Last week, the UK government’s scientists declared a new coronavirus mutation first identified in Bristol was being treated as a “variant of concern”.
The so-called Bristol variant became the fourth variant of concern identified by the New and Emerging Respiratory Virus Threats Advisory Group (Nervtag). The other three were found in Kent in southern England, South Africa, and Brazil. All but the Brazil variant are currently known to be circulating in the UK.
In addition, a variant first seen in Liverpool has also now been named as a variant “under investigation”. Variants of concern are all designated “variant under investigation” first, before in some cases receiving the more serious title after consideration by Nervtag.
Virus variants are not unusual or unexpected – but some can cause more concern than others if they appear to be more resistant to current vaccines or transmit more quickly. So why do so many of these variants – under investigation, or of concern – seem to be originating in the UK?
We’re better at tracking them
The UK has one of the world’s highest Covid death rates and its “world-beating” Test and Trace system is, well, very much not – but there is one thing we can be proud of: our genome surveillance capabilities. We are very much the undisputed leader in tracking SARS-CoV-2, the virus that causes Covid-19.
In March 2020, a group of clinical virologists, human genomes experts, epidemiologists and immunologists from more than 30 UK institutions and universities set up a network for genome sequencing called the Covid-19 Genomics UK Consortium (Cog-UK).
Since then, out of the more than 210,000 samples of SARS-CoV-2 genomes that have been sequenced in the world, nearly half have been sequenced by Cog-UK. Genomic sequencing is key to controlling – and ending – the pandemic. It allows us to track the virus’s mutations and scan for new strains. Without it, new strains would be able to spread silently in the population.
“It’s likely we’re just seeing the tip of the iceberg”
Our dominance over the global genome sequencing network (we’ve sequenced about 10 times as many genomes as the next country) means that when a new variant is discovered here, it could purely be due to our scientists doing the most tracking. “It’s like a giant canvas where one corner has been painted in extraordinary detail but the rest is blank,” a New York Times editorial read.
“Surveillance is really good in the UK so we are much more likely to pick up variants as they evolve,” says Dr Deepti Gurdasani, a clinical epidemiologist at Queen Mary University in London. She points to South Africa, another recognised leader in genomic sequencing, where the B1351 strain was discovered. “There’s certainly a bias towards detecting them in areas where surveillance is better. It’s likely we’re just seeing the tip of the iceberg.”
Scientists have even floated the possibility that the B117 or Kent variant may have actually originated in the US – where genome sequencing has been comparatively poor and underfunded – but was merely identified first in Britain.
Professor Stuart Neil, a virologist at King’s College London, agrees that the UK’s “head and shoulders the best in the world” genomic surveillance and sequencing has played “at least in part” a role in the number of UK variants of concern. “A lot of this is about the more you look, the more you find,” he tells HuffPost UK. “It’s a testament to the power of our genomic surveillance that we found these [variants] quickly.”
High transmission rates
As Gurdasani has previously discussed with HuffPost UK, the parts of the globe that have seen new variants arising also have had high levels of transmission. She explains: “Viruses mutate as they replicate, so the more replications the more new random mutations emerge. Most of these mutations have no effect on the virus, but some have a favourable effect on it [from the virus’s perspective].
“As infection spreads from person to person, variants that are favourable to the virus that improve transmission are selected over time. So when you have high levels of transmission, you create conditions for mutations. In the UK, this process of selection which allowed the virus to adapt and become more and more dominant in a population occurred not just on one serendipitous occasion but many, many times in different places.”

In the Brazilian rainforest city of Manaus, where the P1 variant or “Brazil variant” has caused a terrifying second coronavirus wave, Gurdasani points to the high transmission rates where there was a largely unmitigated epidemic for a long period of time. Similarly high levels of community transmission were also seen in South Africa.
Conversely, in places with very low or no levels of infections, the virus has little to no opportunity to mutate. “You’re not going to see variants developing or thriving in New Zealand or Australia,” she continues. “Unless the virus is spreading from person to person at a high level, the virus doesn’t get the chance to replicate and mutate.”
More people with antibodies
Antibody levels in people aged over 70 have more than doubled, according to figures by Public Health England (PHE) published on Friday, suggesting the UK’s vaccination efforts are working. A separate study by the Office for National Statistics (ONS) showed around one in seven people in England would have tested positive for Covid-19 antibodies by mid-January.
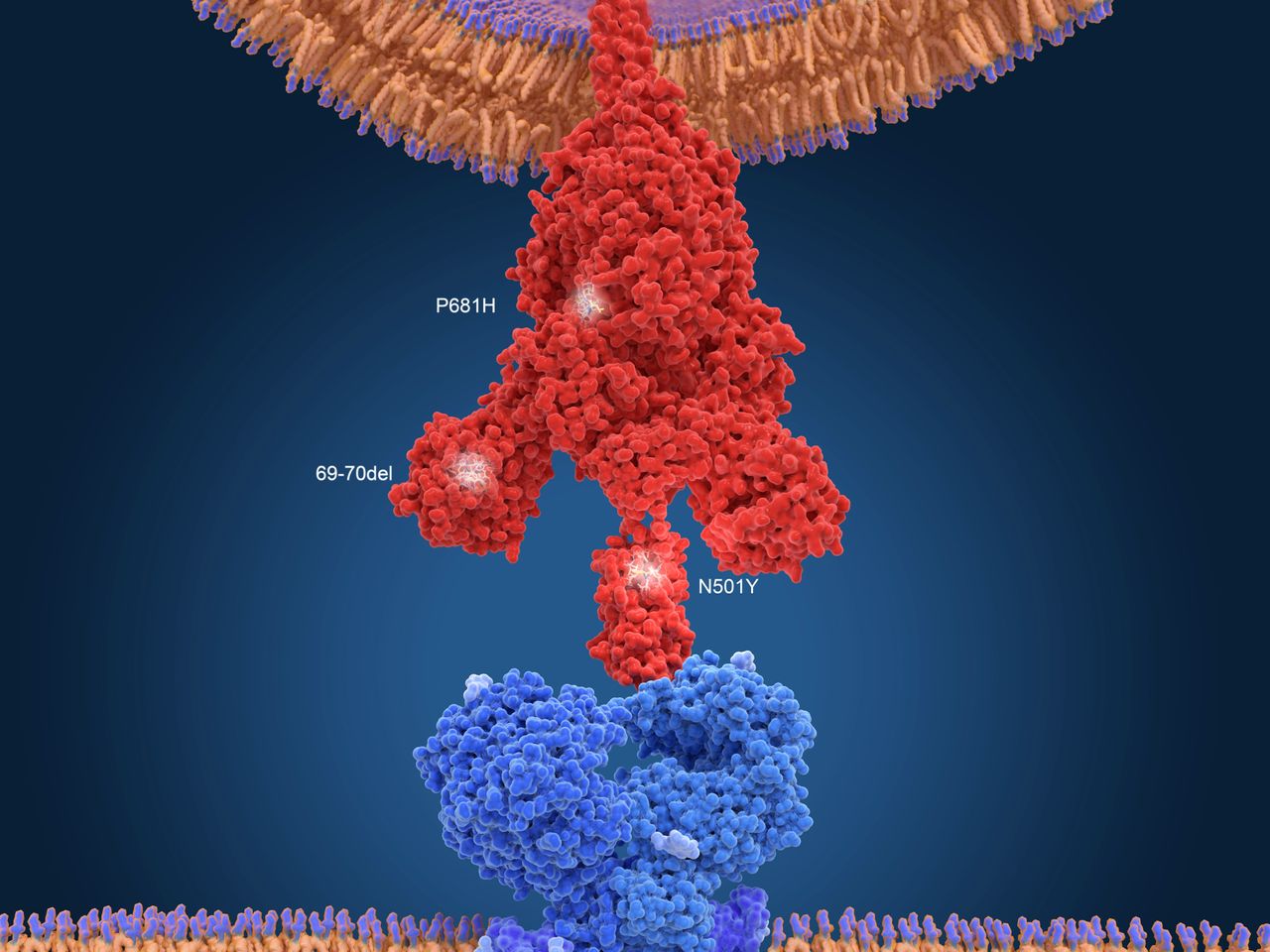
Neil believes this could be one reason why variants have emerged from the UK. “We’ve got very good [knowledge of the] molecular structure of the spike protein [the crown-like spikes that latch the virus onto a cell] of Covid, so we know what parts of that molecule different people’s antibodies bind to. We also know which are the places for antibodies to bind in order to block the virus from getting into the cell.
“The natural conclusion is that these variants are being selected in people who have antibodies against the virus.”
“What we’re seeing is these mutations are arising from parts of the spike protein known as the epitope that antibodies bind to. The bit of the protein that actually interacts with the cell and allows it to get in in the first place is changing, and those changes are making some of the antibodies that target those sequences work less well.”
In other words, these new variants could be emerging as a result of these antibodies. “We don’t know for certain, but when you see what’s happening the natural conclusion is that the reason these variants are growing out is that they are being selected in people who have the antibodies against the virus.”
The case of the P1 or Brazil variant appears to substantiate this idea. First discovered in Manaus in December, the variant has since troubled scientists who had previously believed the city – which saw about 80 recorded coronavirus deaths each day in May 2020 – had reached a level of herd immunity during the first wave.
About 75% of Manaus’ population had already had coronavirus prior to the emergence of the new variant and should already have a certain level of antibodies. Yet the resurgence of Covid-19 has led to hospitals in the northern city once again running out of beds and oxygen.
If these variants are emerging in places where people already have antibodies, could this mean the next variants of concern could come from countries like Israel, which has vaccinated more than 40% of its total population? Neil believes it is “perfectly possible”. “To a certain extent, you can use that as a half-full aspect of knowing [a country’s] interventions are clearly working, because these viruses are being selected out.”
Gurdasani believes this could also mean we may likely continue to see serious variants coming from the UK. “If variants are emerging due to immune selective pressure from antibody treatments and if levels of transmission are not brought down, then I would be surprised if that didn’t happen.”
Treating Covid-19 patients
A fourth possible factor – and Neil stresses there is “no evidence yet to say this is definitely the case” – is that these strains could be coming from people who are severely sick with Covid-19 or who are heavily immunosuppressed.
These patients are given a convalescent serum (the part of blood that contains antibodies that should block infection) taken from people who have already recovered from the virus, to help them clear the illness. “One of the issues is that the screening of these convalescent sera is not done very well,” he says.
Instead of using viral neutralisation tests, scientists are regularly checking a serum’s antiviral properties using surrogate tests. Surrogate tests only accurately show the presence of antibodies and not always their amount or magnitude.
Neil believes this is leading to some patients being given a lower concentration of antibodies. “To use an analogy, it’s exactly the same as what would happen if you gave someone a half dose of antibiotics. It’s possible some of these mutations we’re seeing are selections of the virus that are more resistant to the serum that’s gone into these patients, and then escaping inside people and infecting hospital staff and spreading out that way.”
It’s “certainly a plausible possibility” that this is how new variants are emerging – although patients given convalescent serum are treated by hospital staff wearing a high level of personal protective equipment (PPE).
“What we do know is that if you do a very controlled and contrived experiment in a lab with a completely different virus in which you’ve cloned the spike protein of SARS-CoV-2 to minimise the risk of anything going wrong, and you try and select that virus to become resistant to certain specific antibodies, then you end up selecting most of the same mutations that you see in these variants.”
The fact that new variants are becoming increasingly resistant to the serum isn’t necessarily something we need to “crap ourselves” about, he says. “We need to put things in a bit of perspective: some of these mutations have lost their sensitivity to a certain antibody but most people respond with a range of different antibodies, so they should be fairly well protected once they’re vaccinated.
“We’re talking about death by a thousand cuts, and by then we’ll be updating vaccines periodically to take into account the variations.”
Should they be renamed?
Former US president Donald Trump was (rightly) criticised by the international community for his insistence on calling coronavirus the “China virus” or “Chinese virus” during his time in office. Such phrases were discriminatory, racist and led directly to the rise in anti-Chinese and anti-Asian abuse across the US and Europe.
“We shouldn’t really name them after where they were first detected. There’s a level of prejudice that comes with that.”
The same could be argued in naming coronavirus variants based on where they were first identified. “This label apportions blame. This label says loud and clear: South Africa is a source of a threat,” writes Steve Miller, head of the charity Save the Children in South Africa. There’s the added fact that variants are not necessarily identified in the area they first emerged.
Similarly, the people of Kent may fairly worry about how the B117 variant’s potential impact on the reputation of the Garden of England. “We must accept that damage has been done to the Kent brand,” a Tunbridge Wells resident told a local paper. “While people’s memories are often very short, the internet’s isn’t and there’s the risk Kent will be synonymous with the variant.”
Neil agrees. “It’s a useful shorthand but we shouldn’t really name [the variants] after where they were first detected. There’s a level of prejudice that comes with that.”
