
Many factors ― including scare tactics in school, agenda-pushing politics and misrepresentations in popular culture ― have created a massive stigma around HIV and AIDS. This impacts everything we think we know about the condition, from who we believe can contract HIV, what an HIV infection looks like and how the virus spreads.
Experts say that incorrect stereotypes about HIV have led to underdiagnosis and undertreatment for many folks who are either afraid to get tested, don’t think they need prevention or don’t think they can get the virus.
In other words, the stigma is dangerous. And, unfortunately, since these ideas are so ingrained in our culture, it’s also hard to break. But education is one way to help dispel the misinformation that exists so it can be easier for people to talk about HIV and get tested and treated for it.
Experts say there are a few pervasive myths, in particular, that contribute to the overall stigma for the virus. Below, they break them down and why they’re so wrong:
Myth 1: HIV is a death sentence.
Dr. Toyin Nwafor, an infectious diseases physician and the senior medical director of HIV Prevention at ViiV Healthcare, said that people often believe that HIV means an inevitable death, which is not only inaccurate but can impact people’s treatment choices, too. This thought “prevents people from getting tested or engaging in care,” Nwafor said.
HIV is not a death sentence, and experts can’t stress this enough.
“[HIV has] really become a chronic disease in many ways akin to high blood pressure or diabetes,” said Dr. Oni Blackstock, the founder and executive director of Health Justice. “I would say the one difference is the level of stigma that is associated with it.”
“Because once people are diagnosed and can get on effective therapy, the virus suppresses and their immune system recovers,” Nwafor said. “So, people living with HIV have long, healthy, productive lives.”
Myth 2: HIV is no longer an issue.
HIV does not get the same attention from the media and the public that it did decades ago, which can lead people to assume the virus is no longer a threat. But that’s also wrong.
In the United States, 36,000 people were diagnosed with HIV in 2021, Nwafor said. “So that emphasises the need to continue to increase the awareness around HIV [and] the need for routine testing.”
Additionally, certain groups are being disproportionately infected, which doubly underscores that HIV still is around.
“Of all those new diagnoses, about 40% of them are in Black Americans, about 30% in Latino and about 25% in white and 5% in multiracial people,” Nwafor noted. “And why that’s important is because Black Americans only make up 12% of the population, yet they had 40% of the new diagnosis. Latino [people make up] about 18% of the U.S. population, yet they had about 30% of HIV infections.”
Myth 3: Once someone is diagnosed with HIV, they’ll give it to all of their sexual partners.
“When [someone is] virally suppressed on treatment and becomes undetectable and stays undetectable on treatment, they no longer can transmit that virus sexually to their sexual partner,” according to Nwafor.
Many people are completely unaware of this — most people think that if an infection happens, they’ll always spread the virus to their partners.
“Something we call U=U, undetectable equals un-transmittable. That is one of the biggest things that has been so impactful in engaging people in HIV testing, because the reason most people are scared of getting tested or the stigma around testing is, ‘What happens if I have a positive result?’” Nwafor added.
Folks should recognise that through treatment, they can become undetectable. The fact that you’re “no longer able to transmit the virus sexually to your partners is a very empowering message,” Nwafor said.

Myth 4: Only certain people get HIV.
While HIV does disproportionately impact gay, bisexual and other men who have sex with men — 70% of new infections in the U.S. in 2021 were in people in these groups — it can also infect others.
But most people don’t think this way. It’s often believed that only certain people are affected or can be affected by HIV, Blackstock said. This is due to the positioning of HIV from the start of the epidemic.
“From the very beginning, there were ... the 4Hs ... and then sort of this idea that it was mainly a ‘gay disease,’” Blackstock said. (The 4Hs refers to the original designation of the four “at-risk” groups by the Centres for Disease Control and Prevention — homosexuals, heroin addicts, haemophiliacs and Haitians — which has since been criticised.)
The idea that it was a “gay disease” along with the 4Hs designation minimised the impact of HIV on other groups. “There was less attention to Black trans women and Black cisgender women and primarily focused initially on white gay men,” Blackstock said.
This myth is still around today. Blackstock said her cisgender women patients are frequently shocked when they learn of their diagnosis. “They didn’t have what they thought were the risk factors that were associated with HIV.”
“There are certain groups that are disproportionately impacted, but that doesn’t mean that because you aren’t part of one of those groups that you are somehow immune or protected from HIV,” Blackstock added.
Myth 5: You can get HIV from kissing and touching.
There are misconceptions regarding how HIV spreads, too. The idea that you can get HIV from casual contact like hugging, kissing or sharing utensils is unequivocally false, Nwafor stressed. “That is such a big myth.”
HIV is transmitted through blood, semen, pre-seminal fluid, vaginal fluids and breast milk and rectal fluids. “But you cannot get that from breathing the same air as someone, touching the toilet seat, sharing the same plates or utensils,” Blackstock said.
This myth is a direct result of misinformation and scare tactics. “There’s a lot of ignorance around it, and myths and stigma. So that has to do with just continuing to educate the public,” Nwafor said.
Myth 6: PrEP is only for men.
PrEP, or Pre-Exposure Prophylaxis, is a medication that reduces your risk of acquiring HIV. And there’s a pervasive myth that the medication is only for men.
“There are PrEP options for everyone who would benefit from prevention, and that includes cisgender women, transgender women, men who have sex with men and men who have sex with women. So, PrEP is for cisgender women and trans women in addition to cisgender men and transgender men,” Nwafor said.
It’s a valuable way to stay infection-free. According to the CDC, when taken as prescribed, PrEP reduces your risk of contracting HIV sexually by 99% and reduces your risk of contracting HIV through injection drug use by 74%.
Myth 7: HIV tests are expensive and take forever for results.
Nwafor said many folks believe that HIV tests are costly and that it takes a long time to get results. While this may have been the case at one time, it is not the reality now.
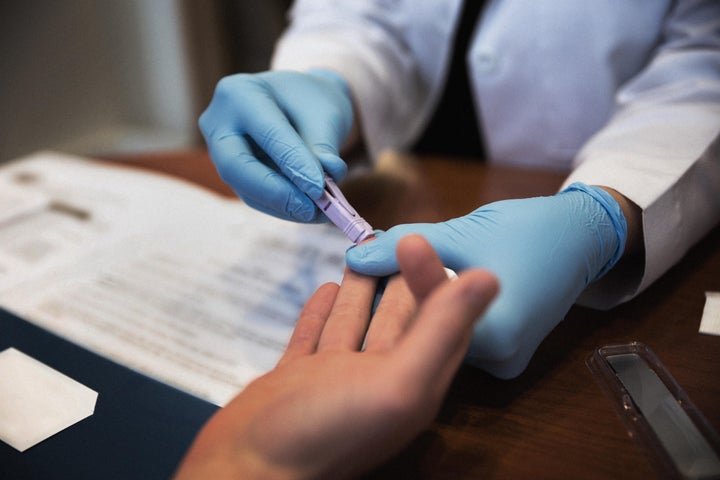
“Technology has improved so much, and we can get results rapidly — in 30 minutes or less. There’s home testing, there’s testing in different health care settings,” Nwafor said. “And in every state and city in the country, there are places where we can get a free HIV test.”
You can use the CDC’s Get Tested tool to find free HIV and STD testing in your area.
Myth 8: There’s a cure for HIV.
While there are effective treatments that can prevent HIV infections and lower people’s viral load to undetectable levels, there is not yet a cure.
Some people incorrectly believe that rich people have access to cures that the average person does not, Blackstock said. While money certainly can ensure treatments and a healthy lifestyle, there is not currently a cure for HIV.
Blackstock said she’s seen this belief regarding Magic Johnson. “The fact that he had access to really effective treatment and so he’s been able to, again, live a really long, healthy life, I think that confused a lot of people,” she said. “I think people are like, ‘Oh, Magic Johnson’s cured,’ so there’s some strange beliefs that are out there.”
Blackstock added that researchers are working on a potential cure — it just hasn’t been achieved yet.
Certain thought patterns allow these myths to exist — but there are ways to help end the stigma.
HIV myths are so pervasive because most people are not properly educated about HIV. For many people, the only education they did get is the message that HIV is scary, Nwafor explained. So as a defense mechanism, people isolate themselves from the realities of the virus.
By isolating themselves, HIV doesn’t have to become personal, Nwafor added. “By saying it’s only certain people, it’s gonna be a death sentence ... it becomes an ‘other’ and when that happens, then people don’t ever think that it’s something that could impact them.” But that isn’t reality.
There are more layers to this, too.
“One is that the groups that are most impacted [by HIV] are groups like men who have sex with men, trans women, people who inject drugs ― and these are all groups that have been heavily stigmatised by society,” Blackstock said.
The behaviours that can lead to an HIV infection — sexual activity, drug use — are heavily stigmatised by society as well, Blackstock added.
“So, I think because of the groups that have been impacted and the behaviours that are associated with these groups ... because they’re also stigmatised, that has sort of led people to generate these different myths and ... false beliefs about HIV,” Blackstock noted.
If it feels like an almost pile-on of stigma, you aren’t wrong. Much needs to be done to help end these dangerous ideas, but experts say there are changes that society can make to help.
“Talking more openly about HIV helps to normalise the topic,” Blackstock said. “If someone hears someone say something that is incorrect about HIV, really stepping in and interrupting and saying, ‘Hey, you know, that’s actually not true.’”
Plus, studies show that being mindful of how you talk about HIV and people living with HIV can be important, too, she said.
Additionally, Blackstock (who is also a CDC clinical ambassador) said the health agency has a helpful resource called Let’s Stop HIV Together, which aims to educate people about HIV, encourage testing and treatment and stop the harmful stigma and misinformation.
“We can each play a role ... to stop the stigma by being thoughtful about our language and how we speak up against HIV stigma,” Blackstock said.