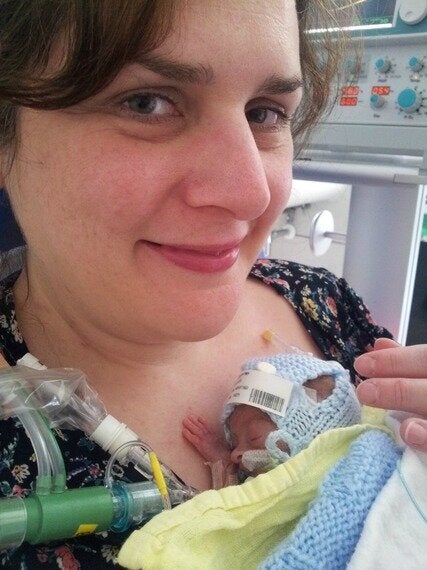
My son Hugo died in my arms in March 2014 aged 35 days.
He was born when I was just 24 weeks' pregnant because I had the rare, life-threatening pregnancy complications HELLP syndrome and preeclampsia. The day before Hugo's birth, I had been transferred to a specialist hospital two hours away from my home.
There is nothing I can fault in the clinical care either Hugo or I received.
There is nothing that can be done to bring Hugo back.
But there were many issues surrounding communication that could have prevented further stress in an already heartbreaking situation.
Hugo's Legacy is about helping other women who suffer birth trauma, other families with a baby in neonatal care, and parents who lose a baby. Anyone who experiences any of these things deserves compassionate care, and a streamlined system that enables people to get the support they need, rather than battle against it.
That's why I have these things to tell the National Maternity Review which is assessing current maternity services, and consider how services across the country should change to meet the needs of women and babies.
So this is what I would like the National Maternity Review to know:
That every woman is individual.
That evidence is vital in the context of providing safe care. But to recognise that evidence cannot tell you everything. Each woman, each situation needs to be considered according to its own merits.
Postnatal care - Hospital
That any new mother separated from her newborn baby for clinical reasons, as Hugo and I were, should be reunited as soon as it is clinically possible.
That no new mother should be left in an intensive care bed, her baby in the neonatal unit fighting for his life, feeling that she is the least important patient on that ward.
There should never be a delay due to interdepartmental squabbling about beds, and to which department the responsibility of taking the mother to see her baby belongs. (This happened to me in intensive care).
That postnatal wards need to have a greater awareness of the needs of mothers whose babies are being cared for in a neonatal unit. It is difficult enough for us being on a ward with women who have their babies with them.
Please don't delay us visiting the neonatal unit to see our babies because of a lack of coordination between maternity and neonatal about timing of rounds.
Please don't force us to make our own meal arrangements because the food that is provided sits getting cold on a tray next to our postnatal bed, while we are spending precious time with our baby.
Postnatal care - Community
That better consideration needs to be given to the postnatal care needs of mothers whose baby is in neonatal care, especially when the woman has been transferred to a specialist hospital away from home. The pathways need to be clear, sensible, and appropriate staff aware of them.
For example, at first I was told I would need to make the four-hour round trip to see my own GP - impossible. Then I was told I would need to register with a local GP - challenging. Eventually I was able to see a community midwife at the hospital.
Support for Birth Trauma and Bereavement
That no bereaved parent should return home with empty arms and feel cast adrift from the hospital. To have to find their own support. To have to make telephone call after telephone call explaining an illness they do not yet quite understand and have to say the 'D' word again and again. To feel like such a failure as a woman and as a mother. To have to relive everything that happened again and again because services in the 21st century seem not to find the capability to communicate with one another.
That there is support for women who have experienced birth trauma, and for bereaved parents, but people need to know about it - professionals need to know about it so they can direct parents accordingly. Let's use some of that 21st century communication capability to close those circles, make those connections.
That when a woman makes a complaint about her care, (or feeds back about her care in any way) they are listened to respectfully. That they are made to feel like a human being with emotions with a response that includes words like 'sorry' where appropriate. That they do not receive a response that feels like a report to the trust board, a box ticked. That they are reassured learning has been made so no other woman has to suffer the same upsets, the same heartbreak, the same trauma. The same nightmares.
No mother should ever be told by a panel of consultants their recommendation to 'withdraw treatment' for their child while that same panel of consultants stands, mouth agape as the mother lies crumpled on the floor, sobbing as though her heart has been ripped out of her chest. Which it has.
No mother should have to be told dismissively "all mothers feel guilty", as if that is a salve on their pain.
No mother should have to read in a referral letter inaccuracies about the details of her son's life and death, and for the GP who wrote it to phone her to apologise with the excuse that they did not read her notes because they were 'too busy'.
No mother should be made to feel like she is abnormal because of what the trauma of her own life-threatening illness and grief over the death of her son has done to her mind. Instead, she should receive compassionate support to help her understand, and live with the trauma.
This is part of my story, a snapshot of my life and experiences since February 2014.
There is nothing that can be done to undo what happened to me, or to Hugo. There is nothing that can be done to bring Hugo back.
But there are things that can be done to prevent other women suffering such unnecessary additional upset and torment.
That is why I would like the National Maternity Review to read, to listen, and to take account of my experiences.
In Hugo's memory.
Image blogger's own.
For more posts like this, visit Leigh's blog at Headspace Perspective.