doctors
Key legislation you may have missed amid the Rwanda bill row.
"I didn’t realise this was real."
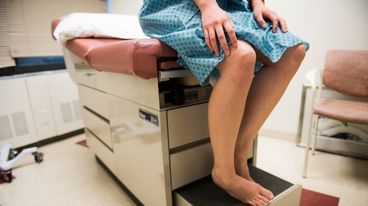
"As I stood mostly naked under her gaze, I became a problem, not a person."
Life is too short not to allow yourself an occasional indulgence, these physicians say.
Unfortunately, my experience is all too common. If you find yourself in a situation like I did, here's what you should do.
Wes Streeting admitted it's "uncomfortable" to discuss their own inflated pay.
So MPs asked for thousands for their second jobs, but junior doctors start on just £14 an hour?
There's a "social contract being pulled from under doctors’ feet”, according to an NHS surgeon.
There isn't an instant fix, but here's what the pros do to feel better when they're sick.
A new league table 'names and shames' surgeries, but doctors say it's not that simple.