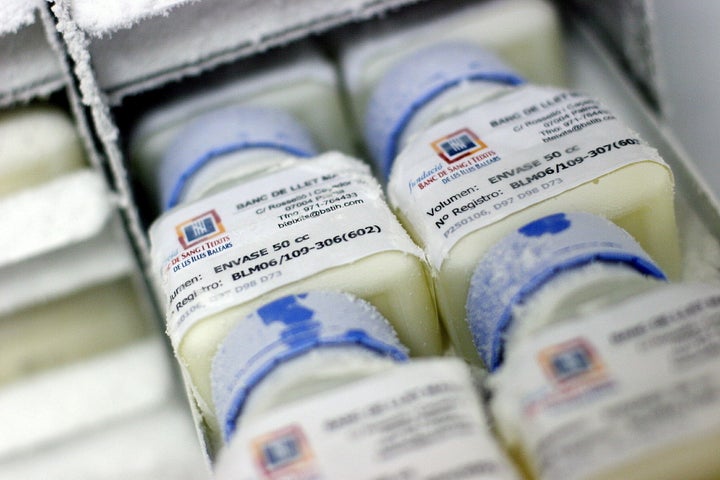
Almost half of babies breastfed at birth are supplemented with formula milk in hospital. Supplementation can sometimes be vital, but many babies end up having supplements for non medical reasons, with those who are supplemented with formula less likely to go home breastfed. Early supplementation can interfere with milk supply and decrease maternal confidence.
So what if we stopped using formula when babies needed extra milk?
We are of course not talking about babies starving or becoming severely ill, but rather using donor human milk (DHM) as a supplement instead of cow milk-based formula.
In the UK, parents of extremely premature babies (born under 30 weeks) will usually be offered DHM if their mother is unable to express, or express enough of her own milk. The milk is donated to specialised human milk banks by breastfeeding mothers who have extra milk. Mothers are screened with questionnaires and blood tests, the milk is pasteurised, and strict monitoring steps for contamination in place. For these babies, receiving human milk over formula can be lifesaving, decreasing the risk of necrotising enterocolitis (where the gut is wholly or partially destroyed), breathing and eye problems, and cutting their stay in hospital and, increases the chances of mothers establishing their own milk supply.
Babies might need supplementation if they have lost a lot of weight after birth. NICE guidelines state that mothers should be supported to maximise their own milk supply, but sometimes additional milk is needed whilst this happens. Case studies show that using small amounts of DHM instead of formula reduces hospital stay and supports breastfeeding, by feeling like a bridge for mums to establishing their own supply.
And what about babies who will never be breastfed because their mother has had a mastectomy, needs chemotherapy or is taking a lifesaving medication incompatible with breastfeeding? Many want their baby to have breastmilk and some source milk from friends, family, or even strangers. This brings the risk of not necessarily knowing the donor’s health background and potential contamination. What if these babies could have DHM instead?
Even a few days of breast milk helps protect babies, predominantly due to its species-specific immune function properties that formula milks do not contain. DHM is pasteurised to kill off contaminants, but pasteurised donor milk still contains many of these components, including lactoferrin which helps iron absorption, lysozyme which destroys bacteria, and large numbers of immunoglobulins.
It would also help protect the microbiome. We all have trillions of ‘good and bad’ bacteria in our digestive system. Simplifying things somewhat, the more good bacteria, the lower our chances of obesity, asthma and bowel conditions. Our first milk feeds help seed our microbiome. Although more research is needed, human milk helps certain types of bacteria (e.g. Bifidobacterium) to flourish, possibly protecting babies against allergies. Babies who are given formula have very different microbiomes.
This switch need not be prohibitively expensive, especially given the known cost-savings of increasing breastfeeding rates. A 50-ml bottle of DHM costs around £7.50. In a limited study where babies who had lost weight were supplemented with 10 ml of formula, this typically happened just a few times a day for two days. Even preterm babies receiving donor milk only need it for five days on average until their mothers establish their own supply.
Some worry that expanding provision would lead to a lack of availability for very premature babies. DHM has had to be rationed because of a lack of sufficient milk bank services to process it and recruit donors. With the right systems scaled up, supplies do not need to be limited. We’d need to work out how we were going to enable more mothers to donate. Ethically, fairly, and easily. There would need to be government or philanthropic funding to scale services. But there’s certainly a will between mothers to make sure more babies get milk - informal milk sharing social media pages have tens of thousands of members.
And now we have a Foundation that wants to make this a reality for all families who need it. The Human Milk Foundation aims to ‘create a future where more babies can have access to screened donor milk when their own mothers cannot produce milk, or need time and support to get there’. The first step was to set up the UK’s first independent, non-profit human milk bank, the Hearts Milk Bank, founded by Dr Natalie Shenker and Gillian Weaver. It grew rapidly, supplying donor milk to hospitals, then due to donated supply outstripping hospital demand, to families in the community, supported by a health professional, and free of charge to the family.
The outcome? Over 25 babies have thrived. Where the donor milk was used to support the mother to establish her own supply, most mothers overcame their challenges and breastfed. Many are still feeding their babies now. All express just what a difference being able to receive donor milk made to their families.
Families like Koan’s. Koan has a genetic condition that meant he developed seizures that worsened with infections. His mum had very low milk supply during the time he was in hospital. From the age of two months, he received five weeks of DHM supplements and lactation support from the HMF. His mother managed to establish exclusive breastfeeding, and Koan has not been readmitted since. He is still breastfed and thriving at 16 months.
Now who’s going to help us change more families lives for the better?