Squeeze. Release. Pause.
Squeeze. Release. Pause.
20 times a minute.
1,200 times an hour.
28,800 times a day.
Listen for the hiss of air. Watch that little chest rise and fall.
Skip a round - just once, not even enough to feel the cramp come back in to your fingers - and your daughter will skip her next breath too.

A ventilator is a machine that breathes for people who have lost the ability to breathe on their own - under the influence of certain drugs in surgery, for instance, or if they have a serious illness. It's quite literally mechanical life support.
But in low-resource setting hospitals this kind of expensive equipment - let alone the electricity required to keep it switched on - is largely absent. In Malawi, 82% of district hospitals and 50% of central hospitals can't rely on consistent running water, let alone a functioning electrical generator.
What they can rely on are patients who will die if they don't get help breathing, family members who would do anything to keep them alive - and bag valve masks for manual ventilation.
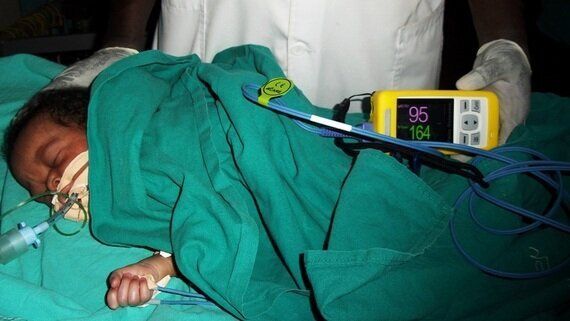
"How long has she been ventilating the baby?" asks the visiting doctor from the doorway of the children's ward at a hospital in Malawi.
She gestures to the woman in a bright cotton wrap crouched by a bed in the corner of the room, squeezing a clear plastic sphere. It's attached to a mask that covers a two-year-old's chapped lips. Each time the woman squeezes, she forces a gust of air into her daughter's lungs.
"Forty-eight hours," replies the nurse anaesthetist. "We hope to take her off today."
This is not an article about the superhuman strength of parental love, or its global universality. "I used to fear their deaths," author and journalist Caitlin Moran wrote about her daughters. "Until I realised it need never be a problem: on the trolley, on the way to the mortuary, I would put my hands into their ribs and take their hearts and swallow them, and give birth to them again, so that they never, ever end."
This is, instead, about anaesthesia: what it is, what else it is, and why it's a crisis when absent or unsafe.

"There is no surgery without anaesthesia," explains Dr William Banda, a medical anaesthetist in Malawi. "You can train 100 surgeons - but there will be no surgery."
This is both true and untrue: before the advent of anaesthesia for sedation and pain management, essential operations - say, an amputation to prevent deadly sepsis - still took place, but with several orderlies to pin the patient down.
Surgeons chose "slashing speed over precision...[as] the sound of patients thrashing and screaming filled operating rooms."
There is no surgery that qualifies as anything other than expedited torture without anaesthesia. There is no surgery without anaesthesia that anyone in the world should have to endure.
But this knack of putting people to sleep and waking them up again is just the beginning.
The anaesthesia provider is also responsible for resuscitation, for bringing the collapsed patient back from the brink, or ending that deafening silence of a baby delivered but still, still, still not crying.
They're in charge of ventilation, setting up systems that breathe for the patient until they can breathe for themselves again. They intubate - guiding a tube down the throat to allow for assisted breathing long term (akin to playing a life and death 'wire loop game' several times a day: take too long or go the wrong way and instead of making the wire buzz, your patient goes into cardiac arrest).
Pain management - that's also the anaesthesia provider's responsibility, from short term protection against the scalpel as it slides against your skin, to the long-term treatment of chronic pain sufferers.
This is a vast and risky portfolio, even in a high-resource setting hospital when anaesthesia providers are usually medical physicians with years of training (pharmacology, physiology, biochemistry, anatomy). They also have reliable access to drugs, the latest research, and a high tech equipment support system including at least eight different electronic monitors for the safety of each patient under anaesthesia.

In a low-resource setting with limited equipment (often inappropriate), critical drug and staff shortages and minimal access to continuing education - an estimated 95% of the anaesthesia workforce in Malawi is non-physician - it's a phenomenally daunting prospect.
And it's no wonder that anaesthesia becomes more dangerous. Risk of mortality soars, from around 1 in 200,000 in the US, to 1 in 133 in West Africa, with an impact on the family - and provider - that's devastating.
"It's traumatic," explains Dr Oyebola Adekola, a consultant anaesthetist in Nigeria. "When a patient dies who you know should have survived - you turn to your colleagues - you counsel each other...But still it's devastating. Often people need time off just to recover from the pain and trauma. And then you come back to work knowing nothing has changed."
Part of the problem is that too many people don't know it needs to.
Recently MBC TV, the main television station in Malawi, sent a camera crew to an anaesthesia training workshop at the central hospital. They saw first hand the skills that are required for safe anaesthetic care, the staff shortages and equipment struggles, and the best possible results in spite of this: a baby girl born safely by emergency Caesarean section.
The report was screened twice in 24 hours. What was the response?
"We didn't know, people say," explained the journalist about the operation - unthinkable without anaesthesia. "We didn't know you needed all this to survive."
This week, one of the biggest events in anaesthesia (it's not on your calendar?) takes place in New Orleans: the American Society of Anesthesiologists' annual conference.
More than 10,000 people from all across the US will gather for education sessions, networking, to try out the latest gadgets and find out what their Political Action Committee - the largest physician PAC in the country - is doing to advocate for anaesthesia's professional support and profile in Congress.
Lifebox Foundation will be there too, hosting a joint session with the ASA's Global Humanitarian Outreach (GHO) committee, and smaller sessions with experts in the field of global anaesthesia. We'll be advocating for support of low-resource setting providers, colleagues in anaesthesia who don't have the resources or the clout to advocate for themselves on this stage.
They're too busy in every corner of the hospital, running from surgery to delivery, an often undervalued dynamo in a fragmented healthcare system; stopping to check in on a mother who could tell you why more support for safer anaesthesia is necessary - if she wasn't so tired, crouched in the corner, still breathing for her baby.