They say that 40 is ‘the new 30’ – but there’s no better reminder you’re only the ‘new’ 30, and not the actual 30, than an NHS Health Check invitation landing on your doormat. It doesn’t help that this free service, offered to everyone from 40-74, has been nicknamed the ‘midlife MOT’.
But is it anything to worry about – and what can we do to make sure we ‘pass the test’ with flying colours?

What is the NHS Health Check?
Much like a car MOT, the ‘midlife MOT’ is to check that some of your body’s most important systems are running smoothly – and detect any potential problems before they have damaging or fatal consequences.
“It’s essentially a cardiovascular risk assessment of circulatory and heart problems – in other words, heart attacks and strokes,” Dr. Rob Hicks explains to HuffPost Lifestyle.
What does it involve?
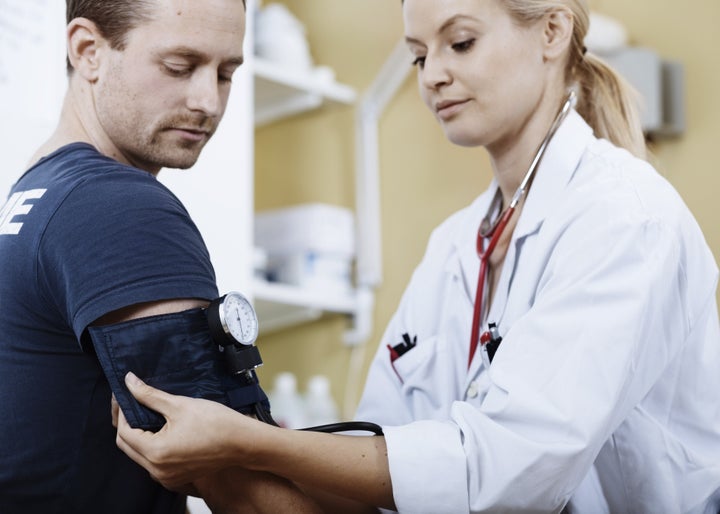
You can expect to be weighed, have your BMI checked, your blood pressure taken, a blood test taken for diabetes and cholesterol, and to be asked a few lifestyle related questions – like whether you smoke, how much alcohol you drink, and how active you are.
“The reason the [Health Check] tests for blood pressure, cholesterol and diabetes, is that when blood pressure and cholesterol are high and not controlled – and when diabetes is not treated correctly – they all increase the risk of cardiovascular problems,” explains Dr Hicks.
What’s the point of the check?
“The idea is to help identify whether patients are at risk of a heart attack, stroke or diabetes,” he adds. “If these risks are identified, the doctor will offer advice on how you can reduce or eliminate the risks. But even if you’re not identified as someone at risk, this is a good opportunity to say, ‘at the moment you’re not at risk but these are the steps you can take in order to keep yourself in that situation.’”
How can we pass our MOT with flying colours?
Barely a week goes by without some new study unveiling a new way to cut heart disease risk, lower blood pressure or reduce cholesterol levels. But while it might be nice to think that you can maintain a healthy ticker on a diet of red wine, chocolate and sex – it really all comes down to a few simple, common sense lifestyle choices.
And the steps for managing blood pressure, cholesterol and BMI are pretty much the same: “If you achieve an ideal weight, you reduce your risk of diabetes and there’s a good chance you will improve the balance of fats in your body, therefore reducing your risk of high cholesterol,” says Dr Hicks.
Eat right
From blueberries and beetroot to goji berries and garlic – the list of so-called ‘superfoods’ that can apparently cut your risk of heart disease is seemingly never-ending. But the NHS is quick to point out that superfood is simply a marketing term – and most superfood studies test extracts in much greater concentrations than you would find naturally in food.
In other words, there is no singular miracle food for keeping heart disease at bay: it’s all about a healthy, balanced diet. According to Dr Hicks, that’s one that includes “five portions of fruit and veg, lots of fibre, not too much saturated fat and not too much sugar.”
But while saturated fat should be avoided, the NHS advises that unsaturated fat can actually reduce cholesterol. Find this in olive, sunflower, corn, rapeseed, vegetable, nut and seed oils – as well as vegetable spreads, avocado, oily fish and nuts.
Heart UK suggests fruit and vegetables are also a valuable source of cholesterol lowering soluble fibres and recommends trying to include at least one pulse (beans, peas, lentils) everyday. Other rich sources include sweet potato, aubergine, broccoli, apples, strawberry and prunes.

Move more
Doing 150 minutes of moderate aerobic activity every week can improve your cholesterol levels, according to the NHS. How do you know it’s moderate aerobic activity? When you can still talk, but you can’t sing the words to a song, they explain.
Of course, the major stumbling block for many of us is finding the time to fit exercise in around our busy schedules. But Dr Hicks says we need to stop groaning that we can’t find 30 minutes in the day to go to the gym and be more creative about integrating exercise into our day.
“I know I spend an awful lot of my time sitting down so now I stand and use my laptop while I’m standing. I even jog on the spot while I’m editing copy so I’m being active while getting the work done,” he explains.
And this can even be extended to meetings: “Tomorrow I have a meeting, which is supposed to be in a café by the river but instead we’ll grab a coffee and go for a walk along the river. I even went to one meeting where instead of sitting around this big desk, we just all got up and walked around it while we talked.”
Half the battle is making exercise a habit – because once it becomes a habit you’re less likely to make excuses. Here are some tips on how to get back on the exercise wagon.

Banish your bad habits
If you’re a smoker, kicking the habit is the single best action you can taketo protect the health of your heart, according to the British Heart Foundation. Smokers are almost twice as likely to have a heart attack as those who have never stopped – but the good news is that the risk to your heart health decreases significantly soon after you stop.
Drinking is a more complex issue because it’s okay to enjoy a drink every now again but many of us are oblivious to the amount we’re really drinking. And too much alcohol can also raise blood pressure, and contribute to weight gain and obesity.
“What we’ve often said in medicine is that when doctors ask you how much you drink, the doctor doubles it and records it in the notes. It’s only when people start logging their intake they realise just how much they drink,” says Dr Hicks.
New guidance published in January lowered the limit for men to 14 units a week (the same as women). But a report from Drinkaware revealed that men between the ages of 45 and 64 were drinking an average of 37 units a week and don’t believe their health is at risk, while government statistics have shown that people in this age group are the most likely to be admitted to hospital with alcohol-related disease.
If you do stick to the 14 units a week, Dr Hicks warns that you shouldn’t be saving it all up for a once-weekly blowout: “If you’re going to have 14 units a week, you should consume that over at least three days and have a couple of days in the week that are alcohol free.”