Acne is a common skin condition, estimated to affect roughly 80% of people aged 11-30 in the UK. While many associate it with hormonal teens, in reality it can affect anyone at any age.
“It’s quite common to see patients presenting in their thirties who may have had clear skin in their teens,” explains Dr Justine Hextall, consultant dermatologist on behalf of The Harley Medical Group.
“Adult acne is increasing in prevalence, in women particularly.”
Anything from poor diet to pollution can contribute towards acne, but Dr Hextall says that stress and hormonal changes in adulthood are the most common triggers. And no, it’s not caused by having dirty skin or poor hygiene.
Here, we look at the different types of acne and what treatment is available.
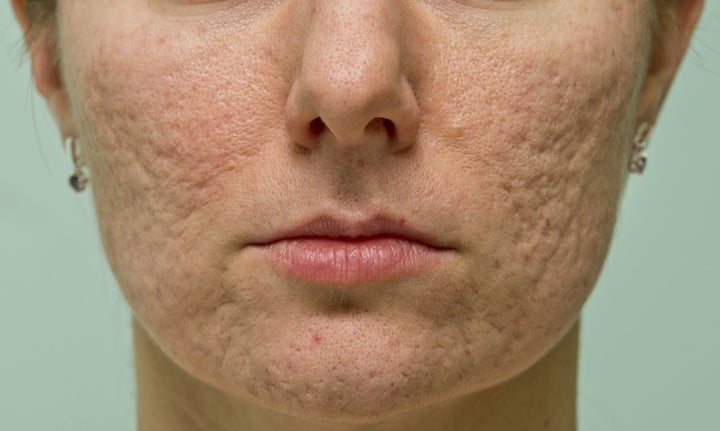
What is it?
“Acne vulgaris is a broad term which covers the occasional spot through to severe cystic acne,” Dr Hextall tells HuffPost UK. “As dermatologists, we look for black or whiteheads with the spots to help differentiate it, for example, from rosacea.”
The condition occurs when hair follicles in the skin become blocked and oil builds up.
“Sebaceous glands attached to hair follicles secrete an oil-based substance known as sebum,” explains Christine Bailey, a nutritionist on behalf of The Harley Medical Group.
“Sebum normally helps moisturise skin and keep it supple. However, when there is excess sebum produced, the follicle can become blocked. Sometimes, bacteria called Propionibacterium acnes that normally reside in the skin interact with the sebum trapped in a clogged follicle and lead to inflammation.
“So anything that clogs pores, leads to the rapid division of skin cells, and/or creates or worsens infection and inflammation will contribute to blemishes.”
There are six main types of spots caused by acne, these include: blackheads, whiteheads, papules (small, tender, red bumps), pustules (similar to papules but with a white tip in the centre), nodules (large, sometimes painful, hard lumps that build up beneath the surface of the skin) and cysts (large pus-filled lumps which can cause scarring).
Causes
Hormone imbalances and, in particular, excess production of testosterone can increase the amount of sebum in the skin.
“This is one of the reasons why acne is more common in adolescence,” explains Bailey. “It also explains why women may notice an outbreak just before their monthly period as levels of hormones fluctuate.”
Stress can also play a key role. “Cortisol, one of our stress hormones, interferes with blood sugar and causes the sebaceous glands to produce more sebum,” she continues.
“Stress can also lead to hormonal imbalances worsening ongoing symptoms.”
Unfortunately acne is also hereditary, so if your parents had acne it’s likely you’ll develop it too.
It is also thought that diet can play a part, however the NHS does note that research hasn’t found any foods that specifically cause the condition.
“There has been much debate about the role of diet and development of acne,” explains Bailey. “However a number of studies suggest certain types of food could worsen or improve acne. So if you are undergoing treatments for your skin, maximise the benefits by making some changes to your diet.”
She explains that drinking more water can help flush out toxins and replenish water in the cells, which keeps your skin looking “plump and fresh-looking”.
It’s also important to be conscious of foods high in carbohydrates, the nutritionist recommends.
“In particular quick-releasing carbs such as fruit juices, cakes, alcohol, biscuits, sweet foods, refined white grains and processed foods,” she explains, “as these lead to a sudden rise in blood sugar and the production of excess insulin.”
This spike in blood sugar can result in the production of certain growth hormones like IGF-1, “which can stimulate sebaceous glands, promote more insulin in the body and alter skin cell production”.
Bailey recommends trying wholegrain rice or quinoa or starchy vegetables such as sweet potato, carrots and beetroot, instead.
She also advices to eat more greens and whole foods, try fermented foods naturally rich in beneficial bacteria (such as yoghurt or kimchi) and possibly cut out dairy.
“For some people dairy produce is known to aggravate acne,” she explains. “Milk is a direct source of hormones and a number of growth factors including IGF-1.
“Simply switching to a milk alternative such as almond or coconut may lead to improvements.”
Treatment
Treatment for acne depends on how severe it is. For mild cases - where you have a few blackheads, whiteheads or spots - you should be able to treat them with over-the-counter gels that contain benzoyl peroxide, the NHS suggests.
A good skin care routine is also important.
Dr Anjali Mahto, consultant dermatologist and British Skin Foundation spokesperson, says: “Ensure that cosmetics and sun creams are suitable for acne-prone skin and preferably ‘non-comedogenic’ (such as products that will not block pores).”
Dr Justine Hextall explains it’s also imperative to try a gentle cleanser, as “you need your skin barrier to be as healthy as possible so that it can retain vital moisturiser”.
“As a rule of thumb, if your skin feels tight after washing it is likely the cleanser you are using has disrupted your skin barrier,” she says.
“Skin should feel calm and hydrated after washing. If you are reaching immediately for your moisturiser you may want to consider a more gentle cleanser.”
It can take several months of treatment before acne symptoms improve.
For severe cases, medication might be prescribed such as: topical retinoids, topical antibiotics, azelaic acid, antibiotic tablets, the combined oral contraceptive pill (for women only) and isotretinoin tablets.
Topical treatments contain agents that unblock follicles and reduce inflammation.
Antibiotics, both topical and systemic, are used but resistance is increasing. One study found that four in five teenagers with acne showed some resistance to antibiotics.
For more severe acne, especially if the skin is scarring, drugs like Roaccutane may be considered, however it’s worth noting that it can cause side effects such as dry skin, headaches, depression, hair loss and even psychotic disorders or suicidal feelings.
The drug recently made headlines after campaigners from the Adverse Psychiatric Reactions Information Link said that too many young people are being put on them and not monitored, which could be particularly dangerous for those who experience side effects related to mental health.
In 2016, nearly 49,000 Roaccutane prescriptions were dispensed in England compared to 37,000 in 2014, according to NHS Digital data.
In response to worries over increased prevalence of the drug, The British Association of Dermatologists said that as long as safety recommendations are adhered to, this should not be a cause for concern.
Roaccutane’s manufacturer Roche told the BBC: “Information provided with isotretinoin [Roaccutane] carries a warning that some patients may experience mood changes, including an increase in depression.”
Other treatments for acne include dermabrasion (which involves removing the top layer of skin through either lasers or a wire brush), chemical peels and laser treatment which can help reduce post-acne redness and scarring.
Dr Anjali Mahto concludes: “Do not suffer in silence. Seek support from a healthcare professional, ideally a qualified dermatologist. These are the only people properly trained in managing skin problems.”