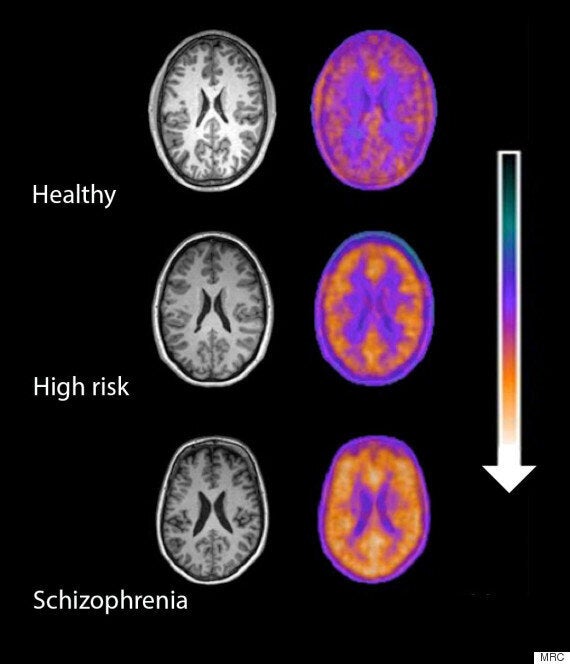
Scientists have discovered a way to diagnose early onset of schizophrenia, which would enable them to offer treatment to patients before symptoms become too severe.
Researchers found that immune cells are more active in the brains of people at risk of schizophrenia, as well as those already diagnosed with the disorder.
The study, which was published in the American Journal of Psychiatry, is the first to find that immune cells in the brain are linked to schizophrenia.
"Our findings are particularly exciting because it was previously unknown whether these cells become active before or after onset of the disease," said lead author Peter Bloomfield, from the Medical Research Council’s (MRC) Clinical Sciences Centre in London.
"Now we have shown this early involvement, mechanisms of the disease and new medications can hopefully be uncovered."
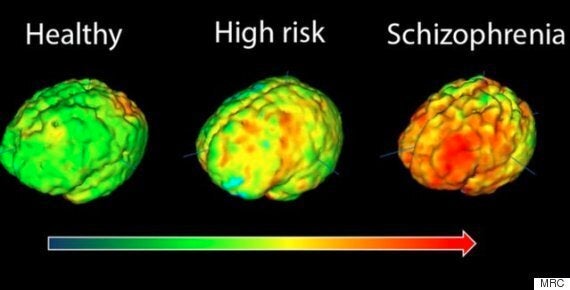
Researchers used positron emission tomography (PET) scans to measure levels of activity of immune cells in the brain.
These cells, known as microglia, respond to damage and infection in the brain, and are also responsible for rearranging the connections between brain cells so that they work as well as possible - a process known as pruning.
The scientists tested a group of 56 people, comprised of those who had already been diagnosed with schizophrenia, those at risk of the disease and those with no symptoms or risk of the disorder.
They found that activity levels of microglia in the brain increased according to the severity of symptoms in people with schizophrenia and that people with diagnosed schizophrenia had high levels of activity of these immune cells in their brain.
SEE ALSO:
This Is What Having Schizophrenia Is Really Like
People On Reddit Gave A Man The Best Advice On Mental Health
"Schizophrenia is a potentially devastating disorder and we desperately need new treatments to help sufferers, and ultimately to prevent it," said Dr Oliver Howes, head of the psychiatric imaging group at the MRC Clinical Sciences Centre.
"This is a promising study as it suggests that inflammation may lead to schizophrenia and other psychotic disorders.
"We now aim to test whether anti-inflammatory treatments can target these. This could lead to new treatments or even prevention of the disorders altogether."
Professor Hugh Perry, chair of the Neuroscience and Mental Health Board at the MRC, added: "Schizophrenia, like other mental health disorders, is a complex disease that we know is caused by an interplay of genetic, behavioural and other contributing factors.
"This study adds to a growing body of research that inflammation in the brain could be one of the factors contributing to a range of disorders – including Alzheimer’s, schizophrenia and depression - and with this new knowledge comes the hope of life-changing treatments."