The majority of costly “add-on” treatments offered by UK fertility clinics are of “no benefit” when it comes to improving the chances of having a baby, BBC Panorama has revealed.
Inside Britain’s Fertility Business found that 26 out of 27 of the so-called treatments have no solid scientific evidence they enhance standard fertility care like IVF and some may even be harmful.
“Add-on” treatments include things like additional procedures, additional drugs or devices to house an embryo. They can cost anywhere between £100 and £3000 on top of standard fertility care.
The research, commissioned by the BBC, forms part of a Panorama investigation to be broadcast on Monday.
It was conducted by Oxford University’s Centre for Evidence Based Medicine and will be published in the medical journal, The BMJ.
Last year, Panorama approached Oxford University to find out how good the evidence is behind these “add-on” treatments. They are world experts in assessing medical evidence. Their research has taken almost a year to complete.
The Oxford researchers began by identifying 27 “add-on” treatments. They then searched for every claim made in connection with these treatments on UK fertility clinic websites. They found little evidence quoted on the clinics’ websites substantiating the claims they made.

Professor Carl Heneghan, Director of Oxford University’s Centre for Evidence Based Medicine, told Panorama: “It was one of the worst examples I’ve ever seen in healthcare.
“The first thing you would expect to happen is that anything that makes a claim for an intervention would be backed up by some evidence.”
Due to the lack of supporting evidence on websites, the researchers went looking for what evidence there is about these treatments. They read hundreds of scientific papers, looking for high quality evidence that “add-on” treatments could improve the chances of having a baby.
They found that 26 of the 27 treatments did not have high quality evidence that they could improve the chances of having a baby with standard fertility care.
Only one treatment – called endometrial scratch - had even moderate quality evidence that shows an increase in the chances of a baby with standard fertility care like IVF. There are still question marks over the evidence for that treatment. Due to its limitations the researchers noted there is currently a randomised trial ongoing in the UK to determine its effectiveness.
Professor Heneghan added: “Some of these treatments are of no benefit to you whatsoever and some of them are harmful… I can’t understand how this has been allowed to happen in the UK.”
At the heart of this debate is whether patients should be sold “add-on” treatments that cost large sums of money when there is no good scientific evidence that they increase the likelihood of having a baby.
Adam Balen, chair of the British Fertility Society, told the show: “Provided we’re not causing harm, I don’t think that there’s any problem with giving patients information....discussing that we don’t know yet but there is an evidence base developing.”
Panorama also found evidence that, when marketing one “add-on” treatment, not all clinics were telling patients everything they needed to know to make a properly informed decision.
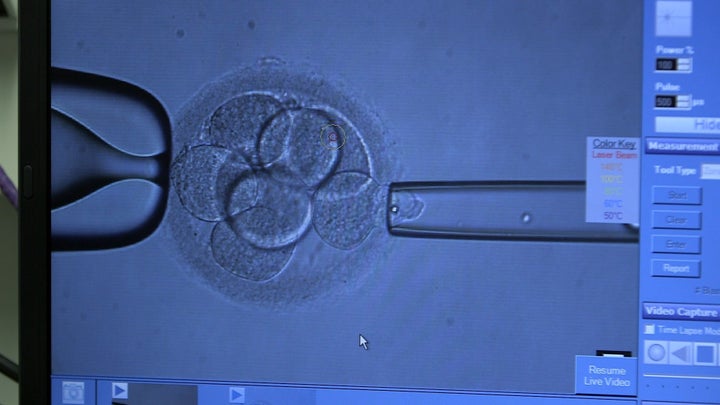
The “add-on” in question is called pre-implantation genetic screening, otherwise known as PGS. It screens embryos for abnormalities that might stop them developing further.
An initial version of the screening process was offered on the basis of small studies. Then a randomised trial in 2007 was the first to discover that this first version may have actually reduced the chances of having a baby.
Many clinics sell new, more accurate versions of the screening process, in some cases for around £3000.
Initial research looks promising and there are randomised trials underway. But as yet there is no high quality evidence from robust trials that these new versions improve your chances of a baby.
An undercover Panorama reporter went to a fertility fair in London last year and spoke to staff from 18 British and foreign clinics at random, to ask if PGS would be a good “add-on” treatment.
Five of the 18 clinics were positive about the treatment. Eight said they would only offer it to women over the age of 40 or those who had experienced repeated IVF failures. There is currently no good scientific evidence from trials that it can increase the birth rate among women in these categories.
Only five clinics gave the full picture, saying that they would not recommend PGS because it lacked evidence.
Sebastiaan Mastenbroek, a clinical embryologist from the University of Amsterdam, conducted trials on the first version of PGS and showed it may have lowered birth rates. He told Panorama he was surprised claims were being made for the newer versions of PGS before the current randomised trials are completed.
Panorama asked the Human Fertilisation and Embryology Authority (HFEA), which regulates fertility clinics in the UK, for a response on the subject of “add-ons”. It says it is “concerned about the recent step change in the use of treatment ‘add-ons.’” It told Panorama it has “limited powers to stop clinics offering them nor to control pricing”.
It says, instead, it publishes information directly for patients, so they can have the facts before they go to a clinic and are able to make informed decisions. Next year the HFEA will launch a new website with more information about a wider range of “add-ons”.
Panorama: Inside Britain’s Fertility Business will air on Monday 28 November at 8:30pm on BBC One.
