Undergoing female sterilisation may feel like the perfect solution for women who know they don’t want children, but a common method used by doctors in the UK has come under increasing scrutiny, both here and abroad.
A number of women who have had Essure implants fitted have suffered severe side effects, according to the BBC’s Victoria Derbyshire programme.
Essure implants work by blocking a woman’s fallopian tubes with scar tissue so sperm cannot pass, preventing her from falling pregnant.
The device has reportedly caused major health repercussions for a number of UK patients - with some saying they needed a hysterectomy (where the womb is removed completely) to remove the implant and others left in pain and feeling suicidal.
The BBC report follows growing concern over Essure in the US, where women have been sharing details of their side effects on the Facebook group Essure Problems. The US Food and Drug Administration (FDA) has also received more than 600 complaints about the device.
Now, the sale of Essure has been temporarily suspended in the EU.
It’s estimated that 750,000 women worldwide have opted for the irreversible procedure. So, if you’ve already been fitted with the implant, should you be concerned?
What is Essure?
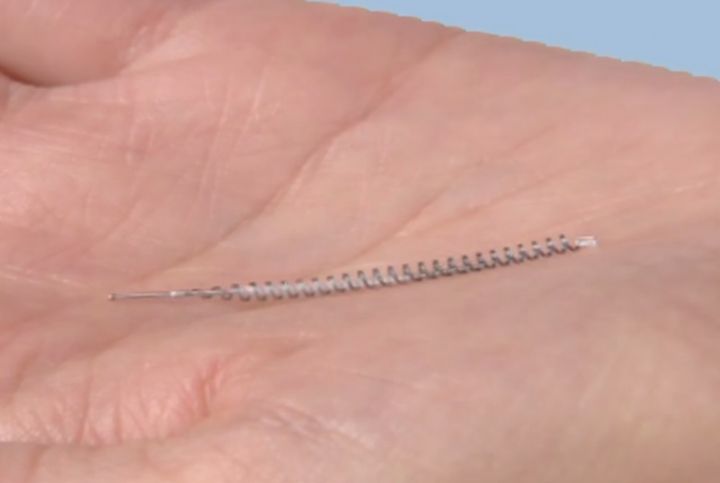
Essure is a permanent birth control procedure used to prevent pregnancy.
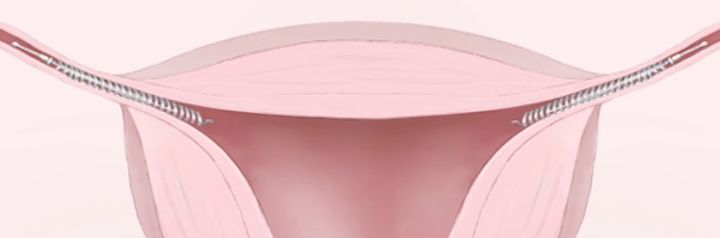
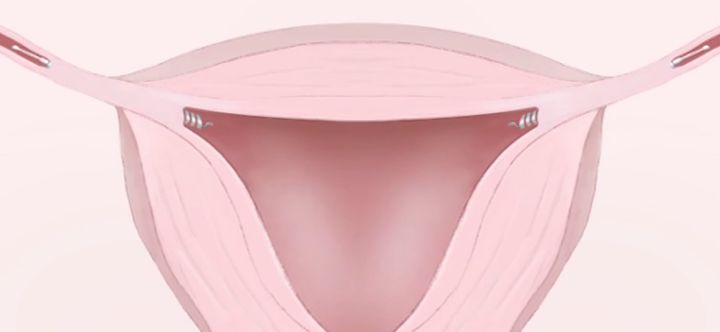
During the procedure, a metal insert is placed into each of the fallopian tubes - the tube that leads from the womb to the ovary, and the place where sperm meets the egg.
Over the next three months, a barrier of scar tissue forms around the inserts.
According to the BBC, the sale of Essure implants in the EU was temporarily suspended this month. In the meantime, the device’s manufacturer, Bayer, reportedly asked UK hospitals not to fit anyone with the implant.
What are the risks?
The product was approved by the FDA in 2002, yet a major study since then showed that this form of sterilisation - known as hysteroscopic sterilisation - has a “high risk” of complications.
The 2015 study, by Cornell University in New York, looked at more than 8,000 women in the US who were treated with hysteroscopic sterilisation and 44,278 with standard sterilisation (where fallopian tubes are tied or blocked via surgery).
According to the research, women who had hysteroscopic treatment were 10 times more likely to need a repeat operation within a year.
At the time a spokesperson for UK’s Medicines and Healthcare Products Regulatory Agency said the devices were “acceptably safe to use” but that “no medical device is complication-free when in clinical use”.
Commenting on the risks, Dr Helen Webberley, who runs the online healthcare service My Web Doctor, told HuffPost UK,: “As with all medical interventions and contraceptives, there are positive and negatives.
“For female sterilisation, techniques have improved over the years. Just 20 years ago, sterilisation would have meant an open operation, a surgical incision and a lengthy recovery period, modern techniques allow us to have the intervention without a general anaesthetic and with minimal recovery time.
“However, as with everything, some people will experience side effects such as pain, bleeding and infection.”
According to the Essure implant’s manufacturer, there are a handful of risks associated with the procedure itself including: inserts being placed incorrectly, part of the insert breaking off during placement and a risk of perforation of the uterus or fallopian tube.
Long-term risks include:
:: Pain (e.g. acute or persistent) of varying intensity and length of time may occur and continue following Essure placement.
:: Allergic reactions to the inserts.
:: Pregnancy.
:: Ectopic pregnancies - where the pregnancy occurs outside of the uterus.
:: If a patient has endometrial ablation, a procedure that removes the lining of the uterus to lighten or stop menstrual bleeding, after the Essure procedure, it is unknown if this will affect the blockage in the tubes, and effect their risk of pregnancy.
What are the benefits of Essure?
According to the NHS, research collected by NICE on hysteroscopic sterilisation found that the fallopian tubes were blocked after three months in 96% of sterilised women.
Unlike tubal occlusion - where fallopian tubes are tied - receiving an Essure implant is non-invasive and does not require general anaesthetic.
The implant is inserted via a narrow tube, through the vagina and the cervix.
“The Essure blocks the tube and thus prevents fertilisation,” Dr Webberley said.
“It is a very reliable and permanent form of contraception which is ideal for women who don’t want to use hormones and want a long-term solution.”
What does Essure say?
In a statement given to HuffPost UK, a spokesperson from Bayer, which makes Essure, denied the suspension of sales is due to health concerns.
“The temporary suspension of the Essure CE Mark [a mark given to products approved for sale in the EU] is not related to product safety or quality issues,” the spokesperson said.
CE marks are usually valid for a period of three years, after which they have to be renewed by the manufacturer. According to the spokesperson, not all queries about the product had been addressed prior to the expiration date, hence the temporary suspension.
They said the Notified Body National Standards Authority of Ireland (NSAI) decided not to renew the certificate until the queries had all been resolved. The spokesperson added that the benefits of Essure outweigh the risks.
“The dataset and clinical evidence provided to the NSAI demonstrate a favourable benefit-risk profile for Essure and compliance with the requirements of the Medical Device Directive,” they said.
“Our view on the favourable benefit-risk profile of Essure is supported by a number of health authorities, their safety assessment committees, and medical organisations, each concluding that, based on data from clinical, epidemiological and post market studies, literature, and pharmacovigilance, the benefit-risk ratio remains favourable.”
They added that “patient safety is Bayer’s top priority and Bayer UK stands behind Essure as an option for women who desire permanent birth control”.
What should women do if they’re concerned?
While the procedure cannot be reversed, it can be removed.
If a patient and their doctor decide that the inserts should be removed after placement due to experiencing side effects, surgery is necessary.
According to the Essure site: “This may include looking in the uterus (hysteroscopy), removal of the insert alone, removal of the insert with the fallopian tube, and/or, in complicated cases, removal of the uterus (hysterectomy).”
According to the NHS, Bayer now advises that women who’ve received the implant may opt for an ultrasound scan to check the placement of the implant after three months.
“If the coils of the implant are seen to be in the correct position, tubal occlusion can be assumed,” the website explains.
Dr Webberley added: “Anyone experiencing severe side effects should see their doctor, but for most women, it is safe, effective and trouble-free.
“Other long-acting methods [of contraception] include the implant, coil and male sterilisation.”
Dr Clare Morrison, from online doctor MedExpress, added: “I suggest that women immediately speak to a doctor after the recent news about Essure.
“Although sometimes these things can be overblown, it’s better to be safe than sorry.”
The Bayer spokesperson told HuffPost UK that “patients with Essure in place can continue to use the product and no action on their side is required as a result of this suspension”.
They added: “Bayer UK will continue to fully support patients with Essure in place along with healthcare professionals who have questions or concerns about the product or who need to report suspected adverse events, suspected quality defects or issues related to usability associated with Essure.”