“Putting them down.”
It’s a pretty odd way to refer to the act of putting your kids to bed. But it’s now a nightly proclamation from my friends and family ― most of whom are in the thick of parenting preschool or school-age children.
“I’ll be over after I put them down.”
“I’ll call you after I put him down.”
“I’ll text you after I put her down.”
It’s the signal to turn off your parent brain and turn on Ted Lasso. To finally sit down after a day of trying to do it all while a few kids hang off you like dangly earrings.
But for me and my husband, Pearse, putting our son, Logan, down each night is the beginning of a 12-hour journey charged with uncertainty and worry.
Logan has a rare form of paediatric epilepsy called Doose Syndrome, also known as myoclonic-atonic epilepsy in a nod to the syndrome’s hallmark seizure types.
For the past eight-plus months, Logan has almost exclusively had nocturnal seizures. But it didn’t start that way.

He had his first seizure out of the blue in the middle of the day Sept. 12, 2022, about a month shy of his third birthday. I was sitting in our parked car outside a market on Cape Cod, when Logan suddenly cried out from the backseat.
The noise he made was a little odd, but it didn’t exactly startle me. After all, he was starting to develop some of his first fears: the dark, things hiding under his bed, monsters. I turned around to see what had spooked him.
I took in his body. Something wasn’t right. His head and eyes were turned up and to the left. His limbs were rigid.
“Logan!” I shouted, trying to get his attention. His eyes were open, but he wasn’t responding to me.
I flew out of the car, yanked his door open, and frantically fumbled with his car seat buckles. Why weren’t my hands working? Everything felt like it was taking too long. Finally, I freed him from the seat and took his stiff body into my arms.
“Help!” I screamed. “Please help!” I started sobbing ― animalistic, guttural cries you can only produce when your mind is trying to keep pace with what you’re experiencing.
The next thing I knew, Pearse was in front of me taking Logan into his arms. Our family members and a few strangers came flying out of the market.
“There’s an urgent care! Right there!” one of the strangers shouted, pointing diagonally across the street. Pearse leapt into our car with Logan while my cousin got in the driver’s seat and sped them to the urgent care centre.
I don’t remember how I got from that parking lot to the urgent care, but I slammed through the front door and bolted to the exam room. Someone had called 911 and the paramedics were already tending to Logan.
“He’s coming out of the seizure,” one of them said.
A seizure.
I’d never seen anyone have a seizure in real life ― let alone my own child ― yet I somehow already knew that’s what it was.
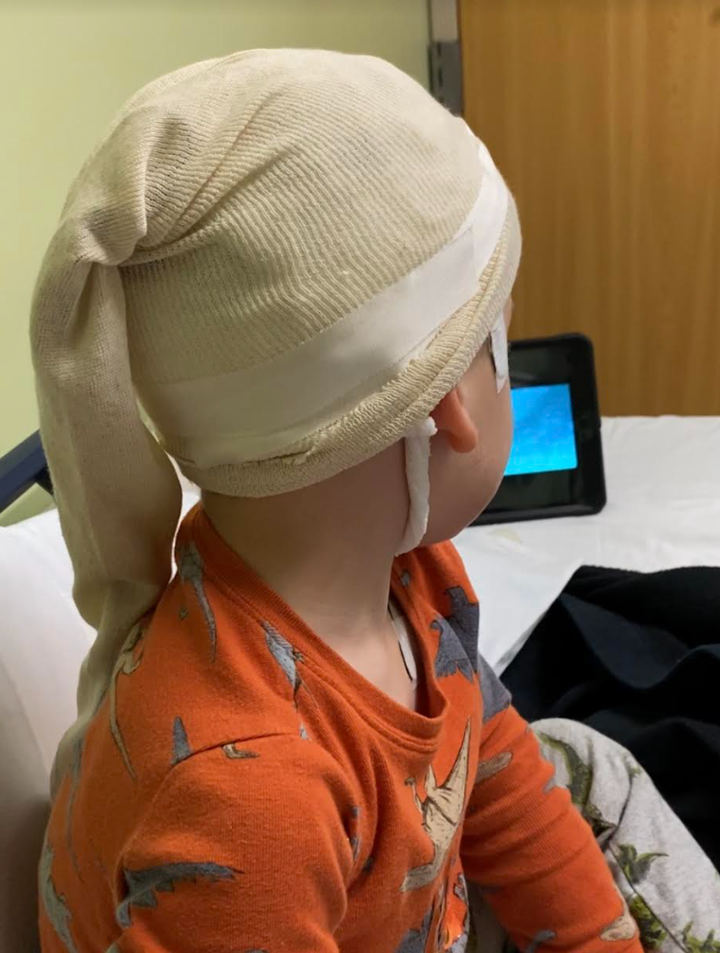
We quickly started to feel like we were drinking water through a fire hose. By Sept. 14, Logan had his first electroencephalogram, typically referred to as an EEG. By Sept. 15, he’d been diagnosed with epilepsy.
That day, he also started taking his first medication: Keppra ― so frequently prescribed to people with epilepsy it was initially described to us as “the Tylenol of anti-epileptic drugs.”
I remember panic-driving to CVS to pick up Logan’s Keppra prescription ― ignoring speed limits and red lights ― thinking once I got this medicine into him, he would never have another seizure.
I hate medicine, but tearing that brown paper bag off the bottle of Keppra, drawing it up into a syringe, and plunging it into Logan’s mouth for the first time brought on an almost-euphoric sense of relief.
But, by Sept. 18, we started noticing new things: seconds-long periods where Logan would stare off into the distance, unresponsive to voice commands or touch; upper body jerks that would sometimes pitch his head, shoulders and arms forward so quickly, he’d fall on his bum.
Then the drops started. Drop seizures, or atonic seizures, are a kind of seizure where a person loses all tone in their body and falls to the ground like a tree in the forest, smashing everything near them on the way down. They’re quick but utterly horrifying.
We’d been strict about screen time up until this point ― only letting Logan watch YouTube videos of Yo-Yo Ma playing the cello.
“Harvard or Yale, buddy?” Pearse would jokingly ask baby Logan, who could repeat his ABCs before he was 18 months old.
Now, as we propped him up in a pillow fort on the couch ― expressionless and exhausted from all the seizure activity ― and turned on the brain-cell-burning singalong that is Cocomelon for the fifth time in a day, that optimism seemed to vaporize.

For months, we watched Logan have thousands of seizures: atonic, myoclonic, absence, atypical absence, tonic-clonic. There are more than a dozen types of seizures, and they all look different.
Most aren’t “Hollywood seizures” –– the kind you see in movies. The majority of seizures aren’t brought on by strobe lights, many don’t feature any convulsions, and some are difficult for the untrained eye to see at all.
Anyone can have a seizure –– and about one out of every 10 people will have one at some point in their life. Beyond that, one in 26 Americans will develop epilepsy.
As we searched for something that would curb Logan’s daily seizure activity, his care team searched for answers. He had a CT scan; a sedated MRI; multiple EEGs, some where he was in the hospital for several days and tethered to monitoring equipment 24/7; blood draws; urinalyses; and a seemingly never-ending lineup of appointments, messages and phone calls with paediatric neurologists, epileptologists, nurses, genetic counsellors and insurance company staff members.
Nothing has yielded a known cause for Logan’s epilepsy; it was ― and continues to be ― a mystery.
By mid-November, Logan was on three medications, and he had two rescue medications on standby in the event he had a seizure longer than five minutes or a cluster of several seizures at once.
Despite those treatments, he was still having hundreds of seizures per day –– sometimes more than one per minute.
Every night, I’d take to the Google-verse, scavenging for any digital scraps of hope I could get my hands on:
Can you outgrow Doose Syndrome?
Chances of becoming seizure-free
Famous people with epilepsy
How long do you have to be seizure-free to get a driver’s license?
As I desperately burrowed through my internet rabbit holes, trying to piece together the potentials and what ifs of Logan’s new future, I began unearthing information about the medical ketogenic diet: a high-fat, ultra-low carb diet that essentially mimics fasting in the body.

I learned that kids with Doose Syndrome are often “super responders” to the diet –– that some become seizure-free on food alone and can eventually ditch all medications.
It wasn’t long before Pearse and I found ourselves getting our formal marching orders from Logan’s new ketogenic diet team at Boston Children’s Hospital. We bought a food scale, moved through educational sessions with Logan’s dietician, stocked up on the necessary staples, started talking to Logan about his new “brain food,” and officially initiated the diet Nov. 28, 2022.
I’m a competitive cooking show super fan, but there is no amount of Chopped or Top Chef that can prepare you for denying a three-year-old of their Annie’s mac and cheese, and instead forcing them to drink 34 grams of heavy whipping cream, then belly up to a meal of butter-drenched shirataki noodles, and a syringe of watered down baking soda (to prevent ketoacidosis).
The morning of Nov. 28, with Pearse at work and Logan angling for my attention, I spent 2 1/2 hours preparing two snacks and a lunch. I filled the dishwasher in one go, using a separate vessel to weigh each ingredient to the tenth of a gram as instructed.
As I tore tiny pieces off a single raspberry to abide by Logan’s carb limit, then stepped back to survey the calorie-dense-but-seemingly-miniscule portions in each container, my eyes filled with tears.
We were warned we’d feel this way but reality hits hard. Still, I thought, if this works, it’s worth it.
It took three long months and lots of tweaks to see real results. But, come March 1, 2023, Logan had achieved daytime seizure freedom as a result of being on a medical ketogenic diet. Today, beyond the diet, he’s still on two medications.
Our life is a parade of syringes and oils and heavy whipping cream and avocados and pill crushers and food scales and ice packs and Tupperware of all shapes and sizes.
When Logan’s in a good seizure-free stretch, it just feels like our necessary rhythm. But when we emerge from a tonic-clonic-filled night, having changed absolutely nothing about his treatment, I admittedly move through the routine that epilepsy has thrust upon us with an unhinged sense of defeat, resentment and anger.
Those are often the days when Logan turns to me randomly and says, “I love you, mama” –– as if he knows I need to hear it.

One day recently, at Logan’s request, I was reading him The Very Hungry Caterpillar. As we approached the double-page feature of all the food the very hungry caterpillar eats, I panicked. He’s frequently confronted by food that doesn’t comply with his diet, but it’s not usually quite as showy as this was about to be.
I turned the page and tried to keep my voice steady as I read the long list of culinary treats. Logan pointed at the ice cream.
“Ice cream isn’t part of my brain food,” he said.
“No, it’s not, buddy,” I confirmed.
“But someday I can have ice cream,” he added. I felt my heart squeeze.
“Yes, someday, bud.”
I now regularly overhear four-year-old Logan very clearly tell the other kids and adults in his life, “I’m on a medical diet because I have epilepsy.” Pride washes over me.
Nothing has ever made me more proud than witnessing the resilience and strength of the young person who grew inside my body, and has now become a force of empathy, bravery and maturity to be reckoned with outside it.
Taking care of a child with a serious medical condition is all-consuming; it simultaneously feels like your highest calling ― your most important work ― and the ice pick that’s chipping away at all the parts of yourself that once made you you.
You can only hope that ice pick is also revealing new nooks, crannies and surfaces you didn’t know you had ― that, in the end, it will offer new depth and reshape you in unexpected, but welcome ways.
And, eventually, someday, like the very hungry caterpillar, you’ll realise you’ve morphed into something new. Something that’s been through the wringer, but emerged beautiful.
I try to keep my sights set on that kind of outcome. But right now we’re still going through it.
Every night, as we turn off Logan’s bedroom light and turn on the baby monitor, we hold our breath, steeling ourselves for the great unknown –– the possibility that we’ll be up and down administering seizure first aid to him every hour on the hour, or that he’ll sleep peacefully and we’ll wake up realising we logged enough consecutive hours to have a dream or two.
In those sporadic dreams I see a world in which conditions like epilepsy are better understood and accurately depicted on the silver screen, rather than over-dramatised and unrecognisable to the people experiencing them in real life. A world where people taking care of medically complex kids have widespread, adequate, easy-to-access support.
And I see Logan, someday in the future, freed of his syringes and oils and heavy whipping cream and avocados and pill crushers and food scales and ice packs and Tupperware. But still very much equipped with the empathy, bravery and maturity this journey has imbued him with ― out there eating all the ice cream he wants, and using all the extra electrical activity now coursing through his brain to set the world on fire.
Melisse Lombard is a writer, editor, content professional and former journalist, now running her own editorial content production company. She lives outside Boston with her husband, Pearse, their son, and their pup. Melisse is also a co-founder of and singer in award-winning professional a cappella group, Sound Off.
Do you have a compelling personal story you’d like to see published on HuffPost? Find out what we’re looking for here and send us a pitch.