
I was addicted to prescription painkillers before I turned twenty.
That truth always catches me off-guard; I grew up in a rural countryside area, had never even seen drugs, let alone take them recreationally. And yet I ended up dependent on opioids for a decade.
It began at 18 when I woke one morning in an excruciating, screaming-into-a-pillow kind of pain. I’d never had very good health but this was different. Over the next few weeks I was in and out of hospital and the GP because I was in so much pain. I couldn’t cope.
But no one could figure out what was wrong with me. Whether it was because the doctor finally believed me or just wanted me to go away, eventually he prescribed me a strong painkiller (opioids) that dulled the pain enough for me to get through the day. That may sound dramatic, but that’s because it was.
“The painkillers caused unpleasant side effects like weight gain and extreme tiredness, but that was nothing compared to the pain I would be in without them”
Overnight my life had changed, but I had no idea just how much. Weeks, then months went by; appointment after appointment, and still no-one could identify the cause of my pain. The painkillers caused unpleasant side effects like weight gain and extreme tiredness, but that was nothing compared to the pain I would be in without them. If I was even an hour late taking my painkillers I would start shaking or get a fever.
I started university and learned to cope with the pain by taking painkillers and staying in bed a lot. Before I knew it, coping meant a wheelchair and round the clock care. But I kept believing I would get better in a week, or a month, or a year. I kept going, and I kept hoping.
I knew the painkillers I was taking were strong, but I was ignorant of how addictive they were and how long-lasting the side effects could be. All I knew was I was desperate and couldn’t cope with the pain.
The amount and strength of painkillers I was taking increased as time went on. Nurses, doctors, consultants would all gasp when they heard the level of medication I was on – one doctor going so far as to refuse to give me what my GP had already prescribed. He told me he was so uncomfortable giving someone my age that amount of painkillers.
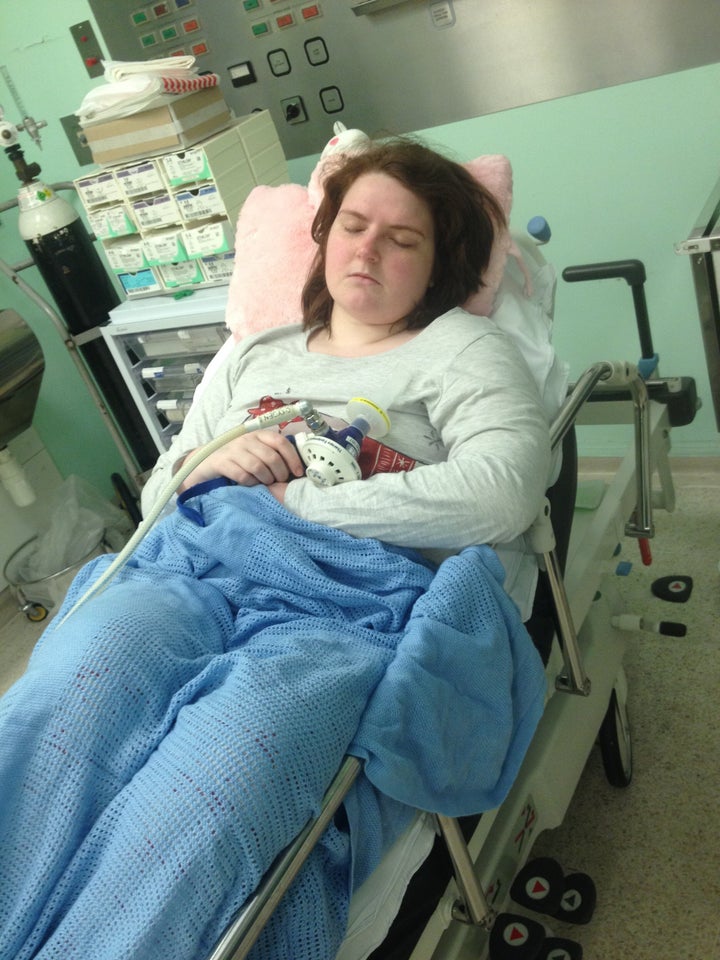
What I didn’t know was, when you take opioids for a long time, they have unseen side effects too. In 2013, I found myself in and out of hospital. And the problem this time was being caused by the medication. The opioids had now become more of a problem than the reason I was taking them. Every doctor I saw told me I needed to come off the painkillers, and each time I cried. I was in so much pain that I needed more, not less. What I didn’t understand then was that the painkillers had stopped working.
You see, opioids work well for a short amount of time on acute pain – they don’t work well on chronic pain. Instead, I had become stuck in a cycle. I’d take a dosage of painkillers which would work for a short amount of time, but when they stopped working I’d need a higher dose to achieve the same effect. I went through this cycle several times, and now the opioids had caused long-term effects. I had no idea this could happen to me.
I’m not the only one. Chronic pain affects 28million adults in the UK. The Department of Health reported that prescriptions of opioids in England and Wales have risen by 60% in a decade, but there remains no support, not even a leaflet to advise you on how to get off them. Most doctors agree opioids are not a solution to this issue, as Dr Cathy Stannard, a consultant in pain medicine has found. “Fewer than one in ten people that are taking them for pain will experience a reduction in pain,” she said. “They are on a medicine that’s not helping but they are on a medicine that’s causing many harms.”
The opioid problem is something even the health secretary, Matt Hancock, has commented on. He said “we must act now to protect people from the darker side of painkillers.” But so far he has only announced that opioids should carry warning labels. Meanwhile, most patients, and even GPs, are ignorant of the reality of withdrawing from painkillers.
“I made the decision to come off the painkillers, a journey that would take me years. Without any help or advice, I was left to navigate these unknown waters myself”
I made the decision to come off the painkillers, a journey that would take me years. Without any help or advice, I was left to navigate these unknown waters myself. I was worried about not being able to cope with the pain. I had ended up in unbearable pain many times, the thought of reliving that was terrifying. I was scared that if I tried reducing my painkillers and couldn’t cope that I wouldn’t be able to up my dosage again. It seemed unlikely that another doctor would be willing to prescribe that amount of medication. I didn’t feel like I had any choice but to try reducing my dosage, given how bad the side effects had become. If I wanted things to get better, I knew I had to give it a go.
I’d lower my dosage, and fevers, uncontrollable shaking, vomiting and pain all over my body would follow. The worst part was being so exhausted yet unable to sleep because your body is crying out for the painkillers. That was when I was close to giving up.
I found it hard to eat because I had stomach cramps and constantly felt nauseated. The symptoms were most extreme in the first week but they often lasted for months. Paul took time off work to look after me, but even so I often felt scared and alone. I was so unwell and weak, I was scared of how much worse I could get. I found it hard to believe I would get better. I didn’t want to tell the people around me because I didn’t think they would believe how awful withdrawal was. Once I was back to ‘normal’, I’d repeat the process and lower my dose again.
I didn’t understand why it was so hard, GPs dismissed me as dramatic. One day I was watching a documentary about the opioid crisis in America in which they described oxycodone as “medical heroin”. Shocked, I checked my painkiller boxes and, sure enough, there was oxycodone written on the side. Suddenly what I was putting my body through – and why it felt like I lost my mind every time I did a reduction – began to make sense.

If I could go back in time, with the hindsight of all I know about opioids now, I wouldn’t make different choices – because I couldn’t make different choices. My GP didn’t hand over my prescription lightly. Pain specialists have waiting lists that are years long. And instead of investing more in pain management programmes, the NHS has only made cuts.
Early intervention could have taught me skills of how to manage pain without painkillers. I was the result of a short-sighted view to prescribe painkillers to patients, instead of giving them pain management treatment. Painkillers did not solve my medical issues. Instead they just dulled the pain until the problem resurfaces another day.
At times, the only thing that would keep me going was my faith, and my husband, Paul. During withdrawal I felt weak physically and mentally. In the middle of the night I would cry out to God to get me through the next hour, and then the next, until morning. When I wanted to give up, Paul reminded me what I’d already achieved and tell me I could do it. And I did.
If I can do it, I know that others can too, with the right support. Having done my own research, I know it is possible to temper the symptoms of withdrawal and educate patients on what to expect. Unless there is some serious investment in pain management and opioid withdrawal, with an ageing population, the opioid crisis is only going to get worse, with repercussions unknown.
Katie Bennett-Davies is a writer living with chronic pain. Follow her on Twitter at @kbennettdavies
Have a compelling personal story you want to tell? Find out what we’re looking for here, and pitch us on ukpersonal@huffpost.com