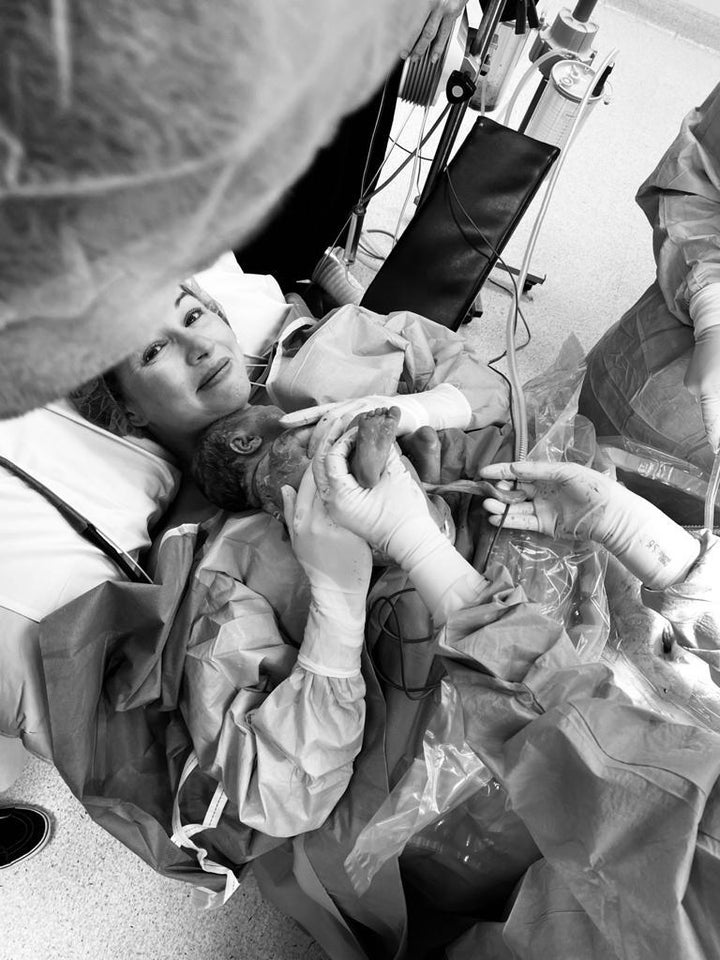
When you picture the moments after birth, you imagine a baby being placed on the mother’s chest. Occasionally, birthing people even reach down and grab their babies themselves, as Kourtney Kardashian famously did when delivering daughter Penelope in 2012.
“I remember always seeing scenes of women giving birth and feeling terrified, so when I had my birth experience, and it was so incredible and amazing, I just remember wanting to share that to help other women maybe not feel terrified or have that perspective,” Kardashian told Variety last year when reflecting on the experience, which was aired on “Keeping Up with the Kardashians.”
Even in the bare-it-all reality genre, the images of Kardashian catching her babies were unusual. We aren’t accustomed to seeing a real newborn, slick with blood and waxy vernix, at the moment they emerge. We also aren’t used to seeing a mother actively participate in her own birth in this way.
If we do hear about a person delivering their own baby, it’s sometimes because they accidentally ended up giving birth in their car, or perhaps as part of a planned home birth.
But what if an experience like that was made available to more birthing people, even those who deliver via c-section — as almost one-third (32.2%) do? The idea of a woman participating in her own surgery might sound far-fetched, but proponents of the practice, known as maternal-assisted caesarean, say that it is not only possible but of benefit to the mothers who choose it.
What is a maternal-assisted caesarean?
A maternal-assisted caesarean involves the same instinctual move that Kardashian made in her deliveries, only instead of reaching down between her legs to lift the baby to her chest, the woman reaches toward the incision in her lower abdomen. (Note that she doesn’t reach into the incision, but takes hold of the baby after a doctor has gotten out the head and shoulders.)
This changes the way the surgery looks, primarily by removing the drape that generally separates the patient’s head and chest from the lower half of her body. In addition to lifting her baby to her chest, she has a full view of the surgery itself.
This means that a woman scrubs into the surgery alongside her doctor, thoroughly washing her hands and forearms, using a nail brush, before donning a pair of sterile surgical gloves that she will wear when she reaches for her baby. Because such preparations are necessary to prevent the chance of infection, only planned c-sections, not emergency ones, can be maternally-assisted. (Note that “emergency” here means the c-section was unplanned, not necessarily that anyone’s life was in danger.)
Maternal-assisted caesareans are not common, and not all doctors will agree to participate in one, but women who have had this type of c-section say that being able to take an active role in their delivery made all the discussion, planning and preparation well worth it.
What are the benefits?
For a woman hoping for a vaginal birth, and a level of control over her birth experience, learning that she will need a c-section may cause frustration or disappointment. Choosing a maternal-assisted caesarean can, for some mothers, make the birth experience more satisfying and meaningful.
“I had experienced a vaginal delivery for my first birth and a c-section birth for my second birth,” Lyz Evans, an Australian physiotherapist (the term physical therapist is more common in the U.S.) told HuffPost.
Evans, who co-founded an exercise program called Empowered Motherhood, used the words “clinical” and “disconnected” to describe her first c-section experience. “You are numb from the chest down, lying flat on your back and have a drape separating you from the birthing team and the surgery,” she said.
In a maternal-assisted caesarean, however, “the drape is removed so you can watch the procedure, and because you are able to reach down and pull your baby out of your stomach yourself, you feel like you are really involved in the process, and that can be so empowering and incredible,” Evans said.
Evans had first heard of maternal-assisted caesareans on South American social media, and wondered why the procedure wasn’t offered more widely. When she was preparing for her third birth, she thought of this option and how it would help her play an “active role.”
The hard part, she said, was convincing her doctor, who had never performed a caesarean in this way before, to do the procedure, and the hospital to allow it.
What are the safety considerations?
The chief safety concern is “the risk of contaminating the sterile field where the surgery is taking place,” Dr. Josie Urbina, an OB-GYN at the University of California San Francisco, told HuffPost. Urbina performs traditional c-sections and explained that “usually patients are behind a non-sterile curtain accompanied by their partners, doulas and the anaesthesia team.”
Removal of the curtain so that the patient can reach down for her baby would make it difficult to maintain a sterile operating field, Urbina said. The team would have to get creative: “If there’s a way to make the patient sterile to help receive their baby, then that may decrease the risk of contamination, and as a result, decrease risk of infection of their incision and/or uterus after c-section.”
An infection, she said, would “delay wound healing” and cause increased pain. Such infections can also become serious.
The procedure is only possible for planned c-sections, and for low-risk pregnancies. Your doctor would need to consider your individual risk before agreeing to perform the surgery.
Despite these risks and caveats, there are advantages to the procedure. One of these, Urbina said, “is helping make sure the patient feels involved and in control of their own birth experience.”
“Assisting a patient with the delivery of their own baby through c-section can be a very satisfying and memorable experience for someone who had initially envisioned a vaginal birth,” she said.
What does preparation look like?
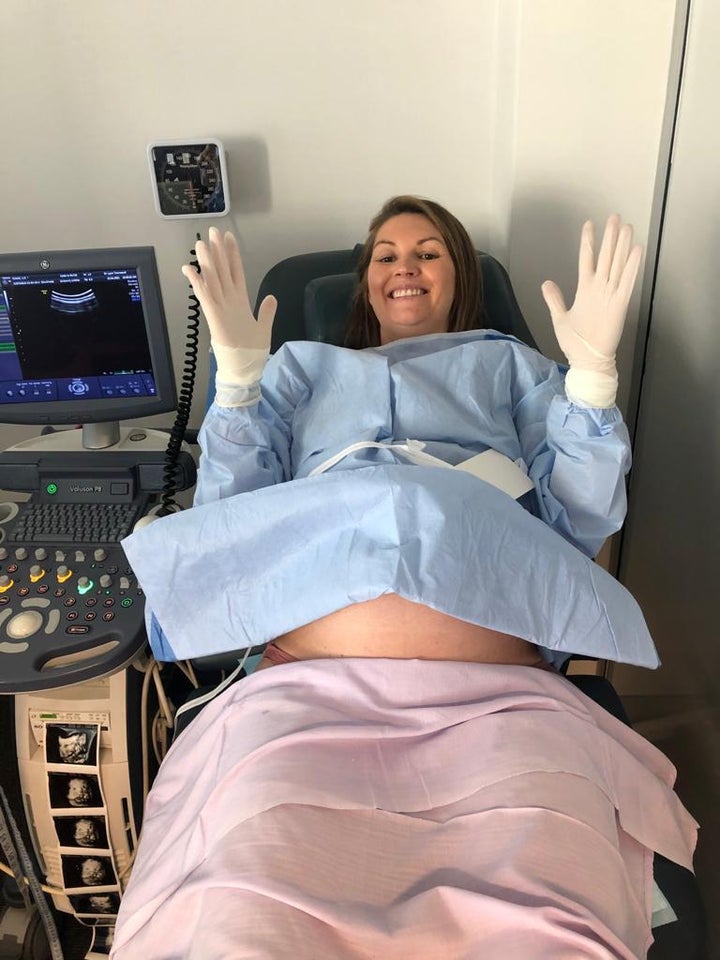
Evans says her doctor, Lynn Townsend, researched the procedure, considered the risks, and agreed to perform the surgery. She then went to bat for Evans with the hospital board, eventually securing their approval for the surgery to take place.
In the weeks preceding the birth, Evans said she and Townsend “discussed the logistics of the birth, and the importance of ensuring a sterile environment, and practiced the steps involved.”
These included having Evans perform a surgical hand-wash, and putting on a gown and sterile gloves while she was lying on her back.
“We rehearsed the timing of when I would reach down to deliver my baby from the abdomen, and the speed at which I would lift her to my chest to ensure Dr. Townsend had enough time to check that the cord had enough length,” Evans said.
In addition to discussing the usual risks of a caesarean, Townsend explained to Evans that if the baby was in distress, or if her labor began spontaneously, they would not be able to proceed with their plan.
Neither of those scenarios came to pass, and when the day of the planned c-section came, Evans experienced something very different from her previous births.
“Compared with my first cesarean section, it felt far less clinical, and I felt far more connected to the procedure as well as everyone else in the room. I was informed of every step along the way which really helped me to feel a part of the team,” she said.
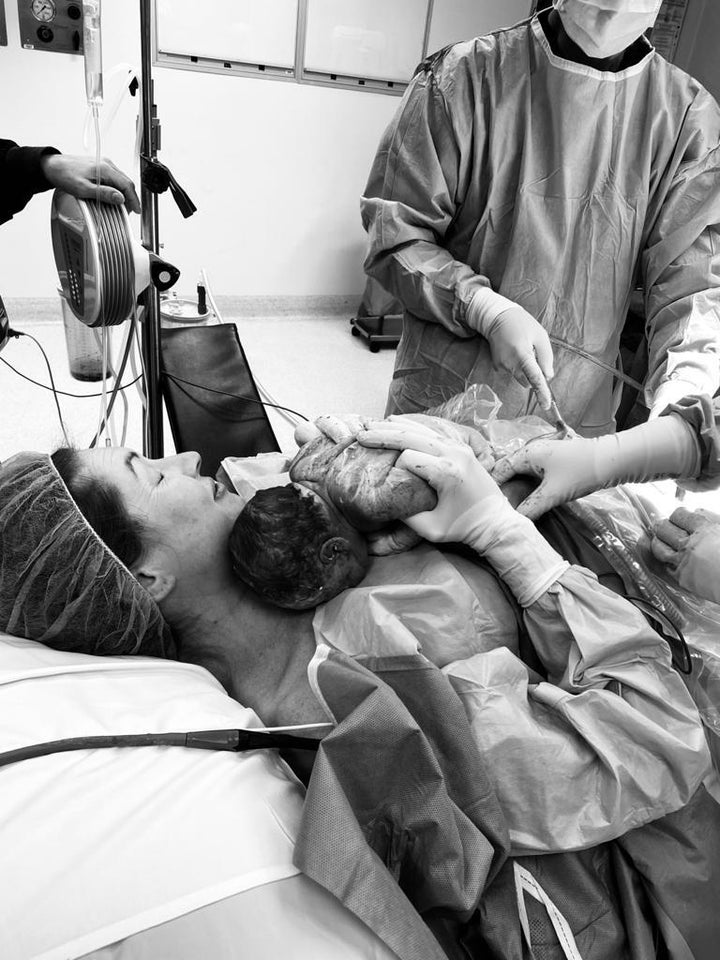
“I had watched every step of the surgery, so by the time it came to the point where I reached down to lift her out, I was so emotional with the build-up to this moment. She cried as soon as she came out of the uterus, and then, like magic, as soon as I placed her on to my chest over my beating heart she settled straight away,” Evans said.
Evans noted that the immediate skin-to-skin contact she described can also happen during a standard c-section, and that patients should ask their doctors about this possibility. More hospitals are now offering this option.
“It was one of the most incredible moments of my life and made it all worth it,” she said.