Fertility struggles are still so shrouded in secrecy that many women have little to no idea about what to expect from IVF until they’re seeking treatment. While IVF stands for ‘in vitro fertilisation’ – the attempt to fertilise an egg with sperm in laboratory conditions – the process before and after that moment very much involves your body, so it’s worth preparing for the physical impact.
Treatment plans will look different from woman to woman, with the type and frequency of drugs tailored to the individual – but IVF does follow some key steps. A treatment cycle usually lasts between four to six weeks, though again this can vary and some women will have multiple cycles trying to conceive.
To help you make an informed choice, we asked fertility experts to explain exactly what happens to your body during IVF and how it’s likely to feel.
Step 1: Preparing For IVF
Before you can begin treatment, doctors will need to take a look at what’s going on inside your reproductive system so they can create a treatment plan with the best chance of success for you.
Doctors will check your ovarian reserve and blood flow to the ovaries, examine the womb and conduct any further tests relating to potential problems they may spot along the way.
This preparation stage usually consists of three to five visits to the IVF clinic for blood tests and ultrasound scans, explains Dr Geeta Nargund, medical director at Create Fertility.
“These should be straightforward, and although the scan is an internal one [the probe is inserted via the vagina] there should be little discomfort, certainly a lot easier than a smear.”
Step 2: Suppressing Your Menstrual Cycle
Doctors will advise whether or not you need to suppress your menstrual cycle, depending on the results of your tests, and your individual circumstances and medical history. Women who have ovarian cysts or suffer from endometriosis may require long-protocol oestrogen suppression drugs, for example – but most other women will not.
“This may involve taking the oral contraceptive pill or an injection you will take each day [for up to two weeks], or even a nasal spray,” explains fertility expert Dr Larisa Corda. “Some of these drugs may temporarily put you in a mini menopausal state, where you can experience hot flushes, night sweats, headaches or mood swings.”
If the side effects become debilitating, your doctor may be able to give you additional medication to counteract them.
Step 3: Egg Stimulation
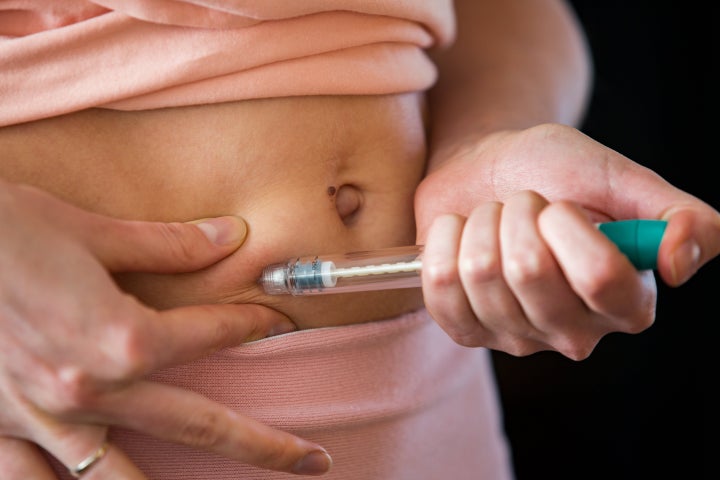
Following on from this – or if you don’t require any suppressing drugs – you will be given a cocktail of fertility hormone drugs tailored to the individual, primarily designed to increase the number of eggs that you produce. “This is a daily injection you give yourself, usually for about 10 to 12 days,” explains Dr Corda, ”but this will vary depending on your own personal response, which will be monitored with regular ultrasound scans and blood tests.”
Injections are designed to be administered via the stomach area or upper thigh – if this sound worrying, rest assured that clinics will provide you with an injection lesson so you know what you’re doing.
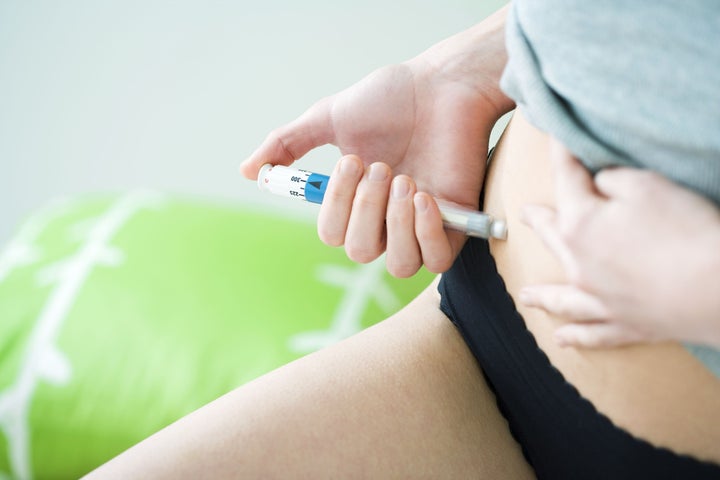
“Injections are done under the skin and some patients might get light bruising that normally disappears within a couple of days,” says Dr Nargund. “If you develop any heavier bruising or an allergic reaction to the injections then it is vital you flag this to your clinical team.”
Some women will also experience mood changes and pre-menstrual symptoms while taking stimulation injections. “The drugs are not without side effects as some women can develop an over-response to the drugs that puts them at risk of developing OHSS (Ovarian Hyper Stimulation Syndrome),” Dr Nargund adds.
This is where your ovaries produce too many eggs in one cycle. “In its mild form you may feel bloated or uncomfortable, but in its most serious form you may develop vomiting or other symptoms, which may require hospitalisation.”
Although OHSS is extremely rare, if symptoms become worse than bloating you should contact your clinical team for advice right away. “If a woman develops OHSS in an IVF cycle and gets pregnant, there is an increased risk of her developing clotting disorders, such as deep vein thrombosis or clotting within the lungs,” explains Dr Nargund – and there can be risks of premature birth.
Step 4: Egg Collection
Egg collection is done under sedation, so you will not feel the actual process. Most women are put to sleep with general anaesthetic, but some clinics will offer local anaesthetic.
“Your eggs will be collected using a needle that’s passed through the vagina and into each ovary under ultrasound guidance,” explains Dr Corda. “This is usually a minor procedure that takes about 15 to 20 minutes.”
Some women experience tummy cramps or a small amount of vaginal bleeding after this procedure, Dr Corda adds, so you will need to take the day off work to recover. You will also be given antibiotics to reduce the chance of infection.
Experiencing discomfort in the pelvic area after the procedure is also common, adds Dr Nargund: “Pelvic discomfort should only last a day or so, but if you begin to feel worse or have abdominal pain then it is important you speak to your doctor.”
Your eggs can be frozen at this stage if you want to delay using them, or you can undergo the next stage (fertilisation) and freeze the embryos.
Step 5: Fertilisation and Preparation For Embryo Transfer
The eggs that have been collected will be mixed with sperm from your partner or donor sperm in a laboratory and after a day, are checked to see if they have fertilised. “Sometimes the process may need additional help where sperm is injected directly into the egg, something called intracytoplasmic sperm injection (ICSI),” explains Dr Corda.
Your embryos will be frozen if you wish to delay transfer, or if you’re opting for a “fresh transfer”, one or two of the eggs will be selected to be placed inside the womb a few days after egg collection. Although there is no physical impact during this stage, you will need to be in regular contact with your doctors for updates.
“Your doctor will give you progesterone injections or pessaries to take to prime the lining of the womb ready to receive the embryo/embryos,” says Dr Corda.
Step 6: Embryo Transfer
The embryo transfer process is relatively straightforward and “is much like having a smear,” explains Dr Nargund. The process is usually done without anaesthetic and involves inserting a speculum and a small plastic tube via the vagina. “It usually takes 10 to 15 minutes and is painless,” adds Dr Corda.
You’ll then need to wait around two weeks before taking a pregnancy test. Depending on the results, your clinic will inform you of the next steps you should take. This might include information about check-ups if you’re pregnant, advice on trying again – or where to access support if you choose not to.
As well as the physical impacts of IVF detailed within this article, undergoing IVF can be an extremely difficult process emotionally, regardless of the outcome. Talk to your clinic about counselling services or visit Fertility Network UK and Fertility Friends for online forums where you can find other people who have experienced treatment.
