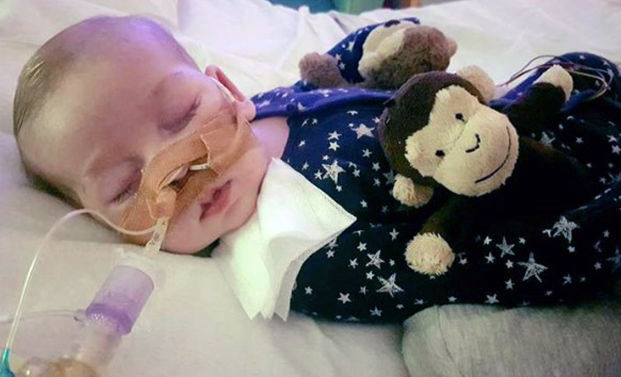
Terminally-ill baby Charlie Gard is unlikely to be allowed to spend his final days at home with his parents, a High Court judge has said.
Mr Justice Francis said he will make a decision about where the 11-month-old boy should spend the remainder of his life, on Wednesday.
Doctors caring for Charlie at Great Ormond Street Hospital in London said they want to fulfil the “last desire” of his parents, Chris Gard and Connie Yates.
But they said there are practical difficulties in providing the intensive care Charlie needs outside a hospital, including that the ventilator Charlie needs won’t fit through the front door of the property his parents want to take him.
and the judge said the chances of him being able to spend his final days at home are “small”.
Charlie’s parents have become embroiled in a fight with doctors over the circumstances of his death, a day after abandoning attempts to persuade a judge to let him travel to America for experimental treatment.
Mr Justice Francis presided over the dispute at a hearing in the Family Division of the High Court in London on Tuesday, and the hearing is scheduled to resume at 2pm on Wednesday.
As Charlie’s mother returned to the High Court on Tuesday, the judge said the dispute cried out for settlement. But he said if a solution could not be agreed he would decide on Wednesday.

Barrister Grant Armstrong, who leads the couple’s legal team, suggested to Mr Justice Francis that hospital bosses were placing obstacles in Charlie’s parents’ way.
“The parents wish for a few days of tranquillity outside of a hospital setting,” Mr Armstrong said.
“The parents had hoped that Great Ormond Street would work with them.”
He added: “The parents’ primary position is that Charlie’s final days of palliative care ... should take place at the family home.”
Mr Armstrong said Great Ormond Street doctors thought that moving Charlie to a hospice was the best plan.
But he said the couple felt there was a “brutality” to taking Charlie to a hospice.
He told the judge: “We struggle with the difficulties which the hospital is placing in the way.”
Barrister Katie Gollop QC, who leads Great Ormond Street’s legal team, said staff were not creating “obstacles”.
She said nothing could be further from the truth – she said staff had “moved heaven and earth” for Charlie.
But she said the couple’s needs had to be balanced against Charlie’s best interests.
“The care plan must be safe, it must spare Charlie all pain and protect his dignity,” said Ms Gollop.
“At the same time, the plan must honour his parents’ wishes about two matters in particular, namely the time and place of his passing.”
She said finalising an end-of-life care plan was the “most delicate and difficult task”.
“Charlie’s parents want him to be with them and ventilated at home for several days before receiving palliative care,” she said.
“Above all, Great Ormond Street wants to fulfil that last wish.”
She added: “The key obstacle, and one which the hospital cannot see a way around, is the reality of invasive ventilation that Charlie requires.”
Ms Gollop said such invasive ventilation was only provided in a hospital setting.
She said Great Ormond Street administrators had been unable to find a specialist anywhere in the country prepared to oversee such a level of intensive care at Charlie’s home.
“Those resources cannot be provided by Great Ormond Street to Charlie at his parents’ home,” she said.
“Great Ormond Street is aware that there are other practical problems, one being that the ventilator does not fit through the front door.”
She added: “Charlie is a child who requires highly specialised treatment. His care cannot be simplified.
“It is in Charlie’s best interests, and everybody’s, that the risk of a precipitate, distressing or disordered death is removed, so that he may be reassured of a peaceful and dignified passing.”
Ms Gollop said Great Ormond Street had found an “excellent hospice” which would give Charlie and his parents the space, privacy and protection they needed.
