requirements made it hard to escape the circles that kept her in heroin’s orbit. She once saw a man in the waiting room whose skin had turned yellow. He told her he had developed an abscess on his rear and lowered his trousers to show a huge patch of black skin. He kept it from the clinic for fear of losing his methadone prescription. He didn’t even go to the adjacent hospital.
Sarah left the clinic and returned to a methadone prescription. She was only able to move to a take-home diamorphine prescription when a friend came off theirs and Sarah took the place. “When I walked in that door to plead for that prescription, I was taking everything, I was even drinking, which I never did,” she says. But once she had this prescription this “just all fell away... I think it was important to feel trusted by the doctor, to be able to get out of my living situation... It was just full of daily drug activity.” After a few months, the doctor eventually agreed to let her take the diamorphine out of London, to stay with her mum in Essex for six months.
Together they would make trips back to London to gradually clean out the flat of gear she had used to take heroin. Contacts connected to drugs stopped ringing. Sarah eventually returned to London. “The difference was like night and day,” she tells me of the change. “Diamorphine, it just knocked on the head all that scoring on top.”
Her addiction and fight for the prescription made her something of an expert in the field and a passionate advocate for drug users. She went on to found a magazine that aimed to “get the medical profession to hear the voices of people who use drugs”. She volunteers on a drugs helpline. She advocates for more doctors to be able and willing to prescribe diamorphine but fears fewer and fewer people are getting it. She dismisses concerns that people who take it home will sell it on. “People aren’t going to sell their pharmaceutical heroin. For what? Street heroin? To go through these hurdles to get on these programmes, heroin’s got to be your problem. Why you would sell that? It doesn’t make sense.”
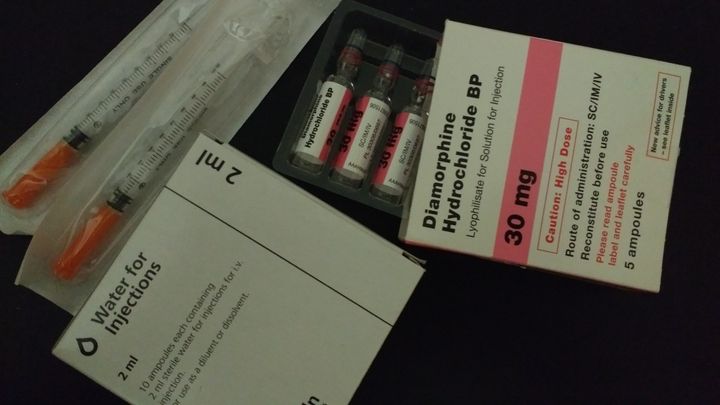
She once gave a presentation showing two photos of her coffee table, one from when she was using street heroin and the other from when she was on the prescription. “With street heroin, you saw spoons, syringes... You can get blocked syringes if your veins are bad... It’s all messy, there’s tissues and lighters to light the spoon. There’s citric to dissolve the heroin, a tourniquet and belts.” The picture contrasted with the picture of her table while on the prescription - clean syringes, water and a box of ampoules.
Sarah has never developed an abscess from injecting her prescribed diamorphine, which, she emphasises, is a “cleaned up” version of street heroin. She compares taking it to taking any medicine. She does not sit back and space out for hours. With the tolerance she has built up, she can inject, get up and go on with her day. “You wouldn’t know I’d had it,” she says. She has brought her dose down to half what it was because the higher amount left her tired. She believes her dosage is about as low as a heroin addict would go. “Methadone is like a heavy coat you wear. It’s not your coat but it keeps you warm. Heroin feels like your clothes. It doesn’t feel as heavy. It doesn’t feel as depressing.”
But Sarah fears Britain is moving away from this system and other addicts in desperate straits are not getting it, denying them the chance she had. “Very few doctors able and willing to prescribe diamorphine and they don’t particularly want to take on new ones,” she says. “I know people now, with a leg missing, who are still shooting up... But they still can’t get it.”
Gary Sutton, a drugs counsellor and head of drugs services at Release, a charity which offers advice and support around drugs and the law, thinks Britain is going “backwards” and insists the numbers receiving diamorphine have fallen.
Sutton recalls former Home Secretary David Blunkett mooted expanding heroin prescriptions in the early 2000s but Blunkett ultimately “moved on” without any significant change. One drug expert estimates there were 400 addicts receiving diamorphine around this time. Media cite figures between 400 and 500 in the early and mid 2000s. In 2008, The British Medical Journal estimated it was around 300. These numbers are dwarfed by the numbers on a methadone prescription. Another study found diamorphine prescriptions had lasted six years on average. But in 2010, the new National Drugs Strategy said “far too many” addicts were languishing on prescriptions that were not proving to be “the first step on the journey to recovery”.
Sutton believes many have been “bullied off” their prescriptions in recent years, adding the current figure is “probably less than a couple of hundred, probably quite a lot less than a couple of hundred”.
As a psychotherapist, Sutton has worked with many people who suffered some form of trauma early in their lives. He says opiates like heroin can help distance them from the feeling this evokes.
“People who are attracted to opiates are often people who have difficulty relating to other people, they often have attachment issues, they’re frequently victims of childhood abuse and neglect,” he says. “I do think that most people who find themselves drawn to opiates on long-term basis have suffered some kind of early-life trauma that they find it extremely hard to compensate for and opiates just give you that distancing.
“You’re aware of the hurt but you don’t feel it with quite the same intensity. There are exceptions but I think that’s a pretty strong an accurate rule of thumb.”
But he concedes diamorphine prescription can be far more expensive than methadone. He checks the price of a 100mg freeze dried diamorphine ampoule - £9 - and works out the annual cost of the average prescription for addict is around £14,500, just for the medication. Methadone supplied daily through pharmacists, he estimates, would be less than £2,000. “It’s a difficult choice to make when you have a limited amount of money,” he says. He emphasises it would be cheaper to provide diamorphine by tablet or powder but the Home Office prefers it to be in ampoules.
Sutton advocates take-home diamorphine prescriptions of the kind Sarah has. “For many people, the most effective way to provide this as a treatment is to give it to people at an appropriate dose and allow them to collect it... Then you’re creating a base from which people can go out and get on with living, without all the distractions and interruptions and social problems that come with having to find the money and score illegally.”
Sarah had plans to come off her prescription. She applied to do a Master’s degree in media, campaigning and social change that would have begun in September. She hoped her track record in activism would substitute for the normally required Bachelor’s degree. But, having left school at 14, she was rejected. She had planned to ditch the prescription after finishing the course.
Sarah: “By the time you get to my age, you’ve got a history of a lot or relapses. The thought of giving up... It’s something I want to do, it’s something I don’t want to get wrong... I don’t want to make a mistake.”
She is self-conscious telling people she has been on it for more than a decade, fearing they’ll say: “Oh, well you’ll be on it forever.”
“It’s not like that... There really is that worry that I won’t get it back... It’s not just like, if you’re a drinker and you stop drinking and you go the pub one day and you have a drink: That’s not going to kill you. But a relapse, when you have low tolerance, that’s when people die. That’s probably when most overdoses happen... They’ve lost their tolerance, they have just a bit. They’re not with someone. They’ve had it. It’s so dangerous.”
“I’d never get this prescription back,” she adds. I ask why she thinks so. “I know so. Once I walk out this door, it closes behind me.”
*Sarah is a pseudonym
