
Annie Rose Barber, 34, was diagnosed with severe stage 4 endometriosis three years ago, but has had it for decades. She’s had two surgeries and is waiting for her third. Here, she tells her story.
When I was a teenager, I felt like I was dying during my periods. Or being stabbed in the stomach repeatedly. They were so incredibly painful, they’d just floor me. Drugs didn’t touch the surface – I’d be out of action the whole week.
I’d always had really painful periods – they’d kept me bed-bound ever since they started when I was 11 – so to soften the pain, I was put on the pill aged 13. But I think that just masked the symptoms. Throughout my childhood, I was always quite sick, and in my teens and early 20s it seemed worse. At 28 – well, that’s where the bigger problems started.
I had come off the pill because I knew, at the back of my mind, something was wrong. I wanted to tackle the problem before having children – and that’s when everything changed.
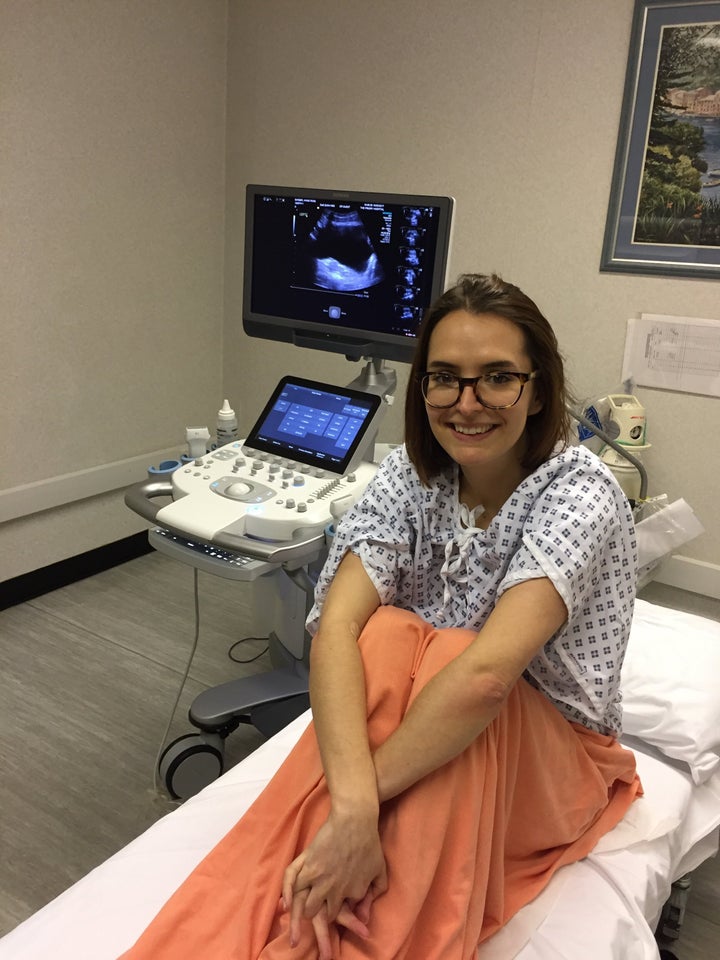
The pain was unbearable – and it wasn’t just during my periods that it was bad. I felt ill throughout the month, which made it hard for doctors to diagnose me. I’d be given painkillers that didn’t do anything, and the constant back and forth with no diagnosis made me doubt myself a lot. I took it to heart and thought I was weak. “It’s just part of being a woman,” they’d say. “It’s period pain, it’s nothing to worry about.” I was made to feel like it was all in my head, like I was a hypochondriac.
Doctors took blood tests, and they came back normal. I was healthy, I was told. Maybe it was stress-related, they said. I was fobbed off time and time again.
It was around this time I learned about endometriosis. I’d never heard of it before, but my husband had done a lot of research because he was worried – and came across it. My symptoms matched up completely.
[Read More: Endometriosis Symptoms And Treatment Explained]
By this point, I had quit my job working for an international organisation, because it involved a lot of travelling. I left without a new job to go to – I just couldn’t handle it. I was too sick to work. I had changed my diet and tried drastic things to stop the pain, but nothing made a difference.
That was until I found a doctor who listened, which took three years. Within 10 minutes, she had referred me to a gynaecologist. That person immediately did an internal examination and could feel a nodule, so suggested an MRI scan. It revealed a suspected diagnosis of severe stage 4 endometriosis. You could see it – lumps all over my pelvis. My womb was stuck to my bowel, my right ovary stuck to the right of my pelvis. It looked terrifying.
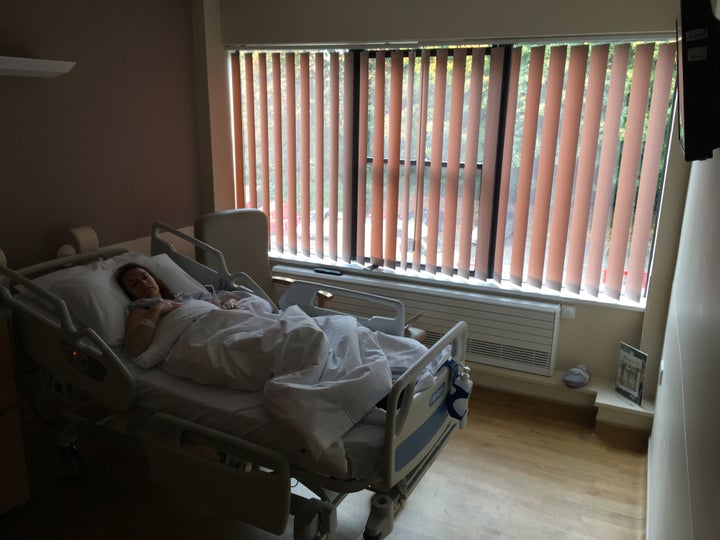
I was told I’d be referred to a general gynaecologist for surgery, but I was desperate for an endometriosis specialist because I’d read things could get missed if medical staff weren’t clued up on it. I wouldn’t back down. I had to fight my local doctor surgery, then the clinical commissioning group and go through an appeal to get the referral to a specialist. It took nine months, but I won.
It was a stressful time, of course. I was already sick, so having to fight to get surgery was frustrating. When I finally had my laparoscopy, the specialist found it was a lot worse than initial scans showed. It wasn’t just in my pelvis, but on the outside of it, on my diaphragm and near the back of my liver, which he said was rare. It was wrapped around my bladder and bowel, all over my womb and both ovaries.
He couldn’t operate there and then – he needed a bowel surgeon and a urologist present because of how severe my case was. The second surgery was another five month wait. I had what’s called excision surgery, which was invasive, but it cuts out the disease at the root. And it did help, to an extent.
It’s been two years since that operation. But because it went undiagnosed for decades, it caused so much damage within my pelvis and caused adhesions. My organs are still stuck together, my bowel still stuck to my uterus. I’d say at its worse before: if the pain was a 10/10 back then, now it’ll hit about a seven or eight.
I’ve been able to get back a lot of my life, sure, but I’m by no means cured. Life is more bearable. I’m working again part-time, but I still have to really take care of myself.

And there are, of course, long-term consequences from those lost years. My fertility, my career. My partner and I have been trying for three years for a baby and had no success. We’ve been offered IVF loads, but I turned it down because it can make endometriosis worse, and that’s not a risk I am willing to take. I’ve found when you talk to doctors about endometriosis, the only thing they care about seems to be fertility. Not pain. Not quality of life. Thankfully, my surgeon who diagnosed me was concerned about those things, too, so I felt more comfortable discussing my fertility with him. He said it’d be harder, but he managed my surgery without damaging my ovaries too much.
Now, I’m having to go back for a third surgery, because scans have shown it’s come back in my bowel area. They’ll do the same thing, cut it out at the root, but I’m not sure how long it’ll last. I’m considering having a hysterectomy for this surgery, as it’s a cure for adenomyosis, which is a sister condition contained in the womb which I have. It’s a drastic and really hard decision, but the pain is so bad that it has to be an option. Because of this, my partner and I have started the adoption process.
We really need to see change in the medical field. In the UK, there’s only a handful of specialists in endometriosis who really know how to identify and treat the disease as well as they can. We can’t blame doctors, because what they’re taught in medical school is so outdated. Endometriosis affects one in 10 women, 176 million women worldwide. And it’s a complicated disease, so we need to invest and put more research into it. We can’t brush over it anymore.
People don’t talk about it, and I think that links to the fact no one really talks about periods, either. It’s seen as a taboo, so women are shy about coming forward with issues. We need to take women’s pain more seriously. Something’s got to change. It just has to.
For information and support on endometriosis, visit national charity Endometriosis UK.