The Pfizer/BioNTech Covid-19 vaccine has been approved for use in the UK, with rollout beginning as early as next week.
The UK is the first country in the world to make the historic move – but how will it be distributed and who will get it first?
What’s in the pipeline for the UK?
The government has secured 40 million doses of the Pfizer/BioNTech vaccine, with 10 million due in the UK by the end of the year.
Patients need two doses, meaning not enough shots have been secured for the entire UK population, PA Media reports.
Health Secretary Matt Hancock told BBC Breakfast on Wednesday that 800,000 doses of the vaccine will be available next week, with “several millions” more coming throughout December.
He said: “We’ll then deploy at the speed that it’s manufactured, and the manufacturing is, of course, being done by Pfizer in Belgium, so that will determine the speed at which we can roll it out.”
How will a vaccine be rolled out?
Work has been going on behind the scenes to ensure that NHS staff are ready to start delivering jabs to the most vulnerable, as well as health and care workers, as a priority.
Matt Hancock told Sky News there would be “three modes of delivery” of the vaccine.
“The first is hospitals themselves, which of course we’ve got facilities like this,” he said.
“Fifty hospitals across the country are already set up and waiting to receive the vaccine as soon as it’s approved, so that can now happen.
“Also vaccination centres, which will be big centres where people can go to get vaccinated. They are being set up now.
“There will also be a community rollout, including GPs and pharmacists.”
The NHS Nightingale Hospitals have also been earmarked as sites for mass vaccination clinics – among other uses.
In addition, NHS leaders have said there will be “roving teams” deployed to vaccinate care home residents and workers.
Based on the current information, the vaccines being developed require two doses per patient, with a 21 to 28 day gap between doses.
New regulations allowing more healthcare workers to administer flu and potential Covid-19 vaccines have also been introduced by the government.
Who is top of the list to get a coronavirus vaccine?
The health secretary told Sky News that the Joint Committee on Vaccination and Immunisation (JCVI) set out its priority list on Wednesday.

Don’t vaccines take a long time to produce?
In the past it has taken years, sometimes decades, to produce a vaccine.
Traditionally, vaccine development includes various processes, including design and development stages followed by clinical trials – which in themselves need approval before they even begin.
But in the trials for a Covid-19 vaccine, things look slightly different. A process which usually takes years has been condensed to months.
While the early design and development stages look similar, the clinical trial phases overlap, instead of taking place sequentially.
And pharmaceutical firms have begun manufacturing before final approval has been granted – taking on the risk that they may be forced to scrap their work.
The new way of working means that regulators around the world can start to look at scientific data earlier than they traditionally would do.
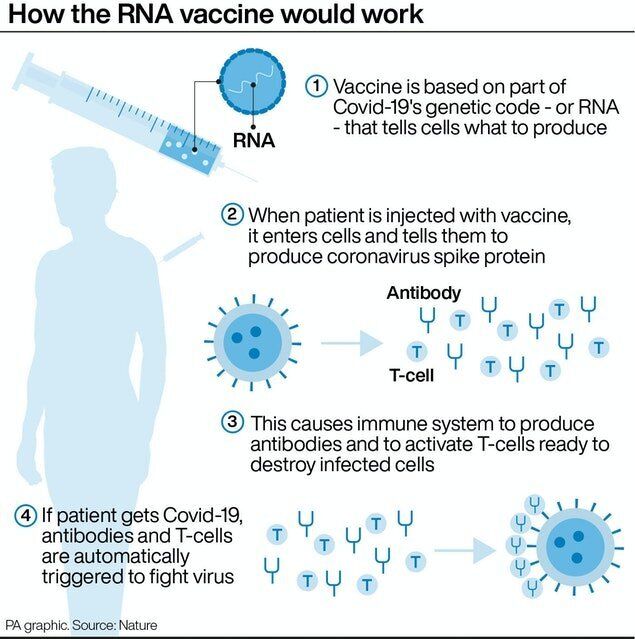
Aren’t there other vaccines?
Yes, recent data from the Oxford/AstraZeneca, and Moderna vaccine trials suggests their candidates also have high efficacy.
Oxford data indicates the vaccine has 62% efficacy when one full dose is given followed by another full dose, but when people were given a half dose followed by a full dose at least a month later, its efficacy rose to 90%.
The combined analysis from both dosing regimes resulted in an average efficacy of 70.4%.
Final results from the trials of Moderna’s vaccine suggest it has 94.1% efficacy, and 100% efficacy against severe Covid-19.
Nobody who was vaccinated with the vaccine known as mRNA-1273 developed severe coronavirus.
Which jab is best?
The early contenders all have high efficacy rates, but researchers say it is difficult to make direct comparisons because it is not yet known exactly what everyone is measuring in the trials.
How many doses has the UK secured?
The UK has secured access to 100 million doses of the AstraZeneca/Oxford University vaccine, which is almost enough for most of the population.
It also belatedly struck a deals for seven million doses of the jab on offer from Moderna in the US.
The deals cover four different classes: adenoviral vaccines, mRNA vaccines, inactivated whole virus vaccines and protein adjuvant vaccines.
The UK has secured access to:
- 100 million doses of the Oxford vaccine
- 60 million doses of the Novavax vaccine
- Some 30 million doses from Janssen
- 40 million doses of the Pfizer/BioNTech vaccine – the first agreement the firms signed with any government
- 60 million doses of a vaccine being developed by Valneva
- 60 million doses of protein adjuvant vaccine from GlaxoSmithKline (GSK) and Sanofi Pasteur
- Seven million doses of the jab on offer from Moderna in the US.
What do they cost?
Pfizer/BioNTech is making its vaccine available not-for-profit.
According to reports, the Moderna vaccine could cost about 38 dollars (£28) per dose and the Pfizer candidate could cost around 20 dollars (£15).
Researchers suggest the Oxford vaccine could be relatively cheap to produce, with some reports indicating it could be about £3 per dose.
AstraZeneca said it will not sell it for a profit, so it can be available to all countries.
However, the details of the deals made by the UK government have not been made public.
How do we know the vaccines are safe?
Researchers reported their trials do not suggest any significant safety concerns.