
On a cold November day, 27-year-old Winnie Sseruma received the news she had been dreading – her HIV test had come back positive. It was 1988, she was living in the US, and her doctor had become so accustomed to delivering this diagnosis, so de-sensitised, that he didn’t even sit down in his chair before he told her. Instead he opened her file and listed off medications.
“Nobody expected me to live,” she tells me over the phone from her home in London, almost 30 years to the day after that diagnosis. It wasn’t just her doctor. Sseruma was so unable to see light at the end of the tunnel that by the summer of 1994, she had booked herself a one-way flight back to her homeland of Uganda. “I just thought: let me die where I want to die.”
But Sseruma, now 57, has defied the early odds. She doesn’t remember the last time she went to a hospital (she only sees her doctor once a year) and no longer tortures herself by replaying the day she believes she contracted it. “I’m choosing to live my life well with HIV,” she says. “I love it.”
[Read More: How it feels to be diagnosed with HIV at 24]
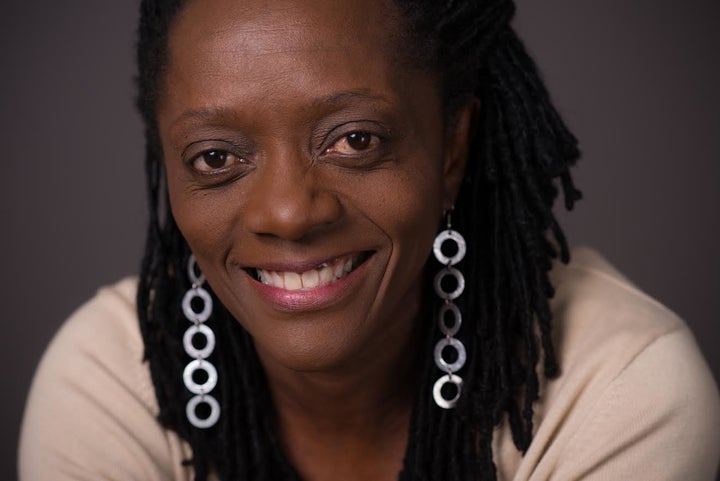
Amanda Mammadova’s diagnosis came in January 2010, when she was 30, and she still hasn’t quite come to terms with the way it was delivered: by a medical receptionist, over the phone, while Mammadova was standing in the middle of her office on her lunchbreak.
The 38-year-old personal trainer from Milton Keynes had only taken the test as a box-ticking exercise – she was trying to join the RAF after a stint in the territorial army and knew her application would involve some element of medical testing, so she preemptively had one done to speed up the process. She never anticipated she might actually be HIV positive.
“My initial thought was: am I going to die? And am I going to die alone? Who is going to want me,” she says. “I’m going to be single forever I need to go and buy 100 cats from somewhere and a cardigan. Within 10 years I’ll be dead.”
Eight years later she has three children, has been through a marriage (and a divorce) and says she couldn’t be in a better place.
[Read More: When I fell pregnant for the first time I was tested for HIV — the result came back positive]
This narrative, this story of the doom and gloom of diagnosis giving way to genuine positivity about a life with HIV, is familiar to Angelina Namiba, a 51-year-old who is originally from Kenya but has lived in London for 27 years.
Namiba was so terrified of finding out her status that when, in 1993, her GP suggested she get tested for HIV (because she already had hepatitis B), she hid the form for the clinic under her bed for six months.
When, eventually, she took the test and got the results, she moved out of her family home there and then, renting a bedsit alone in Chingford so she could keep her diagnosis secret from her mother. She also took a new job in the belief it would keep her busy while she waited to die. “I can’t be sitting in the house looking at the four walls,” she remembers thinking at the time.
“My brother was already very ill with AIDS-related illnesses and the only images of people I’d seen were dying. I’d seen what living with HIV looked like and I was scared,” she says.
Today Namiba has survived 25 years, has a 19-year-old daughter, a career as a charity project manager and is open about her status.
Each of these women have been through unique experiences, but they all agree that HIV does not have to be the death sentence it is often portrayed as in the media. “The stigma has not caught up with the science,” says Namiba.

One of the biggest misconceptions these women lived with was believing they were alone in their diagnosis. “I thought I was the only woman in London with HIV,” says Namiba. “All the images I saw were men.”
Sseruma agrees: “I was hearing a lot about it but not from women’s perspective, it was all about gay men. It came as a shock that as a woman I was being affected by HIV and there was no precedent set.”
Even though she was diagnosed 20 years later, Mammadova says she felt exactly the same. “It’s all well and good being told [by your doctor] there are around 300 people living in Milton Keynes with HIV but I don’t know any of them. I felt very alone.”
She wasn’t. Around 25 per cent of people diagnosed with HIV in the UK are women. The latest Public Health England data shows 4,363 people (3,236 male and 1,125 female) were newly diagnosed in 2017. With 40 per cent of all HIV patients, London continues to have the highest prevalence in the country.
Another myth the women grappled with was believing their positive status meant they faced imminent death – especially for Sseruma who faced a very different prognosis and treatment plan in 1988 to anyone diagnosed today.
“When I was first diagnosed I used to go to a funeral every week,” recalls Namiba. “Friends who hadn’t survived. [I felt] there was no hope for me either.”
“I’d seen the tombstone adverts,” says Mammadova. “I thought I’m going to spend the rest of my life in fear and will be kicked out of society.”
But together these three women have survived a combined 63 years.

They’re not only surviving, but thriving. Science has developed to the point where antiretroviral drugs can now lower the virus to undetectable levels in the blood (less than 40 copies per millilitre). At this point the disease is known as ‘undetectable equals untransmittable’ or U=U.
In short, if the virus is being kept suppressed by medication, you cannot pass it on – either to a sexual partner or to a child in the womb. This advance is what allowed Mammadova and Namiba to give birth to negative status children and all three women to live healthy, successful lives and jobs.
“I always wanted four daughters, and here I am. I was able to realise my dream,” says Namiba. “A lot of people still believe the old messages. If I want to have a relationship or children I can.”
The bigger problem, all three women say, is stigma: people getting HIV wrong and believing a diagnosis means a life of misery – or a life cut short. And it’s a stigma that exists around HIV in a way that it doesn’t around other illnesses.
“Nobody scowls at someone for having breast cancer,” says Mammadova. “But people are still fearful. They think they’ll contract it if I sneeze or share a fork with them. They won’t sit on the same sofa as me.”
“The stigma hurts more than the side effects of the drugs or anything medical. It makes you feel like a leper. I got told by a stranger that anyone with HIV should have it tattooed on their head so people can stay away,” she adds.
Sseruma goes further, saying: “The stigma is what is killing people, the HIV-related stigma. They don’t get tested because they are afraid of being tested.”
What they want you to know is this: a positive diagnosis is not the end of the story. “There is nothing HIV could stop you doing,” says Mammadova. “It used to be the case, but not anymore. People will love you regardless of HIV.”
All three women appear in ‘A Life Beyond’ - a short film about living with HIV, created with support from the Bloomsbury Network at The Bloomsbury Clinic, Mortimer Market Centre, London.
Whether you’re living with HIV, know someone who is, or think you might have put yourself at risk of HIV and need support, you can contact an adviser at the Terrence Higgins Trust to talk. Ring 0808 802 1221.