palliative care
Palliative care and hospice professionals discuss what the process is like — and their insights may challenge what you think about dying.
Emma Clare has an unusual job, offering practical and emotional support to dying people and their families.
"It's like Christmas every day."
Kevin Fong's BBC2 doc asks: does quality or quantity of life matter more?
NHS England seems to be signalling they don’t particularly care where people die or how people die. It’s as if once illness becomes no longer treatable you are no longer a priority
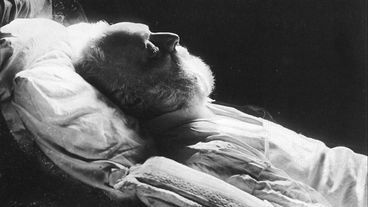
'Dad enjoyed this so much.'
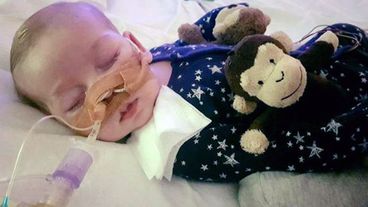
A year on, all those caring for seriously ill children are still reeling from the impact of negative social media coverage and the deepening myths about children’s palliative care
'It's the only leading cause of death that we can’t cure, prevent or slow down.'