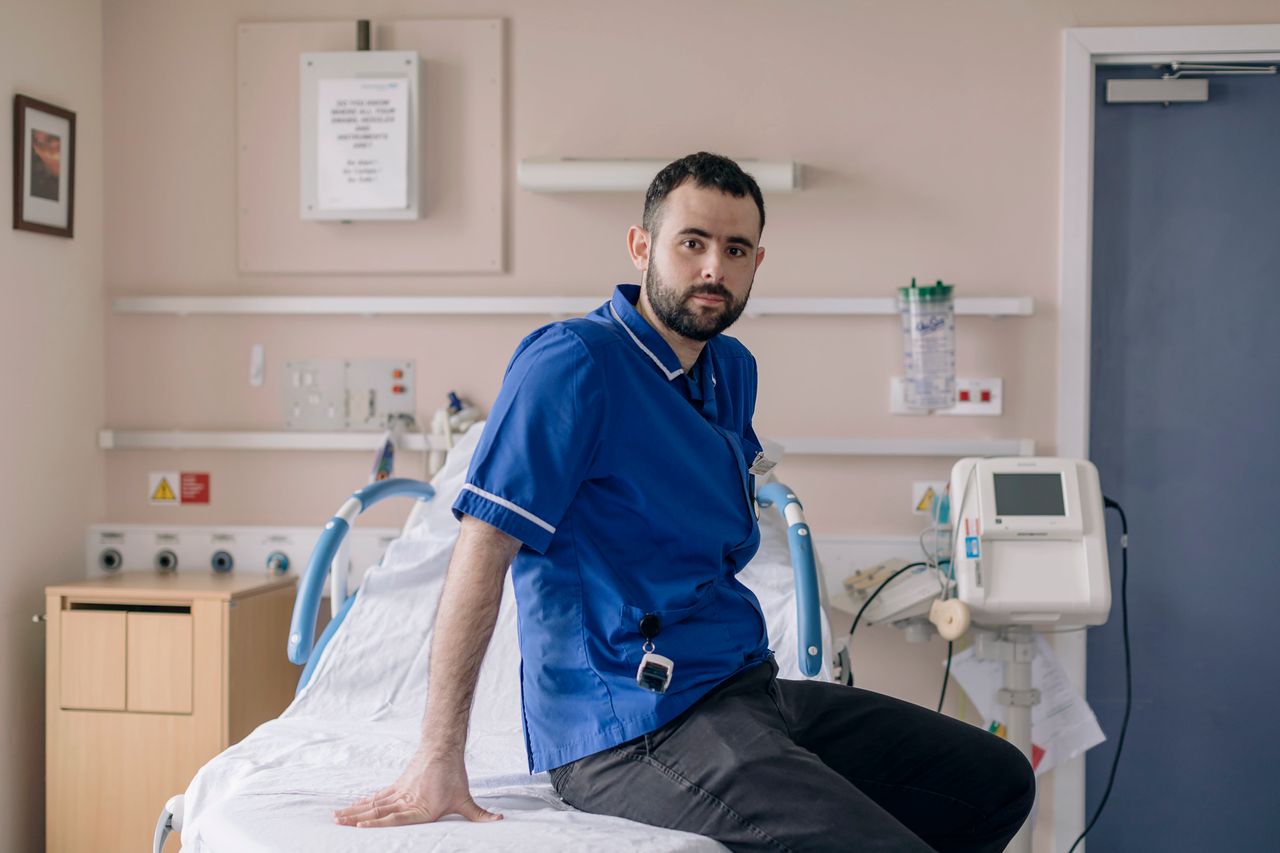
Panos Vakirtzis is a man who clearly loves his job. “I’m the one who welcomes new life into the world, and that’s really special,” says the 27-year-old midwife, who came to Walsall Manor Hospital in the west Midlands from his native Greece just over two years ago.
Yet until surprisingly recently, it’s a job he would not legally have been allowed to do. It was only in 1982 that the Royal College of Midwives dropped its opposition to men entering what had historically been a female-only profession, after years of arguing that such intimate work could only be done by women.
Even now, male midwives still make up less than one per cent of the workforce, and Panos sometimes encounters religious or cultural objections from men to him looking after their wives in labour.
“I try to put myself in their shoes,” he says diplomatically. “I know they need to be encouraged maybe to see that I’m just there doing my job... Sometimes when I go into Tesco’s someone will say “oh, you delivered my baby!” and that’s nice for me, but I don’t really remember them.”
For mothers-to-be surprised to find a man delivering their babies, meanwhile, he’s found the most disarming tactic is self-deprecation. “I know I’m not doing something that’s very common for males to do. I try not be defined by other people, not to follow the stereotype of how you should react because you are male or female.” Recently, reading an article about two Greek women pilots challenging gender stereotypes by flying fighter jets, he was struck by the idea that “we’re doing the same thing, from different angles”.

If changing sexual politics have transformed the role of men in childbirth, however, they have also shaped the expectations of women.
When Alison Edwards first qualified in 1988, initially as a nurse and shortly afterwards as a midwife, mothers-to-be arriving in labour were greeted with a shave and an enema and often the expectation that they’d simply go along with what the doctor said.
Women with high-risk conditions such as heart disease or cystic fibrosis, who these days could be helped safely through childbirth, were routinely told it was too dangerous for them to even attempt pregnancy. Caesareans were rarer - 11.3% in 1989-90, compared to a national rate now of 28% - and so were alternative styles of labour. Alison didn’t see her first water birth until the millennium, and even then it was considered so exotic that she was the only midwife on the team prepared to try it.

It’s a far cry from the birth plans couples are encouraged to draw up today, detailing their preferences in everything from background music to whether the father can help cut the cord (when Alison started out, fathers weren’t allowed in the delivery room).
“I think women know what’s for them now, which is not a bad thing at all. They’re not as submissive as they used to be, which is not a bad thing either,” says the 51-year-old, who now works as a midwifery lecturer at Birmingham City University, training the next generation of NHS staff. “But it can make your job much more challenging. Sometimes you don’t even get a thank you.” Midwives are not, perhaps, held in quite the awe they were.
The work has become more demanding in other ways, too. Thirty years ago, Alison rarely saw an obese mother; now it’s practically a daily occurrence for modern midwives bringing possible complications from high blood pressure and diabetes to practical difficulties in labour. “For the super obese, the operating tables aren’t big enough and the beds only take so much,” she explains.
The turnover on maternity wards is quicker, too. A generation ago mothers would spend three days in hospital recuperating even after a straightforward birth, whereas now they could be home within two hours; as a result, she says, “you don’t get that time to spend with women, to show them how to bath the baby, how to sterilise bottles.”

No wonder some first time mothers leave hospital feeling grateful, but faintly shell-shocked. Only in some of Birmingham’s more traditional Asian communities does she see the old idea of a long confinement at home living on. “They keep up the rituals - if it’s a boy, you are kept in bed for six weeks and you have to eat this kind of sugary stuff to keep your strength up.”
The responsibilities on midwives, too, have increased. These days they must be alert to signs of anything from female genital mutilation - Birmingham Heartlands hospital established its own specialist FGM clinic, after a local midwife spotted cases emerging mainly in the city’s Somali community - to sexual exploitation and domestic violence. “Women have been abused down the centuries, but [a generation ago] I don’t think we would broach it,” says Alison. “Now every time we see a woman, we have to seek an opportunity to ask.”

Panos, meanwhile, describes his biggest challenge on a busy labour ward as staying on top of whatever comes up: “It takes self-discipline, to look after yourself as good as you can, to be always alert when you are at work because you never know what’s going to pass through the door.”
Tellingly, Alison hesitates when asked when the best era was to have a baby. “From the support and one-to-one care you got, probably 30 years ago. But now you’ve got more opportunities open to you, and those who would never in a position to give birth would now be able to, so for those it’s better now.”
The big question for the future, meanwhile, is around staffing levels. The NHS is already short around 3,500 midwives, according to the Royal College of Midwives, and it’s warning of a potential Brexit crunch; although only about 6% of NHS staff come from EU countries, that number was increasing until the referendum. Since Britain voted to leave, the number of new nurses and midwives coming from Europe has fallen by 89%.
Panos, who qualified in Greece before spotting an online recruitment campaign for staff in Walsall, says for now he’s simply trying to put Brexit out of his mind. “Nobody knows what exactly is going to happen. I know the rumours, but I also know that politics and the news is discussions of many things and maybe 1% of these can be true. So I’m waiting until the very last minute to see the plan.”

But he enjoys the way British midwives work, with more autonomy than he sees in Greek hospitals. “There, it’s like ‘I’m telling you what you should do, or telling you to intervene.’ Here the midwives are challenging decisions, they’re discussing what the decisions should be with the patients. Midwives give their opinions and develop a very special relationship with their patients. I think that’s extraordinary.” As for his own career post-Brexit, he shrugs, “I’ll face whatever comes”. It’s what midwives are trained to do.
Midwives’ Pay Struggles
• For almost seven years, midwives’ pay has been effectively capped in the name of austerity. The average midwife’s salary has fallen by about £6,000 in real terms since 2010, according to the Royal College of Midwives, thanks to pay rises below inflation.
• Bursaries for student midwives were scrapped last September, meaning they must now pay up to tuition fees, and starting salaries are currently just over £21,000.
• The government announced proposals in March which would see more than a million NHS workers receive a pay increase of between 6.5% and 29%, if they back the deal. Midwives would be in line to get some of the largest pay increases.
CORRECTION: This piece was amended to swap an estimation of the Birmingham caesarean rate in 1989-1990 for a national caesarean rate.
For more content and to be part of the ‘This New World’ community, join our Facebook Group.
HuffPost’s ‘This New World’ series is funded by Partners for a New Economy and the Kendeda Fund. All content is editorially independent, with no influence or input from the foundations. If you’d like to contribute a post to the editorial series, send an email to thisnewworld@huffpost.com