The NHS has issued an urgent appeal for black people to sign up and give blood to cope with increasing demand.
The appeal launched following a 75% increase in the amount of Ro blood which was issued to hospitals between 2014 and 2016. Ro blood is a special subtype which is most common in black people.
A high proportion of this type of blood is used to treat sickle cell disease, the most common and fastest growing genetic disorder in the UK.
It is expected that demand will grow even more and the NHS estimates it needs 40,000 new black donors to help save lives.
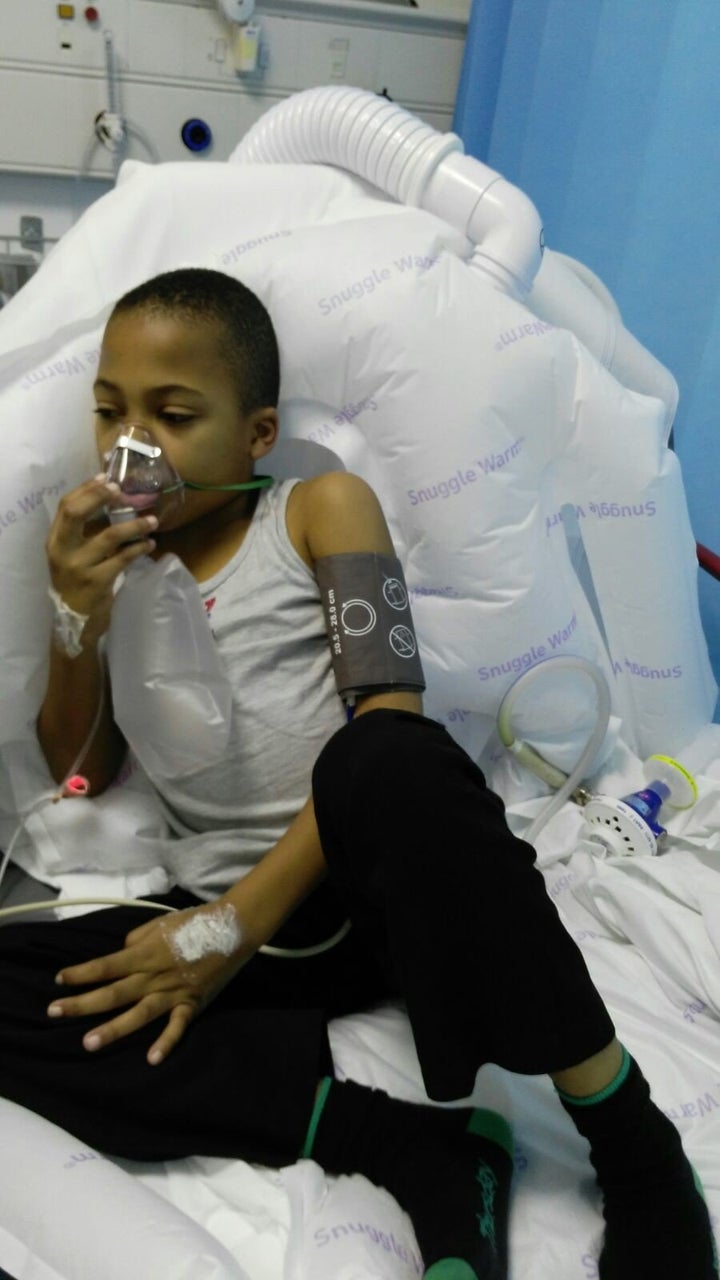
Matthew Akinmuleya, 10, from London, was diagnosed with sickle cell disease at birth. The condition can cause extreme pain, life-threatening infections and other complications such as stroke or loss of vision.
Matthew had his first pain crisis - where sickle-shaped blood cells don’t flow through his veins easily, causing blockages and extreme pain - at six months old. Since his diagnosis he has required a blood transfusion every month.
He is still very ill and in the last six months has been admitted to hospital every month.
His mum Omotolani said: “It’s very stressful and very upsetting seeing your child being in pain every day. He has no break. The hospital tried to see if he could manage without blood transfusions, but he had so much pain.
“The blood he receives makes a huge difference. In the first two weeks after his transfusion he is like a normal 10-year-old. He has energy and is able to go to school.
“But after three weeks, he starts to look pale, jaundiced, tired and pain takes over.”
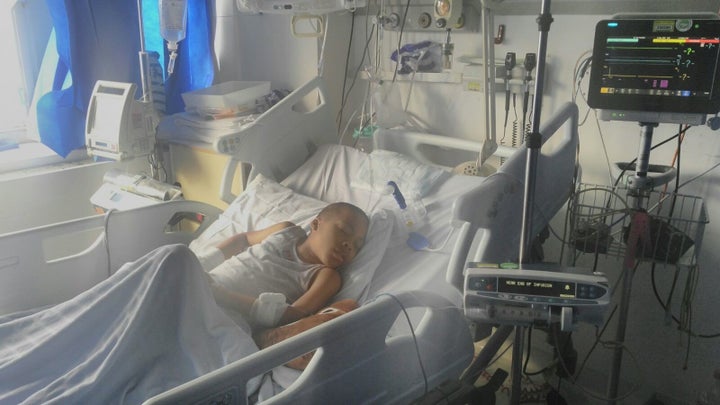
It is estimated that Matthew has received 100 transfusions in his lifetime.
In the week leading up to them, he is often in severe pain which requires him to be admitted to hospital.
“As a mother and carer, I really appreciate all of those who donate,” his mum added.
“My child would not have survived without you. Without this blood, his story would be so different.”
Advancements in the treatment of sickle cell disease mean that patients are living longer and the demand for transfusions is higher than ever before.
Yet, to get the best treatment, patients need blood which is closely matched. This is most likely to come from a donor of the same ethnicity, however currently only 1% of blood donors in England are black.
If patients do not receive blood which has a close enough match, there is an added risk that they can suffer reactions to the donated blood or develop antibodies which make it harder to find matching blood in the future.
Mike Stredder, director of blood donation at NHS Blood and Transplant, said: “Every day, blood donors across the country make a difference; saving people whose lives depend on blood. Whether it is patients receiving treatment for cancer, blood disorders, after accidents, surgery or during childbirth.
“But we need to ensure that we have the right mix of donors and blood types, to help meet the needs of all patients who need life-saving treatment, especially those with conditions like sickle cell disease who require blood which is more closely matched than by group alone.
“In recent weeks, we have been overwhelmed by the numbers of people stepping forward and wanting to donate and show their support for those affected by recent tragic events.
“Thankfully, due to the loyalty of our regular donors, our emergency stocks have proven to be strong and sufficient, but we still need to ensure that we can be there every day, for every patient who needs us.
“Don’t worry if you’ve never given blood before and don’t know what blood group you are – you find out shortly after your first donation. What’s important is that you register as a donor and book your first appointment to donate. By saying ‘I’m there’, you can save the life of someone else, while going about yours.”
To register or book an appointment visit www.blood.co.uk, call 0300 123 23 23 or search for ‘NHS Give Blood’ app.